Reduction of cardiovascular risk factors by the diet - Evaluation of the MoKaRi concept by a parallel-designed randomized study
- PMID: 40057729
- PMCID: PMC11889781
- DOI: 10.1186/s12944-025-02500-1
Reduction of cardiovascular risk factors by the diet - Evaluation of the MoKaRi concept by a parallel-designed randomized study
Abstract
Background and aim: The MoKaRi study aims to evaluate the impact of two nutritional concepts on cardiometabolic risk factors.
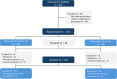
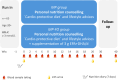
Methods: For our 20-week intervention study, 65 participants with moderate elevated low-density lipoprotein cholesterol (LDL-C; ≥ 3 mmol/l) and without lipid-lowering therapy were recruited. The intervention to improve nutritional behavior was based on individualized menu plans which were characterized by defined energy and nutrient intake. To improve compliance, individual nutritional counselling sessions were held every two weeks. In addition to motivation, cooking skills were strengthened and nutritional knowledge was imparted. Follow-up visits were carried out after 10 and 20 weeks.
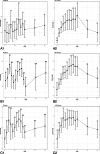
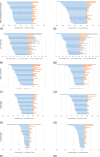
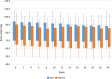
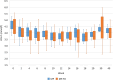
Results: The MoKaRi diet lowered the concentrations of total cholesterol (menu plan group (MP): -15%; menu plan plus fish oil group (MP-FO): -11%), LDL-C (MP: -14%; MP-FO: -16%) and non-high-density lipoprotein cholesterol (MP: -16%; MP-FO: -13%) (p < 0.001). Body weight (MP: -5%; MP-FO: -8%; p < 0.05), waist circumference (MP: -6%; MP-FO: -9%) as well as diastolic blood pressure (MP: -8%; MP-FO: -8%), apolipoprotein A1 (MP: -15%; MP-FO: -20%), apolipoprotein B (MP: -15%; MP-FO: -6%) and glycated hemoglobin A1c (HbA1c) (MP: -1.8%; MP-FO: -3.6%) were also reduced in both groups after 20 weeks (p < 0.05). In both intervention groups, a maximum reduction in LDL-c of approx. 26% was achieved within the 20 weeks of intervention. Individual participants achieved a reduction of 45-49%. The supplementation of fish oil on top of the menu plans resulted in more substantial effects on body weight (MP: -5% vs. MP-FO: -8%), body fat (MP: -11% vs. MP-FO: -20%), triglycerides (MP: -14% vs. MP-FO: -28%), high-sensitivity C-reactive protein (MP: -19% vs. MP-FO: -43%) and HbA1c (MP: -1.8% vs. MP-FO:-3.6%; p < 0.05).
Conclusions: The MoKaRi diet resulted in a significant reduction of cardiometabolic risk factors. Our data highlights the additional benefit of the combination between menu plans and fish oil supplementation, which resulted in more substantial effects on body weight, BMI, TG, HbA1c and hs-CRP.
Gov identifier: NCT02637778.
Keywords: Cardiovascular risk; Dietary fibers; Fatty acids; Nutritional concepts.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: All participants were informed about the aims and scope of the study by the study leader, and if they agreed, they provided written informed consent. All study procedures were carried out in accordance with the Declaration of Helsinki (1989) of the World Medical Association. The study protocol has been approved by the responsible ethical committee (Ethical Committee of the Friedrich-Schiller-University, file number 4656-01/16). The MoKaRi study was registered before launching (ClinicalTrials.gov Identifier: NCT02637778; https://clinicaltrials.gov/ct2/show/NCT02637778 ). Competing interests: The authors declare no competing interests.
Figures
References
-
- World Health Organization. Cardiovascular diseases (CVDs). 2021, accessed 04/11/24 at: https://www.who.int/news-room/fact-sheets/detail/cardiovascular-diseases...).
-
- Voigtländer T, Schunkert H, Vestweber M. Deutsche Herzstiftung e. V. Deutscher Herzbericht 2024. Frankfurt am Main: Deutsche Herzstiftung e.V.; 2024. https://epaper.herzstiftung.de/#0. Accessed 11 Apr 2024.
-
- WifOR Institute. The burden of cardiovascular diseases in Germany 2022, accessed 04/11/24 at https://www.wifor.com/uploads/2022/04/WifOR_Report_Burden-of-CVDs-in-Ger....
-
- Zhang H, Zhou XD, Shapiro MD, Lip GYH, Tilg H, Valenti L, Somers VK, Byrne CD, Targher G, Yang W, Viveiros O, Opio CK, Mantzoros CS, Ryan JD, Kok KYY, Jumaev NA, Perera N, Robertson AG, Abu-Abeid A, Misra A, Wong YJ, Ruiz-Úcar E, Ospanov O, Kızılkaya MC, Luo F, M´endez-S´anchez N, Zuluaga M, Lonardo A, Al, Momani H, Toro-Huamanchumo CJ, Adams L, Al-Busafi SA, Sharara AI, Chan WK, Abbas SI, Sookoian S, Treeprasertsuk S, Ocama P, Alswat K, Kong AP, Ataya K, Lim-Loo MC, Oviedo RJ, Szepietowski O, Fouad Y, Zhang H, Abdelbaki TN, Katsouras CS, Prasad A, Thaher O, Ali A, Molina GA, Sung KC, Chen QF, Lesmana CRA, Zheng MH. Global burden of metabolic diseases, 1990–2021. Metabolism 2024;14155999. 10.1016/j.metabol.2024.155999. - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

