Reduced-energy diet in women with gestational diabetes: the dietary intervention in gestational diabetes DiGest randomized clinical trial
- PMID: 39972237
- PMCID: PMC11839452
- DOI: 10.1038/s41591-024-03356-1
Reduced-energy diet in women with gestational diabetes: the dietary intervention in gestational diabetes DiGest randomized clinical trial
Abstract
Reduced-energy diets promote weight loss and improve long-term outcomes in type 2 diabetes but are untested in gestational diabetes. We aimed to identify if weight loss in pregnancy improves perinatal outcomes in gestational diabetes. We performed a multicentre parallel, randomized, controlled, double-blind trial of energy restriction in women with singleton pregnancies, gestational diabetes and body mass index ≥25 kg m-2. Participants were randomized to receive a standard-energy control diet (2,000 kcal d-1) or reduced-energy intervention diet (1,200 kcal d-1) from enrollment (29 weeks) until delivery, provided as weekly diet boxes (40% carbohydrate, 35% fat, 25% protein). The randomization was performed in a 1:1 ratio, stratified by center and blinded to the participants and study team. Primary outcomes were maternal weight change from enrollment to 36 weeks and offspring birth weight. In total, 425 participants were randomized to the control (n = 211) or intervention (n = 214). Outcome data were available for 388 of 425 (90.1%) participants at 36 weeks and 382 of 425 (89.8%) at delivery. There was no evidence of a difference in maternal weight change to 36 weeks between groups (intervention effect -0.20 (95% confidence interval -1.01, 0.61); P > 0.1) and offspring standardized birth weight (intervention effect 0.005 (-0.19, 0.20); P > 0.1). A reduced-energy diet was safe in pregnancy. ISRCTN registration no. 65152174 .
© 2025. The Author(s).
Conflict of interest statement
Competing interests: The authors declare no competing interests.
Figures

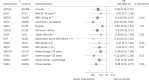

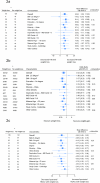
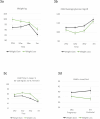
References
-
- Metzger, B. E. et al. Hyperglycemia and adverse pregnancy outcomes. N. Engl. J. Med.358, 1991–2002 (2008). - PubMed
-
- Chu, S. Y. et al. Maternal obesity and risk of gestational diabetes mellitus. Diabetes Care30, 2070–2076 (2007). - PubMed
-
- McIntyre, H. D. et al. Gestational diabetes mellitus. Nat. Rev. Dis. Prim.5, 47 (2019). - PubMed
-
- Yamamoto, J. M. et al. Gestational diabetes mellitus and diet: a systematic review and meta-analysis of randomized controlled trials examining the impact of modified dietary interventions on maternal glucose control and neonatal birth weight. Diabetes Care41, 1346–1361 (2018). - PubMed
-
- Lean, M. E. et al. Primary care-led weight management for remission of type 2 diabetes (DiRECT): an open-label, cluster-randomised trial. Lancet391, 541–551 (2018). - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

