Neonatal administration of Lactiplantibacillus plantarum ATCC 202195 with or without fructooligosaccharide in Bangladesh: a placebo-controlled randomized trial
- PMID: 39992135
- PMCID: PMC11934310
- DOI: 10.1128/msphere.01032-24
Neonatal administration of Lactiplantibacillus plantarum ATCC 202195 with or without fructooligosaccharide in Bangladesh: a placebo-controlled randomized trial
Abstract
Lactiplantibacillus plantarum ATCC 202195 (LP202195) plus fructooligosaccharide (FOS) for 7 days was previously shown to colonize the infant intestine up to 6 months of age and reduced sepsis rates among young infants in rural India. In a phase 2 randomized controlled trial in Dhaka, Bangladesh (N = 519), neonatal administration of LP202195 for 1 or 7 days, with or without FOS, increased LP202195 stool abundance from 14 to 60 days of age, versus placebo. Abundance progressively declined in the post-administration period and did not persist beyond 2 months of age. FOS did not affect LP202195 abundance or its duration of persistence. All regimens were well-tolerated and safe. The absence of LP202195 colonization was inconsistent with results from a prior trial. Additional large-scale trials of LP202195 ± FOS are needed to establish its efficacy in infants who do not become LP202195-colonized.
Importance: Among infants born in Dhaka, Bangladesh, a 7-day regimen of Lactiplantibacillus plantarum ATCC 202195 (LP202195) plus fructooligosaccharide (FOS) did not colonize the infant gastrointestinal (GI) tract. The absence of colonization is inconsistent with a prior study of the same synbiotic regimen in India, in which LP202195 was shown to persist in the infant GI tract for up to 6 months. Sustained LP202195 colonization was thought to be required for the probiotic to impart its beneficial impact on newborn sepsis. Therefore, additional trials are warranted to confirm the previously observed effects of LP202195 on infant clinical outcomes in the absence of LP202195 colonization. Moreover, since regimens of LP202195 that did not include FOS were indistinguishable from the synbiotic in terms of colonization, safety, and tolerability, future trials should assess the role of FOS for clinical efficacy; removing FOS would reduce costs, an important consideration for scale-up.
Clinical trials: This study has been registered at ClinicalTrials.gov as NCT05180201.
Keywords: colonization; developing countries; lactobacilli; neonate; probiotic; randomized controlled trial; safety; severe infection; synbiotic; tolerability.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
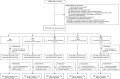

References
-
- Morgan RL, Preidis GA, Kashyap PC, Weizman AV, Sadeghirad B, Pe MP, Synbiotic Work Group . 2020. Probiotics reduce mortality and morbidity in preterm, low-birth-weight infants: a systematic review and network meta-analysis of randomized trials. Gastroenterology 159:467–480. doi:10.1053/j.gastro.2020.05.096 - DOI - PMC - PubMed
-
- Aceti A, Maggio L, Beghetti I, Gori D, Barone G, Callegari ML, Fantini MP, Indrio F, Meneghin F, Morelli L, Zuccotti G, Corvaglia L, Italian Society of Neonatology . 2017. Probiotics prevent late-onset sepsis in human milk-fed, very low birth weight preterm infants: systematic review and meta-analysis. Nutrients 9:904. doi:10.3390/nu9080904 - DOI - PMC - PubMed
-
- Panigrahi P, Parida S, Nanda NC, Satpathy R, Pradhan L, Chandel DS, Baccaglini L, Mohapatra A, Mohapatra SS, Misra PR, Chaudhry R, Chen HH, Johnson JA, Morris JG, Paneth N, Gewolb IH. 2017. A randomized synbiotic trial to prevent sepsis among infants in rural India. Nature 548:407–412. doi:10.1038/nature23480 - DOI - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

