Uptake and 4-week outcomes of an 'opt-out' smoking cessation referral strategy in a London-based lung cancer screening setting
- PMID: 39915257
- PMCID: PMC11804203
- DOI: 10.1136/bmjresp-2024-002337
Uptake and 4-week outcomes of an 'opt-out' smoking cessation referral strategy in a London-based lung cancer screening setting
Abstract
Introduction: Lung cancer screening (LCS) enables the delivery of smoking cessation interventions to a population experiencing long-term tobacco dependence, but the optimal delivery method remains unclear. Here, we report uptake and short-term outcomes of an 'opt-out' smoking cessation referral strategy in an LCS cohort.
Methods: Individuals currently smoking tobacco who attended a face-to-face lung health check in the SUMMIT study (NCT03934866) were offered very brief advice on smoking cessation and where possible, an 'opt-out' referral to their local stop smoking service (SSS). Aggregate data on referral outcomes were obtained from each SSS individually.
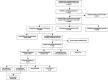
Results: 33.7% (n=2090/6203) of individuals currently smoking tobacco consented to a practitioner-made 'opt-out' smoking cessation referral. 42.7% (n=893/2090) of these individuals resided in boroughs where SSS were not present or required self-referral. Males (adjusted OR (aOR) 1.16), younger individuals (55-59: aOR 1.70, 60-64: aOR 1.71 and 65-69: aOR 1.78) and those of ethnic minority backgrounds (Asian: aOR 1.31, Black: aOR 1.71 and Mixed: aOR 1.72) were more likely to consent, while individuals from the most deprived socioeconomic quintile were less likely to do so (aOR 0.65).High level of motivation to quit within a defined time frame (aOR 1.92), previous quit attempts in the past 12 months (1-4: aOR 1.65 and ≥5: aOR 1.54) and time to first cigarette of ≤60 min (<5: aOR 2.07, 6-30: aOR 1.55 and 31-60: aOR 1.56) were measures of tobacco dependence associated with a higher likelihood of providing consent.Outcomes were available for 742 referrals. An appointment with the service was accepted by 47.3% (n=351/742) of individuals, following which 65.5% (n=230/351) set a quit date. The 4-week quit rate among those setting a quit date and all individuals referred was 57.4% (n=132/230) and 17.8% (n=132/742), respectively.
Conclusion: A proactive, 'opt-out' smoking cessation referral strategy for individuals currently smoking tobacco who interact with an LCS programme may be beneficial.
Keywords: Lung Cancer; Tobacco and the lung.
© Author(s) (or their employer(s)) 2025. Re-use permitted under CC BY. Published by BMJ Group.
Conflict of interest statement
Competing interests: AB, PV, AC, RP, CRK, JLD, CH, ST, HH and JM were or are employed by University College London (UCL) through SUMMIT Study funding provided by GRAIL, Inc. SLQ collaborates on the SUMMIT study and has received honorarium from Elsevier for writing a book chapter and payment for a presentation/website context piece from Global Lung Cancer Coalition. SMJ has received fees for advisory board membership in the last three years from Bard1 Lifescience. He has received grant income from GRAIL, Inc. He is an unpaid member of a GRAIL advisory board. He has received lecture fees for academic meetings from Cheisi and AstraZeneca. His wife works for AstraZeneca. AH has received support for travel for an advisory board meeting for Roche. He is on an academic scientific advisory board for each of Adela Bio, Roche and Luventix who are developing multicancer blood or urine tests, but receives no payments/ honoraria for this from any of these companies. NN reports honoraria for non-promotional educational talks or advisory boards from Amgen, AstraZeneca, AXANA, Boehringer Ingelheim, Bristol Myers Squibb, Daiichi Sankyo, EQRx, Fujifilm, Guardant Health, Intuitive, Janssen, Lilly, Merck Sharp & Dohme, Olympus, and Roche. He has received support for attending meetings and/or travel from Astra Zeneca, Fujifilm, Intuitive, Merck Sharp & Dohme and Olympus. He is a member of British Thoracic Oncology Group steering committee, director of UK Lung Cancer Coalition and Clinical Director of National Lung Cancer Audit. All authors perceive that these disclosures pose no academic conflict for this study and declare no other relationships or activities that could appear to have influenced the submitted work.
Figures
References
-
- Cancer Research UK Lung cancer statistics. [24-Oct-2022]. https://www.cancerresearchuk.org/health-professional/cancer-statistics/s... Available. Accessed.
-
- UK National Screening Committee Lung cancer. [27-Jan-2023]. https://view-health-screening-recommendations.service.gov.uk/lung-cancer/ Available. Accessed.
-
- Cancer Research UK Lung cancer risk. [24-Oct-2022]. https://www.cancerresearchuk.org/health-professional/cancer-statistics/s... Available. Accessed.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous