Feasibility and impact of a patient support group care model on diabetes and hypertension care in informal settlements in Nairobi, Kenya: a quasi-experimental study
- PMID: 40200831
- PMCID: PMC11983520
- DOI: 10.1080/16549716.2025.2482304
Feasibility and impact of a patient support group care model on diabetes and hypertension care in informal settlements in Nairobi, Kenya: a quasi-experimental study
Abstract
Background: A support group care model including self-financing is a promising strategy to improve care for patients with diabetes or hypertension in resource-constrained settings.
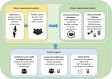
Objectives: We investigated the uptake, feasibility, and impact of a self-financing patient support group care model on cardiometabolic parameters among adult patients with uncontrolled diabetes or hypertension in informal settlements in Nairobi, Kenya.
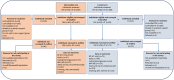
Methods: A two-group prospective quasi-experimental study was conducted. The outcomes were changes in mean glycated haemoglobin (HbA1c), systolic blood pressure (SBP), diastolic blood pressure (DBP), body mass index, and waist-hip ratio in control versus intervention communities, assessed 6 months after intervention implementation.
Results: At baseline, 118 patients with diabetes (intervention, 60; control, 58) and 176 with hypertension (intervention, 87; control, 89) were enrolled. At endline, 81 patients with diabetes and 137 with hypertension were surveyed. In the intervention arm, HbA1c decreased from 10.8% to 9.0% (mean difference [95% CI]: -1.7 [-2.4, -0.9] p < 0.001) and in the control arm from 10.6% to 9.9% (-0.9 [-1.5, -0.3] p = 0.005). Difference-in-difference analysis showed a notably greater reduction in HbA1c in the intervention arm (-0.942 [0.463] p < 0.05). In the intervention arm, SBP decreased from 155.0 mmHg to 148.7 mmHg (-6.3 [-11.7, -0.9] p = 0.022) and in the control arm, from 160.1 mmHg to 152.5 mmHg (-7.6 [-12.9, -2.3] p = 0.005). DBP in the intervention arm changed from 99.1 mmHg to 97.9 mmHg (-1.1 [4.2, 1.9] p = 0.462) and in the control arm from 99.7 mmHg to 94.8 mmHg (-4.9 [7.8, -2.0] p = 0.001).
Conclusions: A self-financing patient support group care model is feasible, improves cardiometabolic parameters and can be a strategy to manage diabetes, hypertension, and other chronic diseases in low-resource settings.
Keywords: Africa; Hypertension; diabetes; low- and middle-income countries; patient support groups; self-financing.
Plain language summary
Main findings: A co-created self-financing patient support group care model tested for 6 months among patients with uncontrolled diabetes or hypertension in informal settlements in Nairobi, Kenya, resulted in substantial reductions in glycated haemoglobin and blood pressure.Added knowledge: A self-financing patient support group care model for diabetes and hypertension is feasible and can impact disease outcomes in low-resource settings.Global health impact for policy and action: The self-financing patient support group care model is an additional toolkit to manage diabetes and hypertension in resource-limited settings and can be adapted for other chronic diseases.
Conflict of interest statement
No potential conflict of interest was reported by the author(s)s.
Figures
Similar articles
-
Impact of Bridging Income Generation with Group Integrated Care (BIGPIC) on Hypertension and Diabetes in Rural Western Kenya.J Gen Intern Med. 2017 May;32(5):540-548. doi: 10.1007/s11606-016-3918-5. Epub 2016 Dec 5. J Gen Intern Med. 2017. PMID: 27921256 Free PMC article.
-
Effect of a Collaborative Care Model on Depressive Symptoms and Glycated Hemoglobin, Blood Pressure, and Serum Cholesterol Among Patients With Depression and Diabetes in India: The INDEPENDENT Randomized Clinical Trial.JAMA. 2020 Aug 18;324(7):651-662. doi: 10.1001/jama.2020.11747. JAMA. 2020. PMID: 32809002 Free PMC article. Clinical Trial.
-
Effectiveness of a Health Coaching Intervention for Patient-Family Dyads to Improve Outcomes Among Adults With Diabetes: A Randomized Clinical Trial.JAMA Netw Open. 2022 Nov 1;5(11):e2237960. doi: 10.1001/jamanetworkopen.2022.37960. JAMA Netw Open. 2022. PMID: 36374502 Free PMC article. Clinical Trial.
-
Assessment of Interprofessional Collaborative Practices and Outcomes in Adults With Diabetes and Hypertension in Primary Care: A Systematic Review and Meta-analysis.JAMA Netw Open. 2021 Feb 1;4(2):e2036725. doi: 10.1001/jamanetworkopen.2020.36725. JAMA Netw Open. 2021. PMID: 33576817 Free PMC article.
-
The effect of integrated health care in patients with hypertension and diabetes: a systematic review and meta-analysis.BMC Health Serv Res. 2022 May 5;22(1):603. doi: 10.1186/s12913-022-07838-1. BMC Health Serv Res. 2022. PMID: 35513809 Free PMC article.
References
-
- Fisher EB, Boothroyd RI, Elstad EA, et al. Peer support of complex health behaviors in prevention and disease management with special reference to diabetes: systematic reviews. Clin Diabetes Endocrinol. 2017;3:4. Epub 20170525. doi: 10.1186/s40842-017-0042-3 PubMed PMID: 28702258; PubMed Central PMCID: PMC5471959. - DOI - PMC - PubMed
-
- Werfalli M, Raubenheimer PJ, Engel M, et al. The effectiveness of peer and community health worker-led self-management support programs for improving diabetes health-related outcomes in adults in low- and-middle-income countries: a systematic review. Syst Rev. 2020;9:133. Epub 20200606. doi: 10.1186/s13643-020-01377-8 PubMed PMID: 32505214; PubMed Central PMCID: PMC7275531. - DOI - PMC - PubMed
-
- World Health Organisation . Hypertension; 2023. Available from: https://www.who.int/news-room/fact-sheets/detail/hypertension
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical