Impact of Anthropometric Measures on Distal vs Conventional Radial Access for Percutaneous Coronary Procedures
- PMID: 39898346
- PMCID: PMC11782795
- DOI: 10.1016/j.jacadv.2024.101565
Impact of Anthropometric Measures on Distal vs Conventional Radial Access for Percutaneous Coronary Procedures
Abstract
Background: Results from the Distal vs Conventional Radial Access (DISCO RADIAL) trial confirmed distal radial access (DRA) as a valid alternative to conventional transradial access, with equally low rates of radial artery occlusion (RAO), yet higher crossovers but shorter hemostasis.
Objectives: The purpose of the study was to investigate whether patient anthropometric measures influence the effect of randomized access on key secondary outcomes.
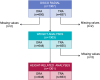
Methods: DISCO RADIAL was an international, multicenter, randomized controlled trial in which patients with indications for percutaneous coronary procedure using a 6-F Slender sheath were randomized to DRA (n = 650) or transradial access (n = 657) implementing best practices to reduce RAO. The primary endpoint of the trial was incidence of forearm RAO, which was extremely uncommon. Secondary endpoints, including sheath insertion time, radial artery spasm, crossover (failure to obtain access through assigned access site), hemostasis time, and access site complications, were the focus of the current analysis. Regression models (linear for continuous and logistic for binary outcomes) were used to determine whether anthropometric measures (weight, height, body mass index, and body surface area) influenced the effect of randomized access on outcomes.
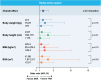
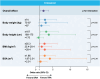
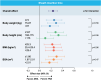
Results: Across tertiles of weight, height, body mass index, and body surface area, both before and after adjustment for sex and age, the main effect of vascular access on radial artery spasm, crossover, hemostasis time, and access site complications remained, with no significant interaction effect.
Conclusions: The results of this exploratory analysis are consistent with the main findings of the trial and support the use of DRA in all patients, regardless of anthropometric measures.
Keywords: body mass index; body surface area; distal radial access; height; transradial access; weight.
© 2025 The Authors.
Conflict of interest statement
The trial was sponsored and funded by Terumo Europe. Drs Sgueglia and Leibundgut have received consulting and lecture fees from Terumo and Cordis outside of the submitted work. Drs Aminian and Ratib have received consulting and lecture fees from Terumo. Dr Iglesias has received an unrestricted research grant to the institution from Terumo, outside of the submitted work; is a consultant for and has received personal fees from Terumo, outside of the submitted work; has received research grants to the institution from Abbott Vascular, AstraZeneca, Biosensors, Biotronik, Concept Medical, and Philips Volcano; and has received personal fees from AstraZeneca, Biotronik, Bristol Myers Squibb/Pfizer, Cardinal Health, Medtronic, Novartis, and Philips Volcano, outside the submitted work. All other authors have reported that they have no relationships relevant to the contents of this paper to disclose.
Figures



References
-
- Neumann F.J., Sousa-Uva M., Ahlsson A., et al. 2018 ESC/EACTS Guidelines on myocardial revascularization. Eur Heart J. 2019;40:87–165. - PubMed
-
- Lawton J.S., Tamis-Holland J.E., Bangalore S., et al. 2021 ACC/AHA/SCAI guideline for coronary artery revascularization: a report of the American college of cardiology/American heart association joint committee on clinical practice guidelines. J Am Coll Cardiol. 2022;79:e21–e129. - PubMed
-
- Ferrante G., Rao S.V., Juni P., et al. Radial versus femoral access for coronary interventions across the entire spectrum of patients with coronary artery disease: a meta-analysis of randomized trials. JACC Cardiovasc Interv. 2016;9:1419–1434. - PubMed
-
- Sgueglia G.A., Di Giorgio A., Gaspardone A., Babunashvili A. Anatomic basis and physiological rationale of distal radial artery access for percutaneous coronary and endovascular procedures. JACC Cardiovasc Interv. 2018;11:2113–2119. - PubMed
-
- Kiemeneij F. Left distal transradial access in the anatomical snuffbox for coronary angiography (ldTRA) and interventions (ldTRI) EuroIntervention. 2017;13:851–857. - PubMed
LinkOut - more resources
Full Text Sources

