Frequency and Outcomes of Acute Kidney Injury in the First Month Post-transplant: A Study on Renal Transplant Recipients in a Resource-Limited Country
- PMID: 40201867
- PMCID: PMC11976677
- DOI: 10.7759/cureus.80277
Frequency and Outcomes of Acute Kidney Injury in the First Month Post-transplant: A Study on Renal Transplant Recipients in a Resource-Limited Country
Abstract
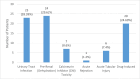
Objective The study aimed to determine the incidence of acute kidney injury (AKI) in renal transplant recipients in the first month after transplant. The number of AKI episodes per patient and their outcome on renal graft function were also determined. Material and methods It is a retrospective study that took place in the Nephrology Department of Pakistan Kidney and Liver Institute and Research Center (PKLI & RC), Lahore, Pakistan. A total of 195 patients aged 18-70 years who underwent kidney transplant surgery at PKLI & RC, Lahore, were selected in this cohort that underwent renal transplants from 31st January 2024 to 31st December 2024. One month post-transplant course was followed by obtaining serum creatinine level values. Data was analyzed using Microsoft Excel (Microsoft® Corp., Redmond, WA, USA). Results A total of 81 out of 195 patients (41.5%) had AKI within the first 30 days following a renal transplant. Seventy patients experienced AKI once (86.4%), meanwhile, 11 patients (13.5%) had two episodes of AKI within the first 30 days. Staging done as per Kidney Disease Improving Global Outcomes (KDIGO) guidelines showed that 73 patients had stage I AKI (90.1%). Three patients had stage II AKI (3.7%), while five patients had stage III AKI (6.2%). The most common cause was found to be pre-renal (dehydration) in 24 patients out of 81 (29.6%) and followed by a urinary tract infection in 23 patients (28.3%). Twenty patients (24.6%) had drug-induced AKI; there was calcineurin inhibitor (CNI) toxicity in 8.6% and acute tubular necrosis (ATN) in 7.4% of patients. One patient had acute antibody-mediated rejection (ABMR). Most cases of AKI were found to be self-limiting, with complete resolution to baseline renal allograft function. Conclusion Even though most episodes of AKI completely resolved to baseline creatinine, it is pivotal to timely diagnose and treat AKI in post-renal transplant patients. If left untreated, there can be a worsening of graft function and overall outcome of the transplant.
Keywords: acute kidney injury; cni toxicity; kidney transplant; post-renal transplant; serum creatinine; urinary tract infection.
Copyright © 2025, Zafar et al.
Conflict of interest statement
Human subjects: Consent for treatment and open access publication was obtained or waived by all participants in this study. Animal subjects: All authors have confirmed that this study did not involve animal subjects or tissue. Conflicts of interest: In compliance with the ICMJE uniform disclosure form, all authors declare the following: Payment/services info: All authors have declared that no financial support was received from any organization for the submitted work. Financial relationships: All authors have declared that they have no financial relationships at present or within the previous three years with any organizations that might have an interest in the submitted work. Other relationships: All authors have declared that there are no other relationships or activities that could appear to have influenced the submitted work.
Figures
References
-
- Prevalence and disease burden of chronic kidney disease. Lv JC, Zhang LX. https://link.springer.com/chapter/10.1007/978-981-13-8871-2_1. Adv Exp Med Biol. 2019;1165:3–15. - PubMed
-
- Predictors of post-kidney transplantation complications among Egyptian recipients - 1-year follow-up. Abdelaziz EM, Darwish MM, Taie AG, et al. Egypt J Intern Med. 2024;36:68.
-
- Incidence and risk factors of infections following kidney transplantation. Alotaibi NE. J Infect Public Health. 2024;17:102491. - PubMed
LinkOut - more resources
Full Text Sources