Ground-Glass Opacities in the Access Route and Biopsy in Highly Perfused Dependent Areas of the Lungs as Risk Factors for Pulmonary Hemorrhage During CT-Guided Lung Biopsy: A Retrospective Study
- PMID: 40137575
- PMCID: PMC11945665
- DOI: 10.3390/tomography11030035
Ground-Glass Opacities in the Access Route and Biopsy in Highly Perfused Dependent Areas of the Lungs as Risk Factors for Pulmonary Hemorrhage During CT-Guided Lung Biopsy: A Retrospective Study
Abstract
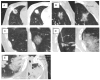
Background/objectives: The risk of hemorrhage during CT-guided lung biopsy has not been systematically studied in cases where ground-glass opacities (GGO) are present in the access route or when biopsies are performed in highly perfused, dependent lung areas. While patient positioning has been studied for pneumothorax prevention, its role in minimizing hemorrhage risk remains unexplored. This study aimed to determine whether GGOs in the access route and biopsies in dependent lung areas are risk factors for pulmonary hemorrhage during CT-guided lung biopsy.
Methods: A retrospective analysis was conducted on 115 CT-guided lung biopsies performed at a single center (2020-2023). Patients were categorized based on post-interventional hemorrhage exceeding 2 cm (Grade 2 or higher). We evaluated the presence of GGOs in the access route and biopsy location (dependent vs. non-dependent areas) using chi square, Fisher's exact, and Mann-Whitney U tests. Univariate and multivariate logistic regression analyses were conducted to evaluate risk factors for pulmonary hemorrhage.
Results: Pulmonary hemorrhage beyond 2 cm occurred in 30 of 115 patients (26%). GGOs in the access route were identified in 67% of these cases (p < 0.01), and hemorrhage occurred more frequently when biopsies were performed in dependent lung areas (63% vs. 40%, p = 0.03). Multivariable analysis showed that GGOs in the access route (OR 5.169, 95% CI 1.889-14.144, p = 0.001) and biopsies in dependent areas (OR 4.064, 95% CI 1.477-11.186, p < 0.001) independently increased hemorrhage risk.
Conclusions: GGOs in the access route and dependent lung area biopsies are independent risk factors for hemorrhage during CT-guided lung biopsy.
Keywords: biopsy; hemorrhage; image-guided biopsy; radiography interventional; risk factors; tomography.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures

References
-
- Nour-Eldin N.-E.A., Alsubhi M., Naguib N.N., Lehnert T., Emam A., Beeres M., Bodelle B., Koitka K., Vogl T.J., Jacobi V. Risk factor analysis of pulmonary hemorrhage complicating CT-guided lung biopsy in coaxial and non-coaxial core biopsy techniques in 650 patients. Eur. J. Radiol. 2014;83:1945–1952. - PubMed
-
- Tai R., Dunne R.M., Trotman-Dickenson B., Jacobson F.L., Madan R., Kumamaru K.K., Hunsaker A.R. Frequency and severity of pulmonary hemorrhage in patients undergoing percutaneous CT-guided transthoracic lung biopsy: Single-institution experience of 1175 cases. Radiology. 2016;279:287–296. doi: 10.1148/radiol.2015150381. - DOI - PubMed
-
- Tomiyama N., Yasuhara Y., Nakajima Y., Adachi S., Arai Y., Kusumoto M., Eguchi K., Kuriyama K., Sakai F., Noguchi M. CT-guided needle biopsy of lung lesions: A survey of severe complication based on 9783 biopsies in Japan. Eur. J. Radiol. 2006;59:60–64. doi: 10.1016/j.ejrad.2006.02.001. - DOI - PubMed

