Inherited Hypertrabeculation? Genetic and Clinical Insights in Blood Relatives of Genetically Affected Left Ventricular Excessive Trabeculation Patients
- PMID: 40003559
- PMCID: PMC11856360
- DOI: 10.3390/life15020150
Inherited Hypertrabeculation? Genetic and Clinical Insights in Blood Relatives of Genetically Affected Left Ventricular Excessive Trabeculation Patients
Abstract
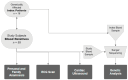
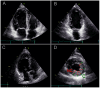
Genetically determined left ventricular excessive trabeculation (LVET) has a wide clinical spectrum ranging from asymptomatic subjects to severe heart failure with arrhythmias and thromboembolic events. Unlike other cardiomyopathies, the relatives of LVET patients never reach the spotlight of guidelines and clinical practice, although these family members can be often affected by these conditions. Thus, we aimed to investigate the relatives of LVET by multidimensional analysis, such as genetic testing, ECG and cardiac ultrasound (ECHO). We included 55 blood relatives from the family of 18 LVET patients (male = 27, age = 44 ± 20.8y), who underwent anamnesis registration. With Sanger sequencing, the relatives were classified into genetically positive (GEN-pos) and unaffected (GEN-neg) subgroups. In addition to regular ECG parameters, Sokolow-Lyon Index (SLI) values were calculated. 2D ECHO images were analysed with TomTec Arena, evaluating LV volumetric, functional (EF) and strain parameters. Individuals were categorized into JENNI-pos and JENNI-neg morphological subgroups according to the Jenni LVET ECHO criteria. Family history showed frequent involvement (arrhythmia 61%, stroke 56%, syncope 39%, sudden cardiac death 28%, implanted device 28%), as well as personal anamnesis (subjective symptoms 75%, arrhythmias 44%). ECG and ECHO parameters were within the normal range. In terms of genetics, 78% of families and 38% of relatives carried the index mutation. LV_SLI and QT duration were lower in the GEN-pos group; ECHO parameters were comparable in the subgroups. Morphologically, 33% of the relatives met Jenni-LVET criteria were genetically affected and showed lower LV_EF values. The frequently found genetic, morphological and clinical involvement may indicate the importance of screening and, if necessary, regular follow-up of relatives in the genetically affected LVET population.
Keywords: cardiology; cardiomyopathy screening; echocardiography; family health; genetics; left ventricular excessive trabeculation; noncompaction.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
Similar articles
-
Electrocardiogram Features of Left Ventricular Excessive Trabeculation with Preserved Cardiac Function in Light of Cardiac Magnetic Resonance and Genetics.J Clin Med. 2024 Oct 3;13(19):5906. doi: 10.3390/jcm13195906. J Clin Med. 2024. PMID: 39407966 Free PMC article.
-
Characteristics of the right ventricle in left ventricular noncompaction with reduced ejection fraction in the light of dilated cardiomyopathy.PLoS One. 2023 Sep 25;18(9):e0290981. doi: 10.1371/journal.pone.0290981. eCollection 2023. PLoS One. 2023. PMID: 37747903 Free PMC article.
-
The use of 2-D speckle tracking echocardiography in assessing adolescent athletes with left ventricular hypertrabeculation meeting the criteria for left ventricular non-compaction cardiomyopathy.Int J Cardiol. 2023 Jan 15;371:500-507. doi: 10.1016/j.ijcard.2022.09.076. Epub 2022 Oct 8. Int J Cardiol. 2023. PMID: 36216087
-
The Trouble with Trabeculation: How Genetics Can Help to Unravel a Complex and Controversial Phenotype.J Cardiovasc Transl Res. 2023 Dec;16(6):1310-1324. doi: 10.1007/s12265-023-10459-6. Epub 2023 Nov 29. J Cardiovasc Transl Res. 2023. PMID: 38019448 Review.
-
[Doubts of the cardiologist regarding an electrocardiogram presenting QRS V1-V2 complexes with positive terminal wave and ST segment elevation. Consensus Conference promoted by the Italian Cardiology Society].G Ital Cardiol (Rome). 2010 Nov;11(11 Suppl 2):3S-22S. G Ital Cardiol (Rome). 2010. PMID: 21361048 Italian.
References
-
- Petersen S.E., Jensen B., Aung N., Friedrich M.G., McMahon C.J., Mohiddin S.A., Pignatelli R.H., Ricci F., Anderson R.H., Bluemke D.A. Excessive Trabeculation of the Left Ventricle: JACC: Cardiovascular Imaging Expert Panel Paper. JACC Cardiovasc. Imaging. 2023;16:408–425. doi: 10.1016/j.jcmg.2022.12.026. - DOI - PMC - PubMed
-
- Jenni R., Oechslin E., Schneider J., Attenhofer Jost C., Kaufmann P.A. Echocardiographic and pathoanatomical characteristics of isolated left ventricular non-compaction: A step towards classification as a distinct cardiomyopathy. Heart. 2001;86:666–671. doi: 10.1136/heart.86.6.666. - DOI - PMC - PubMed
-
- Jacquier A., Thuny F., Jop B., Giorgi R., Cohen F., Gaubert J.Y., Vidal V., Bartoli J.M., Habib G., Moulin G. Measurement of trabeculated left ventricular mass using cardiac magnetic resonance imaging in the diagnosis of left ventricular non-compaction. Eur. Heart J. 2010;31:1098–1104. doi: 10.1093/eurheartj/ehp595. - DOI - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

