Evaluation of the Effect of Management of Drug-Related Problems on Clinical Outcomes of Pulmonary Embolism Outpatients: A Randomized Controlled Trial
- PMID: 40004736
- PMCID: PMC11856807
- DOI: 10.3390/jcm14041202
Evaluation of the Effect of Management of Drug-Related Problems on Clinical Outcomes of Pulmonary Embolism Outpatients: A Randomized Controlled Trial
Abstract
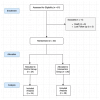
Background: Pulmonary embolism (PE) poses significant morbidity and mortality risks, necessitating tailored anticoagulant therapy. Limited studies investigate the drug-related problems (DRPs) in PE. This study aims to evaluate the impact of clinical pharmacist (CP) interventions on drug-related problems (DRPs) and clinical outcomes in outpatients with PE. By addressing DRPs in this specific population, the study seeks to assess the role of CP-led interventions in enhancing patient safety and optimizing treatment outcomes. Methods: A randomized controlled trial was conducted on PE patients at a pulmonology outpatient clinic over the period of 15 January 2022 to January 2023. In this trial, the intervention group (IG) benefited from CP recommendations targeting DRPs, while the control group (CG) was observed without any additional interventions. Follow-ups were conducted at 90 and 180 days post-discharge. The study focused on DRPs, CP interventions, and patient outcomes. Data were systematically recorded and analyzed, adhering to ethical standards and employing the PCNE v9.1 classification system. Results: The study followed 50 PE patients, with 26 in the IG and 24 in the CG. DRPs, mostly in drug and dose selection, affected 84% of participants (3.34 DRPs/patient). In the IG, the CP made 76 recommendations (91.5%) for 83 DRPs at the prescribing physician level. Majority of these recommendations (94.7%) were accepted. At the 90-day follow-up, bleeding occurred in 16.6% of the CG, with none in the IG (odds ratio [OR] = 2.3, 95% confidence interval [CI]: 1.654-3.198, p = 0.046). As indicated by Cramér's V (0.307), the effect size demonstrated a moderate association between the intervention and the absence of bleeding events in the IG. At the 180-day follow-up, bleeding was 33.3% in the CG and 16.6% in the IG (p = 0.443). Conclusions: PE patients experience common and frequent DRPs, especially in anticoagulation therapy. CP recommendations are widely accepted but need to be better implemented. No bleeding events were observed in the IG where a CP was involved at 90 days, unlike the CG. Including a CP in the PE treatment team seems to influence outcomes positively.
Keywords: anticoagulation; bleeding; clinical pharmacist; drug-related problems; pulmonary embolism.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
Similar articles
-
Investigation of drug-related problems in patients hospitalized in chest disease wards: A randomized controlled trial.Front Pharmacol. 2023 Jan 10;13:1049289. doi: 10.3389/fphar.2022.1049289. eCollection 2022. Front Pharmacol. 2023. PMID: 36703759 Free PMC article.
-
Evaluation of the clinical pharmacist's effect on achieving treatment goals in patients with hypothyroidism: a randomized controlled trial.BMC Endocr Disord. 2025 Apr 8;25(1):94. doi: 10.1186/s12902-025-01914-3. BMC Endocr Disord. 2025. PMID: 40200273 Free PMC article. Clinical Trial.
-
Handling drug-related problems in rehabilitation patients: a randomized study.Int J Clin Pharm. 2012 Apr;34(2):382-8. doi: 10.1007/s11096-012-9623-5. Epub 2012 Mar 3. Int J Clin Pharm. 2012. PMID: 22388601 Clinical Trial.
-
Evaluation of Pharmacist Medication Review Service in an Outpatient Heart Failure Clinic.J Pharm Pract. 2020 Dec;33(6):820-826. doi: 10.1177/0897190019842696. Epub 2019 May 5. J Pharm Pract. 2020. PMID: 31057060 Review.
-
Interventions for preventing venous thromboembolism in adults undergoing knee arthroscopy.Cochrane Database Syst Rev. 2020 May 6;5(5):CD005259. doi: 10.1002/14651858.CD005259.pub4. Cochrane Database Syst Rev. 2020. Update in: Cochrane Database Syst Rev. 2022 Aug 22;8:CD005259. doi: 10.1002/14651858.CD005259.pub5. PMID: 32374919 Free PMC article. Updated.
References
-
- Konstantinides S.V., Meyer G., Becattini C., Bueno H., Geersing G.J., Harjola V.-P., Huisman M.V., Humbert M., Jennings C.S., Jiménez D., et al. 2019 ESC Guidelines for the diagnosis and management of acute pulmonary embolism developed in collaboration with the European Respiratory Society (ERS) Eur. Heart J. 2020;41:543–603. doi: 10.1093/eurheartj/ehz405. - DOI - PubMed
-
- Ortel T.L., Neumann I., Ageno W., Beyth R., Clark N.P., Cuker A., Hutten B.A., Jaff M.R., Manja V., Schulman S., et al. American Society of Hematology 2020 guidelines for management of venous thromboembolism: Treatment of deep vein thrombosis and pulmonary embolism. Blood Adv. 2020;4:4693–4738. doi: 10.1182/bloodadvances.2020001830. - DOI - PMC - PubMed
-
- Arseven O., Ekim N., Müzellim B., Oğuzülgen İ.K., Okumuş N.G., Öngen G., Aksoy E., Altın S., Atış S., Aydıner Ö., et al. Turkish Thoracic Society Pulmonary Thromboembolism Diagnosis and Treatment Consensus Report. 2015. [(accessed on 3 December 2023)]. Available online: https://toraks.org.tr/site/community/library/dwkHt8qc8GMSPZfT.
-
- Stevens S.M., Woller S.C., Kreuziger L.B., Bounameaux H., Doerschug K., Geersing G.-J., Huisman M.V., Kearon C., King C.S., Knighton A.J., et al. Antithrombotic therapy for VTE disease: Second update of the CHEST guideline and expert panel report. Chest. 2021;160:e545–e608. doi: 10.1016/j.chest.2021.07.055. - DOI - PubMed
-
- Alrowily A., Jalal Z., Abutaleb M.H., Osman N.A., Alammari M., Paudyal V. Medication errors associated with direct-acting oral anticoagulants: Analysis of data from national pharmacovigilance and local incidents reporting databases. J. Pharm. Policy Pract. 2021;14:1–8. doi: 10.1186/s40545-021-00369-w. - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous