Associations between cardiometabolic indices and the onset of metabolic dysfunction-associated steatotic liver disease as well as its progression to liver fibrosis: a cohort study
- PMID: 40181314
- PMCID: PMC11969729
- DOI: 10.1186/s12933-025-02716-6
Associations between cardiometabolic indices and the onset of metabolic dysfunction-associated steatotic liver disease as well as its progression to liver fibrosis: a cohort study
Abstract
Background: This study sought to examine the associations between cardiometabolic indices and the onset of metabolic dysfunction-associated steatotic liver disease (MASLD) as well as its progression to liver fibrosis.
Methods: This study comprised 25,366 subjects aged 18 years and older, free of MASLD at baseline, from the Dalian Health Management Cohort (DHMC). Cardiometabolic indices include cardiometabolic index (CMI), atherogenic index of plasma (AIP), triglyceride glucose (TyG), triglyceride glucose-body mass index (TyG-BMI), triglyceride glucose-waist circumference (TyG-WC) and triglyceride glucose-waist height ratio (TyG-WHtR). All participants were categorized into quartile groups based on cardiometabolic indices. Cox proportional hazards regression models and restricted cubic splines were employed to examine the relationship between cardiometabolic indices and the incidence of MASLD as well as its progression to liver fibrosis, and analyses were performed between different subgroups. Mediation analysis was employed to explore how obesity and inflammation serve as mediators in the connection between cardiometabolic indices and MASLD. To evaluate the predictive ability of cardiometabolic indices for the onset of MASLD, the time-dependent receiver operating characteristic (ROC) curve was utilized.
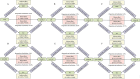
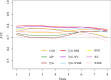
Results: A total of 5378 (21.2%) individuals developed MASLD during the follow-up period of 82,445 person-years. Multivariates Cox regression analyses showed that participants in the highest quartile of cardiometabolic indices had greater risk of MASLD than those in the lowest quartile (CMI: HR = 6.11, 95% CI 5.45-6.86; AIP: HR = 4.58, 95% CI 4.11-5.10; TyG: HR = 3.55, 95% CI 3.21-3.92; TyG-BMI: HR = 13.55, 95% CI 11.80-15.57; TyG-WC: HR = 12.52, 95% CI 10.93-14.34; TyG-WHtR: HR = 11.37, 95% CI 9.96-12.98). TyG-BMI (HR = 1.36, 95% CI 1.18-1.57), but not other cardiometabolic indices, was associated with liver fibrosis. Mediation analysis indicated that BMI mediated 40.4%, 33.2%, 36.5%, - 10.4%, 37.4%, 48.5% of the associations between CMI, AIP, TyG, TyG-BMI, TyG-WC, TyG-WHtR and MASLD. Time-dependent ROC curves demonstrated that TyG-BMI had a superior predictive ability for MASLD onset compared to other indicators.
Conclusions: The risk of developing MASLD increases as the level of cardiometabolic indices increases. Obesity may serve as a mediating factor in the aforementioned association. TyG-BMI showed the strongest association with the onset of MASLD and its progression to liver fibrosis, proved to be outperformed other cardiometabolic indicators, and could be the best clinical non-invasive biomarker for early screening of MASLD and liver fibrosis.
Keywords: Cardiometabolic index; Insulin resistance; Liver fibrosis; Metabolic dysfunction-associated steatotic liver disease; Triglyceride-glucose.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: This study adhered to the Declaration of Helsinki and was approved by the Ethics Review Committee of the Second Hospital of Dalian Medical University (2022064). All participants provided informed consent. Consent for publication: Not applicable. Competing interests: The authors declare no competing interests.
Figures

Similar articles
-
Association between triglyceride-glucose (TyG) related indices and cardiovascular diseases and mortality among individuals with metabolic dysfunction-associated steatotic liver disease: a cohort study of UK Biobank.Cardiovasc Diabetol. 2025 Jan 13;24(1):12. doi: 10.1186/s12933-024-02572-w. Cardiovasc Diabetol. 2025. PMID: 39806394 Free PMC article.
-
Association between triglyceride-glucose related indices and mortality among individuals with non-alcoholic fatty liver disease or metabolic dysfunction-associated steatotic liver disease.Cardiovasc Diabetol. 2024 Jul 4;23(1):232. doi: 10.1186/s12933-024-02343-7. Cardiovasc Diabetol. 2024. PMID: 38965572 Free PMC article.
-
Prognostic effect of triglyceride glucose-related parameters on all-cause and cardiovascular mortality in the United States adults with metabolic dysfunction-associated steatotic liver disease.Cardiovasc Diabetol. 2024 Jun 1;23(1):188. doi: 10.1186/s12933-024-02287-y. Cardiovasc Diabetol. 2024. PMID: 38824550 Free PMC article.
-
Association of triglyceride glucose-body mass index (TyG-BMI) with metabolic dysfunction-associated steatotic liver disease: A systematic review and meta-analysis.PLoS One. 2025 Aug 4;20(8):e0324483. doi: 10.1371/journal.pone.0324483. eCollection 2025. PLoS One. 2025. PMID: 40758732 Free PMC article.
-
Metabolically Healthy Obesity and Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD): Navigating the Controversies in Disease Development and Progression.Curr Obes Rep. 2025 May 19;14(1):46. doi: 10.1007/s13679-025-00637-9. Curr Obes Rep. 2025. PMID: 40387999 Free PMC article. Review.
References
-
- European Association for the Study of the Liver. Electronic address: easloffice@ easloffice.eu, European Association for the Study of Diabetes, European Association for the Study of Obesity, et al. EASL-EASD-EASO Clinical Practice Guidelines on the management of metabolic dysfunction-associated steatotic liver disease (MASLD). J Hepatol. 2024;81(3):492–542. - PubMed
-
- Mantovani A, Scorletti E, Mosca A, et al. Complications, morbidity and mortality of nonalcoholic fatty liver disease. Metabolism. 2020;111S: 154170. - PubMed
-
- Miao L, Targher G, Byrne CD, et al. Current status and future trends of the global burden of MASLD. Trends Endocrinol Metab. 2024;35(8):697–707. - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

