Comparative efficacy of different antihypertensive drug classes for stroke prevention: A network meta-analysis of randomized controlled trials
- PMID: 39982885
- PMCID: PMC11845040
- DOI: 10.1371/journal.pone.0313309
Comparative efficacy of different antihypertensive drug classes for stroke prevention: A network meta-analysis of randomized controlled trials
Abstract
Objective: The study aimed to compare the effectiveness of various antihypertensive drugs in preventing strokes in hypertensive patients.
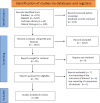
Methods: We conducted a comprehensive search of PubMed, Embase, the Cochrane Library, and ClinicalTrials.gov to identify randomized controlled trials (RCTs) investigating the efficacy of antihypertensive drugs in stroke prevention from inception until April 2023. A network meta-analysis in a Bayesian framework was performed using the random-effects model.
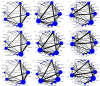
Results: This study included 88 RCTs involving 487,076 patients to investigate the effects of antihypertensive drugs in preventing stroke. Among these trials, 58 RCTs specifically focused on comparing the impact of such drugs on hypertensive subjects. In overall population, Angiotensin-converting enzyme inhibitor (ACEIs), Angiotensin receptor blockers (ARBs), Calcium channel blockers (CCBs), and Diuretics (DIs) demonstrated superiority over placebo in in reducing stroke, all-cause mortality, and cardiovascular mortality. CCBs and DIs outperformed β adrenergic receptor blockers (BBs), ACEIs, and ARBs in stroke reduction. However, when focusing on hypertensive patients, ACEIs, CCBs, and DIs proved superior to placebo in reducing stroke, all-cause mortality, and cardiovascular mortality. ARBs reduced stroke and all-cause mortality but lacked efficacy in reducing cardiovascular mortality. Of the various CCB subclasses, only the Dihydropyridines displayed efficacy in preventing stroke, all-cause mortality, and cardiovascular mortality. Among diuretic subclasses, thiazide-type DIs exhibited no efficacy in preventing all-cause mortality. ACEIs+CCBs were more effective than ACEIs or ARBs monotherapy in reducing stroke, more effective than ACEIs, ARBs, CCBs, or DIs monotherapy in reducing all-cause mortality, and more effective than ARBs in reducing cardiovascular mortality.
Conclusion: These findings suggest that ACEIs, dihydropyridine CCBs, and thiazide-like diuretics may provide superior prevention against stroke, all-cause mortality, and cardiovascular mortality in hypertensive patients. Combinations of ACEIs and CCBs may provide enhanced protection of stroke than ACEIs or ARBs monotherapy.
Copyright: © 2025 Yu et al. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Conflict of interest statement
NO authors have competing interests.
Figures
Similar articles
-
Comparative risk of new-onset diabetes mellitus for antihypertensive drugs in elderly: A Bayesian network meta-analysis.J Clin Hypertens (Greenwich). 2019 Aug;21(8):1082-1090. doi: 10.1111/jch.13598. Epub 2019 Jun 26. J Clin Hypertens (Greenwich). 2019. PMID: 31241860 Free PMC article.
-
The benefits of angiotensin-converting enzyme inhibitors/angiotensin II receptor blockers combined with calcium channel blockers on metabolic, renal, and cardiovascular outcomes in hypertensive patients: a meta-analysis.Int Urol Nephrol. 2018 Dec;50(12):2261-2278. doi: 10.1007/s11255-018-1991-x. Epub 2018 Oct 15. Int Urol Nephrol. 2018. PMID: 30324578
-
Long-Term Anti-Hypertensive Therapy and Stroke Prevention: A Meta-Analysis.Am J Cardiovasc Drugs. 2015 Aug;15(4):243-57. doi: 10.1007/s40256-015-0129-0. Am J Cardiovasc Drugs. 2015. PMID: 26055616
-
Role of antihypertensive therapy with angiotensin-converting enzyme inhibitors or angiotensin II receptor blockers in combination with calcium channel blockers for stroke prevention.J Am Pharm Assoc (2003). 2010 Sep-Oct;50(5):e116-25. doi: 10.1331/JAPhA.2010.09234. J Am Pharm Assoc (2003). 2010. PMID: 20833609 Review.
-
Diuretics versus others for long-term clinical outcomes as first-line antihypertensive medications: analysis of national real-world database.Hypertens Res. 2022 May;45(5):758-768. doi: 10.1038/s41440-022-00890-8. Epub 2022 Mar 25. Hypertens Res. 2022. PMID: 35338336
References
-
- Jussil H, Chaimani A, Carlberg B, Brunström M. Comparative efficacy and acceptability of different antihypertensive drug classes for cardiovascular disease prevention: protocol for a systematic review and network meta-analysis. BMJ Open. 2021;11(3):e044302. doi: 10.1136/bmjopen-2020-044302 - DOI - PMC - PubMed
-
- Gronewold J, Kropp R, Lehmann N, Stang A, Mahabadi AA, Weimar C, et al.. Population impact of different hypertension management guidelines based on the prospective population-based Heinz Nixdorf Recall study. BMJ Open. 2021. Feb 17;11(2):e039597. doi: 10.1136/bmjopen-2020-039597 - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

