Postpartum Hormonal Contraceptive Use and Risk of Depression
- PMID: 40163119
- PMCID: PMC11959440
- DOI: 10.1001/jamanetworkopen.2025.2474
Postpartum Hormonal Contraceptive Use and Risk of Depression
Abstract
Importance: Hormonal contraceptive (HC) use is associated with depression. It is, however, unknown whether this is also true in the postpartum period when women have a heightened depression risk and are routinely offered HC treatment.
Objective: To examine whether HC initiation post partum is associated with the development of depression within 12 months post partum.
Design, setting, and participants: A population-based cohort study based on nationwide Danish register data was conducted including all primiparous women who gave birth from January 1, 1997, through December 31, 2022. Women were excluded if they had depression within 24 months before delivery, multiple births or stillbirth, or a diagnosis of breast cancer or liver tumor. Data analysis was conducted between March 20, 2023, and January 17, 2025.
Exposure: Hormonal contraceptive initiation within 12 months post partum was treated as a time-varying exposure. Hormonal contraceptive types were categorized as combined oral contraceptives (COCs), combined nonoral contraceptives (CNOCs), progestogen-only pills (POPs), and progestogen-only nonoral contraceptives (PNOCs).
Main outcomes and measures: Depression within 12 months post partum, defined as filling an antidepressant prescription or receiving a hospital diagnosis of depression, was the main outcome. Adjusted hazard ratios (AHRs) and average absolute risks of depression within 12 months post partum were estimated using Cox proportional hazards regression and a G-formula estimator.
Results: Of 610 038 first-time mothers, 248 274 (40.7%) initiated HCs within 12 months post partum (mean [SD] age, 27.6 [4.3] years for HC users vs 29.6 [4.8] years for nonusers). Hormonal contraceptive initiation was associated with subsequent depression, with an AHR of 1.49 (95% CI, 1.42-1.56) compared with no use, resulting in an increase in the 12-month absolute risk from 1.36% (95% CI, 1.32%-1.39%) to 1.54% (95% CI, 1.50%-1.57%). The AHR for COC was 1.72 (95% CI, 1.63-1.82); CNOC, 1.97 (95% CI, 1.64-2.36); and PNOC, 1.40 (95% CI, 1.25-1.56). Progestogen-only pill exposure was associated with an instantaneously reduced risk in the early study period, but it was increased late post partum. The earlier COCs were initiated post partum the higher the associated rate ratio of depression.
Conclusions and relevance: In this cohort study, HC initiation post partum was associated with an instantaneous increased risk of developing depression. The associated risk was higher the earlier it was initiated post partum, at least for COC. This finding raises the issue of whether the incidence of depression post partum is increased by routine HC initiation after childbirth.
Conflict of interest statement
Figures

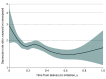
References
-
- O’Hara MW, Swain AM. Rates and risk of postpartum depression—a meta-analysis. Int Rev Psychiatry. 1996;8(1):37-54. doi:10.3109/09540269609037816 - DOI

