Prognostic Relevance of Type 4a Myocardial Infarction and Periprocedural Myocardial Injury in Patients With Non-ST-Segment-Elevation Myocardial Infarction
- PMID: 39968630
- PMCID: PMC11913249
- DOI: 10.1161/CIRCULATIONAHA.124.070729
Prognostic Relevance of Type 4a Myocardial Infarction and Periprocedural Myocardial Injury in Patients With Non-ST-Segment-Elevation Myocardial Infarction
Abstract
Background: Periprocedural myocardial injury (PMI) with or without type 4a myocardial infarction (MI) might occur in patients with non-ST-segment-elevation MI (NSTEMI) after percutaneous coronary intervention (PCI). This study investigated the incidence and prognostic relevance of these events, according to current definitions, in patients with NSTEMI undergoing PCI. The best cardiac troponin I (cTnI) threshold of PMI for prognostic stratification is also suggested.
Methods: Consecutive patients with NSTEMI from January 2017 to April 2022 undergoing PCI with stable or falling pre-PCI cTnI levels were enrolled. According to the Fourth Universal Definition of Myocardial Infarction, the study population was stratified into those experiencing (1) PMI with type 4a MI, (2) PMI without type 4a MI, or (3) no PMI. Post-PCI cTnI increase >20% with an absolute postprocedural value of ≥5 times the 99th percentile upper reference limit within 48 hours after PCI was used to define PMI. The primary end point was 1-year all-cause mortality, and the secondary end point consisted of major adverse cardiovascular events at 1 year, including all-cause mortality, nonfatal reinfarction, urgent revascularization, nonfatal ischemic stroke, and hospitalization for heart failure. Internal validation was performed in patients enrolled between May 2022 and April 2023.
Results: Among 1412 patients with NSTEMI undergoing PCI with stable or falling cTnI levels at baseline, 240 (17%) experienced PMI with type 4a MI, 288 (20.4%) experienced PMI without type 4a MI, and 884 (62.6%) experienced no PMI. PMI was associated with an increased risk of adverse clinical outcomes, with patients with type 4a MI demonstrating the highest rates of 1-year all-cause mortality and major adverse cardiovascular events. A post-PCI ΔcTnI >20% but ≤40% showed similar outcomes to patients without PMI, whereas >40% was identified as the optimal threshold for prognostically relevant PMI, confirmed in an internal validation cohort of 305 patients.
Conclusions: Periprocedural ischemic events were frequent in patients with NSTEMI undergoing PCI with prognostic implications. A post-PCI ΔcTnI >40%, combined with an absolute postprocedural value of ≥5 times the 99th percentile upper reference limit, was identified as the optimal threshold for diagnosing prognostically relevant PMI. Recognizing these events may improve risk stratification and management of patients with NSTEMI.
Keywords: myocardial infarction; non-ST elevated myocardial infarction; percutaneous coronary intervention; treatment outcomes; troponin.
Conflict of interest statement
None.
Figures

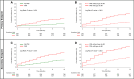

References
-
- Collet JP, Thiele H, Barbato E, Barthelemy O, Bauersachs J, Bhatt DL, Dendale P, Dorobantu M, Edvardsen T, Folliguet T, et al. ; ESC Scientific Document Group. 2020 ESC guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation. Eur Heart J. 2021;42:1289–1367. doi: 10.1093/eurheartj/ehaa575 - PubMed
-
- Fox KA, Clayton TC, Damman P, Pocock SJ, de Winter RJ, Tijssen JG, Lagerqvist B, Wallentin L; FIR Collaboration. Long-term outcome of a routine versus selective invasive strategy in patients with non-ST-segment elevation acute coronary syndrome a meta-analysis of individual patient data. J Am Coll Cardiol. 2010;55:2435–2445. doi: 10.1016/j.jacc.2010.03.007 - PubMed
-
- Elgendy IY, Mahmoud AN, Wen X, Bavry AA. Meta-analysis of randomized trials of long-term all-cause mortality in patients with non-ST-elevation acute coronary syndrome managed with routine invasive versus selective invasive strategies. Am J Cardiol. 2017;119:560–564. doi: 10.1016/j.amjcard.2016.11.005 - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

