Association between the low-density lipoprotein to high-density lipoprotein ratio and prognosis in critically ill intracerebral hemorrhage patients: a retrospective cohort study from the MIMIC-IV database
- PMID: 39905425
- PMCID: PMC11792406
- DOI: 10.1186/s12944-025-02459-z
Association between the low-density lipoprotein to high-density lipoprotein ratio and prognosis in critically ill intracerebral hemorrhage patients: a retrospective cohort study from the MIMIC-IV database
Abstract
Background: The relationship between lipid profiles and intracranial hemorrhage (ICH) has garnered increasing attention. The ratio of low-density lipoprotein to high-density lipoprotein (LHR) is one of the key lipid profile indices. However, studies investigating the association between LHR and the prognosis of critically ill ICH patients remain limited.
Methods: Data for this study were obtained from the MIMIC-IV 3.1 database. Initially, the association between LHR and short-term outcomes in ICH patients, including ICU mortality, in-hospital mortality, and 28-day mortality, was analyzed using Cox regression in both continuous and categorical models. Additionally, restricted cubic spline (RCS), subgroup, and sensitivity analyses were conducted to further validate our findings.
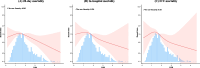
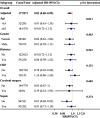
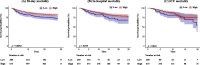
Results: The study included 873 critically ill ICH patients, among whom 20.3% (177/873) succumbed within 28 days. Higher LHR was independently associated with lower short-term mortality in ICH patients (28-day mortality: HR = 0.82, 95% CI: 0.68 ~ 0.99, P = 0.039; In-hospital mortality: HR = 0.7, 95% CI: 0.55 ~ 0.89, P = 0.004; ICU mortality: HR = 0.66, 95% CI: 0.48 ~ 0.92, P = 0.015). The RCS revealed a linear relationship between LHR and short-term all-cause mortality. Subgroup analyses demonstrated consistent results. The optimal cutoff value for LHR was determined to be 1.21. Comparing the mortality risk between the low-LHR and high-LHR groups, the high-LHR group exhibited higher survival rates (28-day mortality, P = 0.0052; In-hospital mortality, P = 0.019; ICU mortality, P = 0.044). Furthermore, higher LHR was also correlated with lower disease severity scores (SAPS-II: r = -0.158, P < 0.001, OASIS: r = -0.117, P = 0.006).
Conclusion: LHR was negatively associated with short-term mortality in critically ill ICH patients. It may aid clinicians in identifying high-risk individuals and providing timely interventions.
Keywords: Intracerebral hemorrhage; Lipid metabolism; Low-density lipoprotein to high-density lipoprotein ratio (LHR); MIMIC-IV; Prognosis.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: The study was performed according to the guidelines of the Helsinki Declaration. The use of the MIMIC-IV database was approved by the review committee of the Massachusetts Institute of Technology and Beth Israel Deaconess Medical Center. The data is publicly available (in the MIMIC-IV database), therefore, the ethical approval statement and the requirement for informed consent were waived for this study. Consent for publication: Not applicable. Competing interests: The authors declare no competing interests.
Figures
Similar articles
-
Triglyceride-glucose index as a potential predictor for in-hospital mortality in critically ill patients with intracerebral hemorrhage: a multicenter, case-control study.BMC Geriatr. 2024 May 1;24(1):385. doi: 10.1186/s12877-024-05002-4. BMC Geriatr. 2024. PMID: 38693481 Free PMC article.
-
Association between serum glucose potassium ratio and mortality in critically ill patients with intracerebral hemorrhage.Sci Rep. 2024 Nov 9;14(1):27391. doi: 10.1038/s41598-024-78230-8. Sci Rep. 2024. PMID: 39521806 Free PMC article.
-
Glycemic variability and its association with short and long term clinical outcomes in critically ill patients with cerebral hemorrhage.Sci Rep. 2025 Mar 6;15(1):7820. doi: 10.1038/s41598-025-92415-9. Sci Rep. 2025. PMID: 40050399 Free PMC article.
-
Association between Triglyceride-Glucose Index and Prognosis in Critically Ill Patients with Acute Coronary Syndrome: Evidence from the MIMIC Database.Int J Med Sci. 2025 Feb 26;22(7):1528-1541. doi: 10.7150/ijms.107976. eCollection 2025. Int J Med Sci. 2025. PMID: 40093800 Free PMC article.
-
Unveiling the role of stress hyperglycemia in predicting mortality for critically ill hemorrhagic stroke patients: insights from MIMIC-IV.Front Endocrinol (Lausanne). 2025 May 2;16:1558352. doi: 10.3389/fendo.2025.1558352. eCollection 2025. Front Endocrinol (Lausanne). 2025. PMID: 40385356 Free PMC article.
Cited by
-
Neutrophil-to-High density lipoprotein cholesterol ratio predicts early hematoma expansion in patients with spontaneous intracerebral hemorrhage.Neurosurg Rev. 2025 Jun 30;48(1):533. doi: 10.1007/s10143-025-03682-z. Neurosurg Rev. 2025. PMID: 40583091
References
-
- GBD 2017 DALYs and HALE Collaborators. Global, regional, and national disability-adjusted life-years (DALYs) for 359 diseases and injuries and healthy life expectancy (HALE) for 195 countries and territories, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet (London, England). 2018;392(10159):1859–1922. 10.1016/S0140-6736(18)32335-3. - PMC - PubMed
-
- Kojima S, Omura T, Wakamatsu W, Kishi M, Yamazaki T, Iida M, Komachi Y. Prognosis and disability of stroke patients after 5 years in Akita. Japan Stroke. 1990;21(1):72–7. - PubMed
-
- Chang CWJ, Provencio JJ, Shah S. Neurological critical care: the evolution of cerebrovascular critical care. Crit Care Med. 2021;49(6):881–900. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Miscellaneous

