Electrical Impedance Tomography during the Extubation Phase in Very Preterm Born Infants
- PMID: 40031894
- PMCID: PMC12129417
- DOI: 10.1159/000544811
Electrical Impedance Tomography during the Extubation Phase in Very Preterm Born Infants
Abstract
Introduction: Although many preterm born infants require invasive mechanical ventilation, it is also associated with detrimental effects. Early extubation should be pursued, but extubation failure is yet common. The critical transition to noninvasive ventilation is characterized by respiratory physiological changes, warranting noninvasive monitoring. We aimed to determine whether electrical impedance tomography (EIT) could provide insights into the respiratory mechanics of neonates around extubation, and if findings were different between successful and failed extubation.
Methods: Single-center observational study where EIT and transcutaneous CO2 measurements were performed in preterm born infants <32 weeks gestational age. Measurements were performed from 24 h before up to 48 h after extubation. EIT parameters extracted from the hour before and after extubation were analyzed to evaluate the short-term physiological changes.
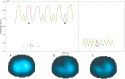
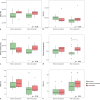
Results: Twenty-one patients were included and 6 (29%) were reintubated. End-expiratory lung impedance and tidal impedance variation were stable around extubation (p = 0.86 and p = 0.47, respectively). Compared to successfully extubated patients, reintubated patients showed more lung inhomogeneity (GI index) after extubation (0.75 vs. 0.84, p = 0.03). The percentage of nondependent silent spaces decreased after extubation in successfully extubated patients (p < 0.001). Body position and ventilator mode influenced these findings.
Conclusion: EIT measurements in preterm neonates provide valuable insight into the respiratory physiology during the transition from invasive to noninvasive ventilation, with significant differences in ventilation distribution and lung homogeneity between successfully extubated and reintubated patients. EIT has the potential to guide personalized respiratory support by assessing ventilation distribution and quantifying inhomogeneity, aiding in the optimization of ventilation settings.
Keywords: Electrical impedance tomography; Extubation; Preterm neonate; Ventilation.
© 2025 The Author(s). Published by S. Karger AG, Basel.
Conflict of interest statement
All declared interests are not related to the submitted work. A.H.J. has received research funding (paid to the institution) from ZonMw, Pulmotech B.V., Liberate Medical, the Netherlands eScience center and Health∼Holland. H.E. has received unrestricted research grants from ZonMW (The Netherlands), Fisher and Paykel Healthcare (Auckland, New Zealand), Roche Diagnostics International Ltd. (Basel, Switzerland), and Ventinova Medical B.V. (Eindhoven, The Netherlands) and speakers’ fee from Getinge (Sweden). The remaining authors declare that they have no relevant competing interests.
Figures
References
-
- Venkatesh V, Ponnusamy V, Anandaraj J, Chaudhary R, Malviya M, Clarke P, et al. . Endotracheal intubation in a neonatal population remains associated with a high risk of adverse events. Eur J Pediatr. 2011;170(2):223–7. - PubMed
-
- Sant’Anna GM, Keszler M. Weaning infants from mechanical ventilation. Clin Perinatol. 2012;39(3):543–62. - PubMed
-
- Manley BJ, Doyle LW, Owen LS, Davis PG. Extubating extremely preterm infants: predictors of success and outcomes following failure. J Pediatr. 2016;173:45–9. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

