Impact of Smoking on Cervical Histopathological Changes in High-Risk HPV-Positive Women: A Matched Case-Control Study
- PMID: 40005352
- PMCID: PMC11857344
- DOI: 10.3390/medicina61020235
Impact of Smoking on Cervical Histopathological Changes in High-Risk HPV-Positive Women: A Matched Case-Control Study
Abstract
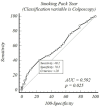
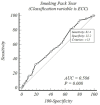
Background and Objectives: The aims of this study were to assess the impact of smoking on cervical histopathology in women with high-risk HPV types 16 and 18 (the most common types) utilizing comprehensive clinical data and to conduct a risk analysis based on smoking pack-years. Materials and Methods: Between 2022 and 2024, 1048 high-risk HPV-positive women aged 25 to 65 years were categorized into two groups: smokers and non-smokers. Data acquired from a histopathological examination of samples collected during a colposcopic evaluation of these women were compared individually regarding clinical and demographic factors, specifically age, gravida, parity, and alcohol consumption. Subsequently, the impact of prolonged and excessive smoking on histopathological cellular changes was assessed in women with the same characteristics. A case-control study was performed on 312 smokers and 312 non-smokers following mutual matching. Results: The women were matched one-to-one regarding gravida, parity, and alcohol consumption. Subsequently, they were paired within a ±2-year age range. The mean age of the smoker group was 47.1 ± 8.8, while that of the non-smoker group was 47.2 ± 8.5 (p: 0.904). In all cases of high-risk HPV positivity, the rate of normal cervical cytological results was 14% in women who smoked and 29% in women who did not smoke. The LGSIL, HGSIL, ASC-H, and AGC-NOS rates were elevated in the smoker group, and a statistically significant difference was observed between the two groups in terms of abnormal cervical cytological results (p < 0.001). After a colposcopic biopsy, the smoker group exhibited higher rates of HGSILs, LGSILs, AGC-NOS, and CIS pathological lesions (28% vs. 23%), whereas the non-smoker group exhibited higher rates of chronic cervicitis (23% vs. 16%). However, no statistically significant difference was found between the two groups (p: 0.092). In a comparison of endocervical curettage (ECC) samples, it was observed that the HGSIL, CIS, and AGC-FN rates in the smoker group were almost the same as those in the non-smoker group. However, the LGSIL histopathology results (32% vs. 18%) were higher, and the rate of negativity with no pathology was higher in the non-smoker group (72% vs. 59%). A statistically significant difference in ECC histopathology was noted between the two groups (p < 0.001). An ROC analysis conducted between smoking pack-years and the colposcopic and endocervical curettage biopsy results revealed that the cutoff value for the colposcopic abnormal histopathological results increased, with 40% sensitivity and 76% specificity above 20 pack-years (AUC: 0.592 and p: 0.025). Additionally, the abnormal histopathology rates for endocervical curettage exhibited 81% sensitivity and 32% specificity above 13 pack-years (AUC: 0.586 and p: 0.008). The rate of abnormalities in the colposcopic biopsy results was 2.19 times higher for individuals with over 20 pack-years, and the rate of abnormalities in the ECC results was 2.08 times higher for those with over 13 pack-years; additionally, statistically significant results were obtained (p-values of 0.027 and 0.008, respectively). Conclusions: The most important cause of neoplastic changes in the cervix uteri is high-risk HPV infection, with evidence indicating that prolonged excessive smoking significantly exacerbates the persistence and progression of HPV infection, thereby influencing neoplastic changes in the cervix uteri. It is crucial for women to cease smoking in order to eradicate HPV infection from the body.
Keywords: cigarettes; colposcopy; endocervical curettage; high-risk HPV; histopathology; quantity of cigarette packs.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
Similar articles
-
The Impact of Tamoxifen Usage in Breast Cancer Patients on the Development of Histopathological Lesions in the Cervix Uteri.Medicina (Kaunas). 2024 Aug 6;60(8):1268. doi: 10.3390/medicina60081268. Medicina (Kaunas). 2024. PMID: 39202549 Free PMC article.
-
The role of endocervical curettage in the diagnosis of cervical intraepithelial neoplasia in human papillomavirus positive patients.Ann Saudi Med. 2024 Jul-Aug;44(4):220-227. doi: 10.5144/0256-4947.2024.220. Epub 2024 Aug 1. Ann Saudi Med. 2024. PMID: 39127897 Free PMC article.
-
Comparison of human papillomavirus testing and cervical cytology with colposcopic examination and biopsy in cervical cancer screening in a cohort of patients with Sjogren's syndrome.Eur J Gynaecol Oncol. 2007;28(4):302-6. Eur J Gynaecol Oncol. 2007. PMID: 17713098
-
Is routine ECC necessary in patients with HPV16 and normal cytology?Diagn Cytopathol. 2018 Dec;46(12):1031-1035. doi: 10.1002/dc.24096. Epub 2018 Oct 24. Diagn Cytopathol. 2018. PMID: 30353715
-
Pooled analysis on the necessity of random 4-quadrant cervical biopsies and endocervical curettage in women with positive screening but negative colposcopy.Medicine (Baltimore). 2017 Apr;96(17):e6689. doi: 10.1097/MD.0000000000006689. Medicine (Baltimore). 2017. PMID: 28445270 Free PMC article.
Cited by
-
Investigating the link between HPV genotypes and cervical abnormality incidence in women with HPV infections: insights from a leading referral centre.Virol J. 2025 Jul 31;22(1):264. doi: 10.1186/s12985-025-02858-9. Virol J. 2025. PMID: 40745336 Free PMC article.
-
High frequency of sexually transmitted infections in patients with precancerous cervical lesions in Brazil.Front Public Health. 2025 Jun 24;13:1480959. doi: 10.3389/fpubh.2025.1480959. eCollection 2025. Front Public Health. 2025. PMID: 40630404 Free PMC article.
-
Oxidative Stress, Inflammation, and Antioxidant Strategies in Cervical Cancer-A Narrative Review.Int J Mol Sci. 2025 May 21;26(10):4961. doi: 10.3390/ijms26104961. Int J Mol Sci. 2025. PMID: 40430101 Free PMC article. Review.
References
-
- Ferlay J., Colombet M., Soerjomataram I., Parkin D.M., Piñeros M., Znaor A., Bray F. Cancer statistics for the year 2020: An overview. Int. J. Cancer. 2021. ahead of print . - PubMed
-
- Restaino S., Pellecchia G., Arcieri M., Bogani G., Taliento C., Greco P., Driul L., Chiantera V., Ercoli A., Fanfani F., et al. Management for Cervical Cancer Patients: A Comparison of the Guidelines from the International Scientific Societies (ESGO-NCCN-ASCO-AIOM-FIGO-BGCS-SEOM-ESMO-JSGO) Cancers. 2024;16:2541. doi: 10.3390/cancers16142541. - DOI - PMC - PubMed
-
- Pruski D., Fraszczak J., Iwaniec K., Przybylski M., Kedzia W., Gretkiewicz-Tomczyk A., Karowicz-Bilińska A., Spaczyński M. Assessment of frequency of regression and progression of mild cervical neoplasia--LGSIL in women with positive high-risk HPV DNA test result. Ginekol. Pol. 2012;83:572–575. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous