Osteosarcopenia in Chronic Kidney Disease: An Overlooked Syndrome?
- PMID: 40192621
- PMCID: PMC11974265
- DOI: 10.1002/jcsm.13787
Osteosarcopenia in Chronic Kidney Disease: An Overlooked Syndrome?
Abstract
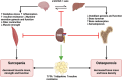
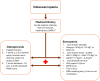
Background: Healthy ageing relies on maintaining physiological systems, particularly the musculoskeletal system (MKS). After 50, declines in bone density, muscle mass and strength increase the risk of osteoporosis and sarcopenia, leading to frailty, fractures and higher healthcare costs. Osteosarcopenia, combining osteoporosis and sarcopenia, is rising because of the ageing population. Chronic kidney disease (CKD) exacerbates this condition through disruptions in mineral metabolism, hormonal imbalances and inflammation, further compromising musculoskeletal health.
Aims: This review examines the pathophysiology of osteosarcopenia associated with CKD, focusing on the role of mineral and hormonal disturbances, chronic inflammation and endocrine dysfunction. It aims to increase clinical awareness and highlight the need for early diagnosis and intervention to mitigate the burden of osteosarcopenia on the quality of life and healthcare systems in ageing CKD populations.
Methods: A narrative review of the current literature was conducted, summarising evidence on the mechanisms underlying osteosarcopenia in CKD, including mineral metabolism alterations, inflammatory processes and hormonal imbalances.
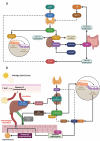
Results: Osteosarcopenia is a recognised consequence of CKD, contributing to increased morbidity and mortality. The pathophysiology of osteosarcopenia in CKD is multifactorial, involving disruptions in mineral metabolism, inflammation, endocrine dysfunction and physical inactivity. CKD-mineral and bone disorder (CKD-MBD) leads to alterations in calcium, phosphate, parathyroid hormone (PTH), fibroblast growth factor 23 (FGF-23) and vitamin D metabolism, resulting in impaired bone mineralisation and increased fracture risk. Simultaneously, CKD accelerates muscle wasting through systemic inflammation, anabolic resistance and metabolic derangements, increasing the risk of sarcopenia. Sarcopenic obesity, inflammaging and hormonal dysregulation further exacerbate bone muscle deterioration. Emerging evidence suggests that osteosarcopenia in CKD is a consequence of interconnected pathophysiological pathways rather than isolated conditions. Diagnosis remains challenging because of overlapping clinical features, necessitating integrated assessment tools. Targeted therapeutic strategies, including mineral metabolism correction, resistance exercise and anabolic interventions, are essential to mitigate osteosarcopenia's progression and improve patient outcomes in CKD.
Conclusions: Osteosarcopenia is a growing concern in ageing CKD populations. Early diagnostic strategies and targeted interventions are essential to mitigate the impact of osteosarcopenia on patient outcomes and reduce associated healthcare costs. Increased clinical awareness and research into effective therapies are crucial for improving the quality of life for individuals affected by CKD and osteosarcopenia.
Keywords: chronic kidney disease (CKD); mineral bone disorder (MBD); osteoporosis; osteosarcopenia; sarcopenia.
© 2025 The Author(s). Journal of Cachexia, Sarcopenia and Muscle published by Wiley Periodicals LLC.
Conflict of interest statement
Simone Vettoretti served as a consultant at advisory boards for Merk Sharp & Dohme, Astra Zeneca, Boehringer and Ingelheim and held a sponsored lecture by Dr. Shär. Lara Caldiroli worked as a consultant for Dr. Shär.
Figures