Association of Rapidly Elevated Plasma Tau Protein With Cognitive Decline in Patients With Amnestic Mild Cognitive Impairment and Alzheimer's Disease
- PMID: 40017276
- PMCID: PMC11878146
- DOI: 10.30773/pi.2024.0094
Association of Rapidly Elevated Plasma Tau Protein With Cognitive Decline in Patients With Amnestic Mild Cognitive Impairment and Alzheimer's Disease
Abstract
Objective: Whether elevation in plasma levels of amyloid and tau protein biomarkers are better indicators of cognitive decline than higher baseline levels in patients with amnestic mild cognitive impairment (aMCI) and Alzheimer's disease (AD) remains understudied.
Methods: We included 67 participants with twice testing for AD-related plasma biomarkers via immunomagnetic reduction (IMR) assays (amyloid beta [Aβ]1-40, Aβ1-42, total tau [t-Tau], phosphorylated tau [p-Tau] 181, and alpha-synuclein [α-Syn]) and the Mini-Mental State Examination (MMSE) over a 1-year interval. We examined the correlation between biomarker levels (baseline vs. longitudinal change) and annual changes in the MMSE scores. Receiver operating characteristic curve analysis was conducted to compare the biomarkers.
Results: After adjustment, faster cognitive decline was correlated with lower baseline levels of t-Tau (β=0.332, p=0.030) and p-Tau 181 (β=0.369, p=0.015) and rapid elevation of t-Tau (β=-0.330, p=0.030) and p-Tau 181 levels (β=-0.431, p=0.004). However, the levels (baseline and longitudinal changes) of Aβ1-40, Aβ1-42, and α-Syn were not correlated with cognitive decline. aMCI converters had lower baseline levels of p-Tau 181 (p=0.002) but larger annual changes (p=0.001) than aMCI non-converters. The change in p-Tau 181 levels showed better discriminatory capacity than the change in t-Tau levels in terms of identifying AD conversion in patients with aMCI, with an area under curve of 86.7% versus 72.2%.
Conclusion: We found changes in p-Tau 181 levels may be a suitable biomarker for identifying AD conversion.
Keywords: Alzheimer’s disease; Amyloid; Biomarker; Mild cognitive impairment; Tau protein.
Conflict of interest statement
The authors have no potential conflicts of interest to disclose.
Figures

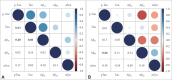

References
-
- Doody R, Kurz A, Mohs RC, Morris JC, Rabins PV, et al. Current concepts in mild cognitive impairment. Arch Neurol. 2001;58:1985–1992. - PubMed
-
- Hanon O, Vidal JS, Lehmann S, Bombois S, Allinquant B, Baret-Rose C, et al. Plasma amyloid beta predicts conversion to dementia in subjects with mild cognitive impairment: the BALTAZAR study. Alzheimers Dement. 2022;18:2537–2550. - PubMed
Grants and funding
- MOST 108-2314-B-016-023/National science and technology council
- MOST 108-2314-B-016-020/National science and technology council
- 110-2314-B-016-036-MY2/National science and technology council
- TSGH-C108-100/Tri-Service General Hospital
- TSGH-C108-216/Tri-Service General Hospital
- TSGH-D-109-101/Tri-Service General Hospital
- TSGH-D-109-185/Tri-Service General Hospital
- TSGH-D-110048/Tri-Service General Hospital
- TSGH-D113108/Tri-Service General Hospital
- TSGH-D114105/Tri-Service General Hospital
- KSVGH-112-123/Kaohsiung Veterans General Hospital
- KSVGH-112-124/Kaohsiung Veterans General Hospital
- KSVGH-113-069/Kaohsiung Veterans General Hospital
- KSVGH-113-060/Kaohsiung Veterans General Hospital
LinkOut - more resources
Full Text Sources
Miscellaneous

