Transcatheter Aortic Valve Implantation (TAVI) in Bicuspid Anatomy
- PMID: 39941442
- PMCID: PMC11818256
- DOI: 10.3390/jcm14030772
Transcatheter Aortic Valve Implantation (TAVI) in Bicuspid Anatomy
Abstract
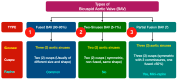
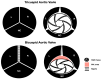
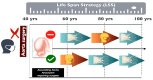
Bicuspid aortic valve (BAV) stenosis, a common congenital condition, presents unique challenges for transcatheter aortic valve replacement (TAVI) due to anatomical variations like cusp morphology, coexisting aortopathy and calcification. TAVI offers a viable option for BAV patients with refinements in technique and technology, though ongoing research is essential to optimize patient-specific approaches and long-term results. Key considerations for TAVI in BAV include precise valve sizing, positioning, and the need for rigorous pre-procedural imaging to mitigate risks such as paravalvular leak and stroke. Early results show TAVI's safety and efficacy are comparable to surgery, though BAV patients undergoing TAVI often are exposed to higher rates of post-procedural pacemaker implantation. Emerging data on next-generation self-expandable (SE) and balloon-expandable (BE) valves reveal that while both offer success in this complex anatomical aortic valve variation, gaps remain in the long-term durability and management of BAV-related aortopathy. This review examines the latest advancements in TAVI for BAV, emphasizing how specialized approaches and device selection address BAV's complexities.
Keywords: TAVI; aortic stenosis; bicuspid.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures

References
-
- Sillesen A.S., Vogg O., Pihl C., Raja A.A., Sundberg K., Vedel C., Zingenberg H., Jorgensen F.S., Vejlstrup N., Iversen K., et al. Prevalence of Bicuspid Aortic Valve and Associated Aortopathy in Newborns in Copenhagen, Denmark. JAMA. 2021;325:561–567. doi: 10.1001/jama.2020.27205. - DOI - PMC - PubMed
-
- Kalra A., Das R., Alkhalil M., Dykun I., Candreva A., Jarral O., Rehman S.M., Majmundar M., Patel K.N., Rodes-Cabau J., et al. Bicuspid Aortic Valve Disease: Classifications, Treatments, and Emerging Transcatheter Paradigms. Struct. Heart. 2024;8:100227. doi: 10.1016/j.shj.2023.100227. - DOI - PMC - PubMed
-
- Michelena H.I., Della Corte A., Evangelista A., Maleszewski J.J., Edwards W.D., Roman M.J., Devereux R.B., Fernandez B., Asch F.M., Barker A.J., et al. International consensus statement on nomenclature and classification of the congenital bicuspid aortic valve and its aortopathy, for clinical, surgical, interventional and research purposes. Eur. J. Cardiothorac. Surg. 2021;60:448–476. doi: 10.1093/ejcts/ezab038. - DOI - PubMed
Publication types
LinkOut - more resources
Full Text Sources

