The relationship between alcohol consumption and outcomes after gastrointestinal surgery: a systematic review and meta-analysis
- PMID: 39905807
- PMCID: PMC11794451
- DOI: 10.1093/alcalc/agaf002
The relationship between alcohol consumption and outcomes after gastrointestinal surgery: a systematic review and meta-analysis
Abstract
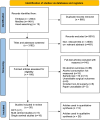
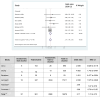
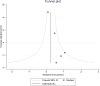
The study aimed to summarise the evidence of the association between preoperative alcohol consumption and postoperative complications in gastrointestinal surgeries. Comprehensive searches of MEDLINE, EMBASE, and Cochrane databases were undertaken to identify original studies investigating the association between preoperative alcohol consumption and postoperative complications occurring within 30 days of surgery. The primary outcome was 30-day mortality risk and secondary outcomes included postoperative complications such as surgical site infections and risk of anastomotic leak. The pooled odds ratios (ORs) and 95% confidence intervals (CIs) were estimated using a random effects model. In total, 3601 reports were identified and reviewed for eligibility, then data was extracted from 26 studies that met inclusion criteria. 13 studies were included in the meta-analysis. The total number of patients in the meta-analysis was 686 181 including 20 163 with a high alcohol intake. Clearly defined high preoperative alcohol consumption was associated with an increased risk of postoperative complications including 30-day mortality (OR = 1.56; 95% CI: 1.07-2.28). The risk of anastomotic leak was significantly increased in those undergoing colorectal surgery with a high alcohol intake, OR 2.17 (95% CI: 1.74-2.72). An increase in risk was also found for surgical site infections in those undergoing gastrointestinal surgery with high alcohol intake. (OR = 1.32; 95% CI: 1.15-1.53). Preoperative alcohol consumption was associated with an increased risk of 30-day mortality, anastomotic leak and surgical site infections. Preoperative modulation of alcohol intake may influence post-operative complications after gastrointestinal surgery.
Keywords: alcohol consumption; gastrointestinal surgery; postoperative outcomes.
© The Author(s) 2025. Medical Council on Alcohol and Oxford University Press.
Figures





References
-
- Almussallam B, Joyce M, Marcello PW. et al. What factors predict hospital readmission after colorectal surgery? - PubMed [internet]. Am Surg. 2016;82:433–8 [cited 2022 Dec 8]. Available from: https://pubmed.ncbi.nlm.nih.gov/27215725/. - PubMed
-
- Bailey SH, Bull DA, Harpole DH. et al. Outcomes after esophagectomy: a ten-year prospective cohort. Ann Thorac Surg [Internet]. 2003[cited 2022 Dec 8];75:217–22. Available from: https://pubmed.ncbi.nlm.nih.gov/12537219/. 10.1016/S0003-4975(02)04368-0. - DOI - PubMed
-
- Bertelsen CA, Andreasen AH, Jørgensen T. et al. Anastomotic leakage after anterior resection for rectal cancer: risk factors. Colorectal Dis [Internet]. 2010. [cited 2022 Dec 8];12:37–43. Available from: https://pubmed.ncbi.nlm.nih.gov/19175624/. 10.1111/j.1463-1318.2008.01711.x. - DOI - PubMed
-
- Drink less - Better Health - NHS [Internet] . 2025. [cited 2023 Jul 12]. Available from: https://www.nhs.uk/better-health/drink-less/. Published July, 2021.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

