Effects of 12-week combined interval running and resistance training on cardiac structure and performance in patients with type 1 diabetes
- PMID: 40162367
- PMCID: PMC11954380
- DOI: 10.1177/20420188251325148
Effects of 12-week combined interval running and resistance training on cardiac structure and performance in patients with type 1 diabetes
Abstract
Background: Exercise has been suggested to effectively improve cardiac performance in children with type 1 diabetes (T1D) by enhancing the glycemic control. The purpose of this study was to investigate (1) effects of a 12-week combined interval running and resistance training (CIRRT) and (2) 1 month of detraining on cardiac structure and myocardial performance in adolescent males with T1D.
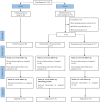
Methods: A total of 72 participants, including 48 adolescent males with T1D (fasting blood glucose (FBG): 274.67 ± 52.99 mg/dL, age: 15.20 ± 1.78 years) and 24 healthy adolescents (FBG: 90.75 ± 5.47 mg/dL, age: 15.08 ± 1.67 years), were recruited to the study. Participants were allocated into diabetes exercise (DE), diabetes control (DC), and healthy controls (HC) groups. The DE group performed 12 weeks of a CIRRT program three times per week. Blood glucose profile, echocardiography (ECHO) indices, and peak oxygen consumption (VO2peak) were measured pre- and post-intervention and following 1-month detraining period. Repeated measures ANOVA was used for pre- and post-intervention comparisons within the DE group and across the three study groups. Significance level was set at p < 0.05.
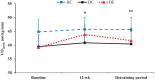
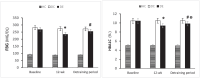
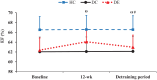
Results: Exercise intervention resulted in decreased hemoglobin A1c (HbA1c% = Pre: 10.44 ± 2.03, Post: 9.38 ± 1.66, p < 0.05), FBG, left ventricular (LV) internal diameter, and both tricuspid and mitral deceleration time (DT) in the DE group. VO2peak, ejection fraction (EF% = Pre: 62.38 ± 1.6, Post: 64.08 ± 1.18, p < 0.05), fractional shortening, early tricuspid diastolic inflow E velocity, and tricuspid velocity during atrial contraction were also increased following the exercise training. HbA1c (Pre vs Follow-up: 9.83 ± 1.73, p < 0.05), EF (Pre vs Follow-up: 62.97 ± 1.56, p < 0.05), LV, and DT tricuspid remained significantly improved after detraining period compared to the baseline. In the baseline, the glycemic index and ECHO variable significantly differed in the DE and DC groups with the HC group (p < 0.05). However, after the intervention, the DC and HC groups did not change significantly (p > 0.05).
Conclusion: The CIRRT intervention was associated with improved cardiac structure and performance in male adolescents with T1D potentially due to exercise-induced adaptations. Meanwhile, the results indicate that most cardiac morphological and functional changes are reversible following periods of inactivity in patients with T1D.
Keywords: VO2Peak; echocardiography; heart; interval running training; resistance training; type 1 diabetes.
© The Author(s), 2025.
Figures
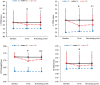
References
-
- Palmieri V, Capaldo B, Russo C, et al. Uncomplicated type 1 diabetes and preclinical left ventricular myocardial dysfunction: insights from echocardiography and exercise cardiac performance evaluation. Diabetes Res Clin Pract 2008; 79(2): 262–268. - PubMed
LinkOut - more resources
Full Text Sources

