The utility of brain biomarkers in predicting survival and neurological outcomes in pediatric patients after cardiac arrest: A systematic review and meta-analysis
- PMID: 40062924
- PMCID: PMC12068238
- DOI: 10.5603/cj.103883
The utility of brain biomarkers in predicting survival and neurological outcomes in pediatric patients after cardiac arrest: A systematic review and meta-analysis
Abstract
Background: Cardiac arrest in children is associated with high morbidity and mortality, primarily due to neurological injury. Biomarkers linked to brain injury, released into circulation from compromised elements of the neurovascular unit, act as significant prognostic indicators in patients suffering from hypoxic-ischemic brain injury (HIBI) subsequent to the restoration of spontaneous circulation (ROSC) after pediatric cardiac arrest. The aim of this systematic review and meta-analysis is to evaluate the prognostic utility of brain injury biomarkers in predicting neurological outcomes and survival in patients following cardiac arrest in the pediatric population.
Methods: Bibliographic databases (PubMed, the Cochrane Library, and Embase) were searched from their inception to November 2024. A random-effect model was used for all analyses.
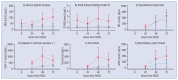
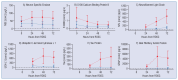
Results: Our meta-analysis demonstrates significant associations between various biomarkers and survival or neurological outcomes after cardiac arrest. Neuron-specific enolase (NSE) levels were consistently elevated in non-survivors and patients with unfavorable neurological outcomes, with pronounced differences observed on Days 2 and 3 (e.g., Day 3 mean difference: -88.48, 95%CI: -146.77 to -30.19, P = 0.003). Emerging biomarkers, including UCH-L1 and GFAP, showed striking differences, such as elevated UCH-L1 levels on Day 1 (mean difference: -415.41, 95%CI: -474.41 to -356.61, P < 0.001) and GFAP levels exceeding 4000 ng/mL in non-survivors on Day 2 (P < 0.001).
Conclusions: Our findings underscore the significant prognostic value of biomarkers in predicting survival and neurological outcomes following cardiac arrest. Neuron-specific enolase (NSE) consistently demonstrated its reliability across multiple time points, while emerging biomarkers like UCH-L1 and GFAP showed promising potential for early outcome stratification.
Keywords: S100β protein; brain markers; cardiac arrest; meta-analysis; neuron-specific enolase; survival.
Conflict of interest statement
Figures

References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous
