Epicardial ventricular arrhythmia ablation: a clinical consensus statement of the European Heart Rhythm Association of the European Society of Cardiology and the Heart Rhythm Society, the Asian Pacific Heart Rhythm Society, the Latin American Heart Rhythm Society, and the Canadian Heart Rhythm Society
- PMID: 40163515
- PMCID: PMC11956854
- DOI: 10.1093/europace/euaf055
Epicardial ventricular arrhythmia ablation: a clinical consensus statement of the European Heart Rhythm Association of the European Society of Cardiology and the Heart Rhythm Society, the Asian Pacific Heart Rhythm Society, the Latin American Heart Rhythm Society, and the Canadian Heart Rhythm Society
Abstract
Epicardial access during electrophysiology procedures offers valuable insights and therapeutic options for managing ventricular arrhythmias (VAs). The current clinical consensus statement on epicardial VA ablation aims to provide clinicians with a comprehensive understanding of this complex clinical scenario. It offers structured advice and a systematic approach to patient management. Specific sections are devoted to anatomical considerations, criteria for epicardial access and mapping evaluation, methods of epicardial access, management of complications, training, and institutional requirements for epicardial VA ablation. This consensus is a joint effort of collaborating cardiac electrophysiology societies, including the European Heart Rhythm Association, the Heart Rhythm Society, the Asia Pacific Heart Rhythm Society, the Latin American Heart Rhythm Society, and the Canadian Heart Rhythm Society.
Keywords: Cardiomyopathies; Catheter ablation; Clinical consensus statement; Electrophysiology procedures; Epicardial access; Ventricular arrhythmias; Ventricular fibrillation; Ventricular tachycardia.
© the European Society of Cardiology 2025.
Conflict of interest statement
Conflict of interest: All members provided disclosure statements to assess potential conflicts of interest. Details are available in the Supplementary material.
Figures

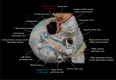


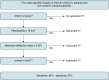
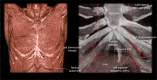

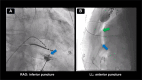
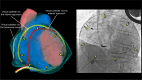
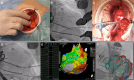
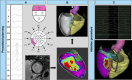
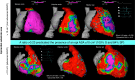


References
-
- Romero J, Cerrud-Rodriguez RC, Di Biase L, Diaz JC, Alviz I, Grupposo V et al. Combined endocardial–epicardial versus endocardial catheter ablation alone for ventricular tachycardia in structural heart disease: a systematic review and meta-analysis. JACC Clin Electrophysiol 2019;5:13–24. - PubMed
-
- Romero J, Patel K, Briceno D, Alviz I, Gabr M, Diaz JC et al. Endo-epicardial ablation vs endocardial ablation for the management of ventricular tachycardia in arrhythmogenic right ventricular cardiomyopathy: a systematic review and meta-analysis. J Cardiovasc Electrophysiol 2020;31:2022–31. - PubMed
-
- Shirai Y, Liang JJ, Santangeli P, Arkles JS, Schaller RD, Supple GE et al. Comparison of the ventricular tachycardia circuit between patients with ischemic and nonischemic cardiomyopathies: detailed characterization by entrainment. Circ Arrhythm Electrophysiol 2019;12:e007249. - PubMed
-
- Aryana A, Tung R, d'Avila A. Percutaneous epicardial approach to catheter ablation of cardiac arrhythmias. JACC Clin Electrophysiol 2020;6:1–20. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

