Use of an anti-D-alloimmunization kinetics model to correct the interval censored D-alloimmunization rate following red blood cell transfusions
- PMID: 39908300
- PMCID: PMC12035998
- DOI: 10.1111/trf.18138
Use of an anti-D-alloimmunization kinetics model to correct the interval censored D-alloimmunization rate following red blood cell transfusions
Abstract
Introduction: The rate of D-alloimmunization amongst RhD-negative recipients of RhD-positive red blood cell (RBC) transfusions is not certain. Recipients with a short duration between the index RhD-positive transfusion and the last antibody detection test that did not show anti-D might become D-alloimmunized in the future. A regression model was developed to predict how often such patients might develop D-alloimmunization in the future to help account for the immunohematological uncertainty that accompanies having short serological follow up periods.
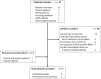
Methods: Using the published literature on recipients who were intentionally transfused with RhD-positive RBCs and serially followed with antibody screens, as well as unpublished datasets, a regression model was constructed to demonstrate the timing of D-alloimmunization for recipients who became D-alloimmunized within 6 months following the index transfusion. The model was then applied to a series of RhD-negative hospitalized recipients of at least one unit of RhD-positive RBCs who did not become D-alloimmunized but who had fewer than 6 months of serological follow up to weight their contribution to the D-alloimmunization rate.
Results: Overall, the rate of D-alloimmunization was 21/105 (20.0%). There were 39 patients whose last documented antibody screen was performed between 14 days and 6 months after the index RhD-positive transfusion, and these patients were entered into the weighted model. After applying the model, the D-alloimmunization rate rose to 26.3%.
Conclusion: Using a weighted model can help reduce the immunohematological uncertainty that accompanies the inclusion of patients with relatively short serological follow up in studies of RBC alloimmunization.
Keywords: RhD alloimmunization; RhD‐positive; anti‐D; model; patients; rate; red blood cells; transfusion.
© 2025 The Author(s). Transfusion published by Wiley Periodicals LLC on behalf of AABB.
Conflict of interest statement
MHY has given paid lectures/reimbursed travel/consulting fees for: Grifols, Hemanext, Terumo, Legacy Innovations. MHY owns equity in Velico Medical, Inc.
Figures

Similar articles
-
Rate of RhD-alloimmunization after the transfusion of multiple RhD-positive primary red blood cell-containing products.Transfusion. 2021 Jul;61 Suppl 1:S150-S158. doi: 10.1111/trf.16495. Transfusion. 2021. PMID: 34269438
-
Receipt of RhD-positive whole blood for life-threatening bleeding in female children: A survey in alloimmunized mothers regarding minimum acceptable survival benefit relative to risk of maternal alloimmunization to anti-D.Transfusion. 2024 May;64 Suppl 2:S100-S110. doi: 10.1111/trf.17807. Epub 2024 Apr 2. Transfusion. 2024. PMID: 38563495
-
Timing of RhD-positive red blood cell administration is associated with D-alloimmunization in injured patients.Transfusion. 2023 May;63 Suppl 3:S54-S59. doi: 10.1111/trf.17330. Epub 2023 Apr 17. Transfusion. 2023. PMID: 37067374
-
Impact of Red Blood Cell Antigen Matching on Alloimmunization and Transfusion Complications in Patients with Sickle Cell Disease: A Systematic Review.Transfus Med Rev. 2019 Jan;33(1):12-23. doi: 10.1016/j.tmrv.2018.07.003. Epub 2018 Jul 26. Transfus Med Rev. 2019. PMID: 30122266
-
Immunological principle of development of red blood cell alloimmunization in pregnancy, hemolytic disease of the fetus and prevention of RhD alloimmunization in RhD negative women.Ceska Gynekol. 2020 Winter;85(6):408-416. Ceska Gynekol. 2020. PMID: 33711901 Review. English.
References
-
- Ji Y, Luo G, Fu Y. Incidence of anti‐D alloimmunization in D‐negative individuals receiving D‐positive red blood cell transfusion: a systematic review and meta‐analysis. Vox Sang. 2022;117:633–640. - PubMed
-
- Hall V, Vadakekut ES, Avulakunta ID. Hemolytic Disease of the Fetus and Newborn StatPearls. 2024. - PubMed
-
- Yazer MH, Spinella PC, Anto V, Dunbar NM. Survey of group a plasma and low‐titer group O whole blood use in trauma resuscitation at adult civilian level 1 trauma centers in the US. Transfusion. 2021;61:1757–1763. - PubMed
-
- Yazer MH, Spinella PC. An international survey on the use of low titer group O whole blood for the resuscitation of civilian trauma patients in 2020. Transfusion. 2020;60(Suppl 3):S176–S179. - PubMed
-
- Clayton S, Leeper CM, Yazer MH, Spinella PC. Survey of policies at US hospitals on the selection of RhD type of low‐titer O whole blood for use in trauma resuscitation. Transfusion. 2024;64(Suppl 2):S111–S118. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources

