The effect of pre-operative MRI on the in-breast tumor recurrence rate of patients with breast cancer: a meta-analysis
- PMID: 40183820
- PMCID: PMC11971173
- DOI: 10.1007/s00423-025-03691-y
The effect of pre-operative MRI on the in-breast tumor recurrence rate of patients with breast cancer: a meta-analysis
Abstract
Purpose: The impact of preoperative MRI on breast cancer recurrence and long-term outcomes remains undefined. Therefore, this study aims at determining the influence of preoperative MRI on in-breast tumor recurrence rates in cases of surgical treatment for breast cancer.
Methods: A systematic review and meta-analysis were performed. Literature searches of PubMed, Scopus, and Google Scholar were conducted for studies up to February 2024. Two authors assessed the quality of the eligible studies and extracted their data.
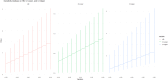
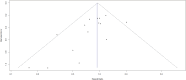
Results: The meta-analysis included 14 studies (2 RCTs, 12 cohort studies) with 12,889 patients with 5,451 undergoing preoperative MRI. Pooled hazard ratio for in-breast tumor recurrence was 0.95, using fixed effects and 0.94 using random effects models with 95% confidence intervals of 0.80-1.14 and 0.77-1.14, respectively. A trend towards lower recurrence rates in the MRI group was seen, but the reduction was not statistically significant.
Conclusion: This meta-analysis found no significant reduction in in-breast tumor recurrence rates associated with preoperative MRI use in breast cancer patients, consistent with previous findings.
Keywords: Breast neoplasms; Magnetic resonance imaging; Meta-analysis; Preoperative evaluation; Recurrence.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: Not applicable. Consent for publication: Not applicable. Competing interests: The authors declare no competing interests.
Figures


References
-
- Pittinger TP, Maronian NC, Poulter CA, Peacock JL (1994) Importance of margin status in outcome of breast-conserving surgery for carcinoma. Surgery. 116(4):605-8 discussion 8–9 - PubMed
-
- Tartter PI, Kaplan J, Bleiweiss I, Gajdos C, Kong A, Ahmed S et al (2000) Lumpectomy margins, reexcision, and local recurrence of breast cancer. Am J Surg 179(2):81–85. 10.1016/s0002-9610(00)00272-5 - PubMed
-
- Houssami N, Macaskill P, Marinovich ML, Dixon JM, Irwig L, Brennan ME et al (2010) Meta-analysis of the impact of surgical margins on local recurrence in women with early-stage invasive breast cancer treated with breast-conserving therapy. Eur J Cancer 46(18):3219–3232. 10.1016/j.ejca.2010.07.043 - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

