Behavioural changes in frontotemporal dementia and their cognitive and neuroanatomical correlates
- PMID: 39938002
- PMCID: PMC12316017
- DOI: 10.1093/brain/awaf061
Behavioural changes in frontotemporal dementia and their cognitive and neuroanatomical correlates
Abstract
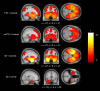
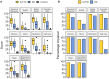
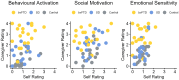
Behavioural changes are a central feature of frontotemporal dementia (FTD); they occur in both behavioural-variant (bvFTD) and semantic dementia (SD)/semantic-variant primary progressive aphasia subtypes. In this study, we addressed two current clinical knowledge gaps: (i) are there qualitative or clear distinctions between behavioural profiles in bvFTD and SD; and (ii) what are the precise roles of the prefrontal cortex and anterior temporal lobes in supporting social behaviour? Resolving these conundrums is crucial for improving diagnostic accuracy and for the development of targeted interventions to treat challenging behaviours in FTD. Informant questionnaires to assess behavioural changes included the Cambridge Behavioural Inventory-Revised and two targeted measures of apathy and impulsivity. Participants completed a detailed neuropsychological battery to permit investigation of the relationship between cognitive status (including social-semantic knowledge, general semantic knowledge and executive function) with behaviour change in FTD. To explore changes in regional grey matter volume, a subset of patients had structural MRI. Diagnosis-based group comparisons were supplemented by a transdiagnostic approach that encompassed the spectrum of bvFTD, SD and 'mixed' or intermediate cases. Such an approach is sensitive to the systematic graded variation in FTD and allows the neurobiological underpinnings of behaviour change to be explored across an FTD spectrum. We found a wide range of behavioural changes across FTD. Although quantitatively more severe on average in bvFTD, as expected, the item-level analyses found no evidence for qualitative differences in behavioural profiles or 'behavioural double dissociations' between bvFTD and SD. Comparisons of self and informant ratings revealed strong discrepancies in the perspective of the caregiver versus the patient. Logistic regression revealed that neuropsychological measures had better discriminative accuracy for bvFTD versus SD than caregiver-reported behavioural measures. A principal component analysis of all informant questionnaire domains extracted three components, interpreted as reflecting: (i) apathy; (ii) challenging behaviours; and (iii) activities of daily living. More severe apathy in both FTD subtypes was associated with: (i) increased levels of impaired executive function; and (ii) anterior cingulate cortex atrophy. Questionnaire ratings of impaired behaviour were not correlated with either anterior temporal lobe atrophy or degraded social-semantic knowledge. Together, these findings highlight the presence of a wide range of behavioural changes in both bvFTD and SD, which vary by degree rather than quality. We recommend a transdiagnostic approach for future studies of the neuropsychological and neuroanatomical underpinnings of behavioural deficits in FTD.
Keywords: behavioural-variant frontotemporal dementia; semantic dementia; social behaviour; social-semantic knowledge; transdiagnostic.
© The Author(s) 2025. Published by Oxford University Press on behalf of the Guarantors of Brain.
Conflict of interest statement
The authors report no competing interests.
Figures



References
-
- de Vugt ME, Riedijk SR, Aalten P, Tibben A, van Swieten JC, Verhey FR. Impact of behavioural problems on spousal caregivers: A comparison between Alzheimer’s disease and frontotemporal dementia. Dement Geriatr Cogn Disord. 2006;22:35–41. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources

