Longitudinal assessment of cerebral infarcts and small vessel disease using magnetic resonance imaging in antiphospholipid syndrome: A single-centre retrospective study
- PMID: 39917355
- PMCID: PMC11800375
- DOI: 10.1002/jha2.1065
Longitudinal assessment of cerebral infarcts and small vessel disease using magnetic resonance imaging in antiphospholipid syndrome: A single-centre retrospective study
Abstract
Introduction: Stroke is the most frequent arterial thrombosis in antiphospholipid syndrome (APS) with high rates of recurrence.
Methods and patients: A retrospective, single-centre 10-year review of patients with APS having sequential cerebral magnetic resonance imaging (MRI) was performed to describe ischaemic features in APS and associated disease risk factors and progression over time.
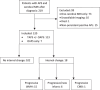
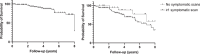
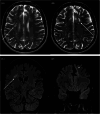
Results: A total of 120 patients and 307 scans were included with 67% of patients receiving vitamin K antagonists (VKA). Note that 65% of patients had baseline ischaemic features with white matter hyperintensities (WMH), as a feature of small vessel disease (SVD), seen in 79% of abnormal scans. Fifteen percent of patients had progressive ischaemic changes with 83% demonstrating progressive WMH and 33% new infarcts (predominantly lacunar) on sequential scans. Progression-free survival for progressive ischaemia was 88% at 5 years. Multivariate analysis showed longer follow-up was a risk for developing progressive ischaemia (odds ratio [OR] 1.43, 95% confidence interval [CI] 1.13-1.86, p = 0.005). Hypertension (56% vs. 30%, p = 0.04) and ischaemic heart disease (22% vs. 6%, p = 0.04) were more prevalent with progressive ischaemia. There was no difference in progression or bleeding events according to VKA therapeutic intensity.
Discussion: These results show SVD is a common feature of APS using MRI with progressive changes despite anticoagulation. Traditional risk factors for cerebrovascular disease were associated with progression.
Keywords: MRI; anticoagulation; antiphospholipid syndrome; imaging; stroke.
© 2025 The Author(s). eJHaem published by British Society for Haematology and John Wiley & Sons Ltd.
Conflict of interest statement
The authors declare no conflicts of interest.
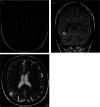
Figures


Similar articles
-
Recurrent cerebrovascular events after recent small subcortical infarction.J Neurol. 2024 Aug;271(8):5055-5063. doi: 10.1007/s00415-024-12460-8. Epub 2024 May 27. J Neurol. 2024. PMID: 38802623 Free PMC article.
-
Cerebrovascular disease in patients with antiphospholipid antibody syndrome: a transcranial Doppler and magnetic resonance imaging study.Rheumatol Adv Pract. 2024 May 7;8(2):rkae060. doi: 10.1093/rap/rkae060. eCollection 2024. Rheumatol Adv Pract. 2024. PMID: 38800574 Free PMC article.
-
Association of Cerebrovascular Reactivity With 1-Year Imaging and Clinical Outcomes in Small Vessel Disease: An Observational Cohort Study.Neurology. 2024 Dec 10;103(11):e210008. doi: 10.1212/WNL.0000000000210008. Epub 2024 Nov 5. Neurology. 2024. PMID: 39499872 Free PMC article.
-
Combined brain/heart magnetic resonance imaging in antiphospholipid syndrome-two sides of the same coin.Clin Rheumatol. 2021 Jul;40(7):2559-2568. doi: 10.1007/s10067-020-05498-2. Epub 2020 Nov 16. Clin Rheumatol. 2021. PMID: 33196982 Review.
-
Cerebral small vessel disease: Recent advances and future directions.Int J Stroke. 2023 Jan;18(1):4-14. doi: 10.1177/17474930221144911. Int J Stroke. 2023. PMID: 36575578 Free PMC article. Review.
References
-
- Miyakis S, Lockshin MD, Atsumi T, Branch DW, Brey RL, Cervera R, et al. International consensus statement on an update of the classification criteria for definite antiphospholipid syndrome (APS). J Thromb Haemost. 2006;4(2):295–306. - PubMed
-
- Barbhaiya M, Zuily S, Naden R, Hendry A, Manneville F, Amigo M‐C, et al. The 2023 ACR/EULAR antiphospholipid syndrome classification criteria. Arthritis Rheumatol. 2023;75(10):1687–1702. - PubMed
-
- Crowther MA, Ginsberg JS, Julian J, Denburg J, Hirsh J, Douketis J, et al. A comparison of two intensities of warfarin for the prevention of recurrent thrombosis in patients with the antiphospholipid antibody syndrome. N Engl J Med. 2003;349(12):1133–1138. - PubMed
-
- Tektonidou MG. Prognostic factors and clustering of serious clinical outcomes in antiphospholipid syndrome. QJM. 2000;93(8):523–530. - PubMed
-
- Sanna G. Central nervous system involvement in the antiphospholipid (Hughes) syndrome. Rheumatology (Oxford). 2003;42:200–213. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous
