Hypertensive Disorders of Pregnancy and Peripartum Cardiomyopathy: A Meta-Analysis of Prevalence and Impact on Left Ventricular Function and Mortality
- PMID: 40095796
- PMCID: PMC11900926
- DOI: 10.3390/jcm14051721
Hypertensive Disorders of Pregnancy and Peripartum Cardiomyopathy: A Meta-Analysis of Prevalence and Impact on Left Ventricular Function and Mortality
Abstract
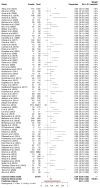
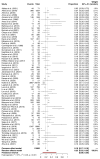
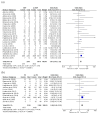
Background: The purpose of this meta-analysis was to examine the prevalence of hypertensive disorders of pregnancy (HDPs), particularly preeclampsia (PE), in peripartum cardiomyopathy (PPCM)-affected pregnancies, and to evaluate whether a HDP significantly alters the prognosis of PPCM, with specific reference to the recovery of left ventricular function (LVEF) and mortality. Methods: A total of 5468 potentially eligible studies were identified, and 104 were included in the meta-analysis. For pooling proportions, the inverse variance methods with logit transformation were used. Complete recovery of LVEF (>50%) and mortality were expressed by odds ratios (ORs), with 95% confidence intervals (CIs). The Peto OR (POR) was used in cases of rare events. Baseline LV function and baseline LV end-diastolic diameter (LVEDD) were summarized by the mean difference (MD) and 95% confidence interval (CI). Results: The summary estimate of the prevalence of HDPs and PE in women with PPCM was 36% and 25%, respectively. Patients with HDPs and, more specifically, PE with PPCM had a higher chance of complete recovery (OR = 1.87; 95%CI = 1.64 to 2.13; p < 0.001 and OR = 1.98; 95%CI 1.69 to 2.32; p < 0.001, respectively), a higher baseline LVEF (MD, 1.42; 95% CI 0.16 to 2.67; p = 0.03 and MD, 1.69; 95% CI 0.21 to 3.18; p = 0.03, respectively), and a smaller baseline LVEDD (MD, -1.31; 95% CI -2.50 to -0.13; p = 0.03 and MD, -2.63; 95% CI -3.75 to -1.51; p < 0.001, respectively). These results, however, did not translate into a significant difference in 12-month mortality (POR = 0.80; 95% CI = 0.57 to 1.13; p = 0.21 and POR = 1.56; 95% CI 0.90 to 2.73; p = 0.12, respectively). Conclusions: The findings of this study may contribute to evidence that can be utilized to aid in the risk stratification of patients with PPCM regarding their long-term prognoses.
Keywords: hypertensive disorder; meta-analysis; peripartum cardiomyopathy; preeclampsia; pregnancy.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures






References
-
- Pearson G.D., Veille J.-C., Rahimtoola S., Hsia J., Oakley C.M., Hosenpud J.D., Ansari A., Baughman K.L. Peripartum cardiomyopathy: National Heart, Lung, and Blood Institute and Office of Rare Diseases (National Institutes of Health) workshop recommendations and review. JAMA. 2000;283:1183–1188. doi: 10.1001/jama.283.9.1183. - DOI - PubMed
-
- Bauersachs J., Konig T., Meer P., Petrie M.C., Hilfiker-Kleiner D., Mbakwem A., Hamdan R., Jackson A.M., Forsyth P., Boer R.A., et al. Pathophysiology, diagnosis and management of peripartum cardiomyopathy: A position statement from the Heart Failure Association of the European Society of Cardiology Study Group on peripartum cardiomyopathy. Eur. J. Heart Fail. 2019;21:827. doi: 10.1002/ejhf.1493. - DOI - PubMed
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources

