Exploring the impact of metabolic comorbidities on epicardial adipose tissue in heart failure with preserved ejection fraction
- PMID: 40121452
- PMCID: PMC11929347
- DOI: 10.1186/s12933-025-02688-7
Exploring the impact of metabolic comorbidities on epicardial adipose tissue in heart failure with preserved ejection fraction
Abstract
Background: Heart failure (HF) with preserved ejection fraction (HFpEF) is increasingly prevalent worldwide due to aging and comorbidities. Epicardial adipose tissue (EAT), favored by diabetes and obesity, was shown to contribute to HFpEF pathophysiology and is an emerging therapeutic target. This study explored the relationship between ventricular EAT measured by cardiovascular magnetic resonance (CMR), metabolic factors, and imaging characteristics in controls, pre-HF patients, and HFpEF patients.
Methods: Patients from a Belgian cohort enrolled from December 2015 to June 2017 were categorized by HF stage: pre-HF (n = 16), HFpEF (n = 104) and compared to matched controls (n = 26) and to pre-HF (n = 191) from the Beta3-LVH cohort. Biventricular EAT volume was measured in end-diastolic short-axis cine stacks. In the Belgian cohort, associations between EAT, HF stage, and various biological and imaging markers were explored. The clinical endpoint was a composite of mortality or first HF hospitalization in the HFpEF group.
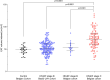
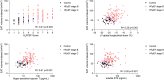
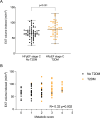
Results: EAT significantly differed between groups, with higher values in HFpEF patients compared to pre-HF and controls (72.4 ± 20.8ml/m2vs. 55.0 ± 11.8ml/m2 and 48 ± 8.9ml/m2, p < 0.001) from the Belgian cohort and to pre-HF (52.0 ± 15.0 ml/m2, p < 0.001) from the Beta3-LVH cohort. Subsequent analyses focused on the Belgian cohort. In contrast to atrial fibrillation, diabetes prevalence and body mass index (BMI) did not differ between pre-HF and HFpEF patients. Multivariable logistic regression and random forest classification identified EAT, N-terminal pro-B-type natriuretic peptide (NT-proBNP), and H2FPEF score as strong markers of HFpEF status. EAT was significantly correlated with H2FPEF score (r = 0.41, p = 0.003), BMI (r = 0.30, p < 0.001), high-sensitive troponin T (r = 0.41, p < 0.001), NT-proBNP (r = 0.37, p < 0.001), soluble suppression of tumorigenicity-2 (sST2) (r = 0.30, p < 0.001), E/e' ratio (r = 0.33, p < 0.001), and left ventricular global longitudinal strain (r = 0.35, p < 0.001). In HFpEF patients, diabetes, ischemic cardiomyopathy, and elevated sST2 were independently associated with elevated EAT. In contrast with diabetes and BMI, increased EAT was not associated with prognosis.
Conclusions: EAT assessed by CMR was significantly higher in HFpEF patients compared to controls and pre-HF patients, irrespective of diabetes and BMI. EAT was moderately associated with HFpEF status. HFpEF patients with elevated EAT exhibited a marked diabetic, ischemic, and inflammatory profile, highlighting the potential role of drugs targeting EAT.
Trial registration: Characterization of Heart Failure With Preserved Ejection Fraction; Assessment of Efficacy of Mirabegron, a New beta3-adrenergic Receptor in the Prevention of Heart Failure (Beta3_LVH).
Trial registration number: ClinicalTrials.gov. Identifier: NCT03197350; NCT02599480.
Keywords: Cardiovascular magnetic resonance (CMR); Diabetes; Epicardial adipose tissue; Heart failure with preserved ejection fraction; Inflammation; Metabolic syndrome; Obesity; Soluble ST2.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: The study was approved by the Institutional Review Board of the Cliniques universitaires Saint-Luc, Université Catholique de Louvain, and all participants gave written consent to participate in the study. Consent for publication: Not applicable. Competing interests: The authors declare no competing interests.
Figures


References
-
- Packer M, Lam CSP, Lund LH, Maurer MS, Borlaug BA. Characterization of the inflammatory-metabolic phenotype of heart failure with a preserved ejection fraction: a hypothesis to explain influence of sex on the evolution and potential treatment of the disease. Eur J Heart Fail. 2020;22(9):1551–67. - PMC - PubMed
Publication types
MeSH terms
Substances
Associated data
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

