The role of microbiota in the chronic prostatitis/chronic pelvis pain syndrome: a review
- PMID: 40143861
- PMCID: PMC11937130
- DOI: 10.3389/fmicb.2025.1488732
The role of microbiota in the chronic prostatitis/chronic pelvis pain syndrome: a review
Abstract
Chronic prostatitis/Chronic pelvis pain syndrome (CP/CPPS), a kind of frequent urinary condition among adult males, has caused a lot of inconvenience to patients in life, whose pathogenesis is unclear. Current evidence suggests that it is most likely to be an autoimmune disease. Symbiotic microbes, a highly diverse biological community that harbors trillions of microbes in each region of the human body, have gradually made people realize their important role in immune regulation, material metabolism, and health maintenance. In recent years, increasing studies have shown a connection between microbiota and CP/CPPS. In view of this, we performed this review to summarize the literature pertaining to microbiota and its association with the pathophysiological mechanism of CP/CPPS. In addition, we gleaned the latest progress in the therapeutic strategy of CP/CPPS that related to microbiota regulation in order to offer new perspectives on the management of CP/CPPS.
Keywords: CP/CPPS; microbiota; pathogenesis; treatment; treatment microbiota.
Copyright © 2025 Deng, Yue, Niu, Zhang, Hou, Zhang, Liang and Du.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
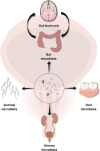
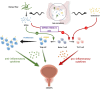
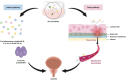
References
-
- Bartoletti R., Cai T., Mondaini N., Dinelli N., Pinzi N., Pavone C., et al. (2007). Prevalence, incidence estimation, risk factors and characterization of chronic prostatitis/chronic pelvic pain syndrome in urological hospital outpatients in Italy: Results of a multicenter case-control observational study. J. Urol. 178 2411–2415. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous

