A Dynamic Time Warping Extension to Consensus Weight-Based Cachexia Criteria Improves Prediction of Cancer Patient Outcomes
- PMID: 40151817
- PMCID: PMC11949122
- DOI: 10.1002/rco2.107
A Dynamic Time Warping Extension to Consensus Weight-Based Cachexia Criteria Improves Prediction of Cancer Patient Outcomes
Abstract
Background: Cachexia is a complex syndrome that impacts up to half of patients with cancer. Criteria systems have been developed for the purpose of diagnosing and grading cachexia severity in clinical settings. One of the most widely known is those developed by Fearon et al. in 2011, which utilizes body mass loss and body mass index (BMI) to determine the presence and extent of cachexia. One limitation of this system and other clinical cachexia scales is the lack of systematic methods for assessing cachexia severity longitudinally. We sought to develop an extension to the 2011 consensus criteria that categorizes cancer patients with respect to their temporal cachexia progression and assess its predictive capacity relative to the current time-agnostic system.
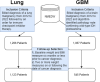
Methods: Two cancer cohorts were identified in electronic health record data: lung cancer and glioblastoma. We extracted weight and BMI measures from the time of cancer diagnosis until death or loss to follow-up and computed cachexia severity according to the consensus criteria. Subgroups of cachexia progression were uncovered using dynamic time warping (DTW) followed by unsupervised clustering. This system and baseline consensus criteria measurements were each assessed for their ability to stratify patient outcomes utilizing Kaplan-Meier curves and Cox proportional hazards and subsequently compared with model concordance and inverse probability of censoring weighting (IPCW).
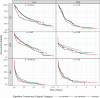
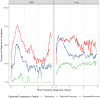
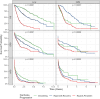
Results: Significant differences were observed in overall survival Kaplan-Meier curves of 1023 patients with lung cancer when stratified by baseline cachexia classification (p = 0.0002, N events = 592) but not in a cohort of 545 patients with glioblastoma (p = 0.16, N events = 353). DTW uncovered three patterns of cachexia progression in each subgroup with features described as 'smouldering', 'rapid with recovery' or 'persistent/recurrent'. Significant differences were observed in Kaplan-Meier curves when stratified by cachexia longitudinal patterns in lung cancer (p < 0.0001) and glioblastoma (p < 0.0001). Adjusted hazards ratios comparing the 'persistent/recurrent' cluster to referent subgroups in Cox models were 4.8 (4.1-5.8, p < 0.05) and 1.9 (1.4-2.4, p < 0.05) among patients with lung cancer and glioblastoma, respectively. Areas under the curve at multiple time points and Cox model concordances were greater when patients were stratified by progression pattern compared with baseline consensus criteria.
Conclusions: Our results suggest that accounting for cachexia's longitudinal progression in a systematic way can improve upon the prognostic capacity of a widely used consensus criteria set. These findings are important for the future development of systems that recognize concerning patterns of cachexia progression in clinical settings and aid clinicians in cachexia-related decision making.
Keywords: cancer cachexia; dynamic time warping; electronic health records.
© 2024 The Author(s). JCSM Communications published by Wiley Periodicals LLC.
Conflict of interest statement
Theresa Walunas receives unrelated research funding from Gilead Sciences.
Figures
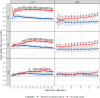
References
-
- Tisdale M. J., “Cachexia in Cancer Patients,” Nature Reviews Cancer 2, no. 11 (2002): 862–871. - PubMed
-
- Fearon K., Strasser F., Anker S. D., et al., “Definition and Classification of Cancer Cachexia: An International Consensus,” Lancet Oncology 12, no. 5 (2011): 489–495. - PubMed
-
- Buzby G. P., Mullen J. L., Matthews D. C., Hobbs C. L., and Rosato E. F., “Prognostic Nutritional Index in Gastrointestinal Surgery,” American Journal of Surgery 139, no. 1 (1980): 160–167. - PubMed
-
- Onodera T., Goseki N., and Kosaki G., “Prognostic Nutritional Index in Gastrointestinal Surgery of Malnourished Cancer Patients,” Nihon Geka Gakkai Zasshi 85, no. 9 (1984): 1001–1005. - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
