Epidemiology of sepsis in hospitalised neonates in Indonesia: high burden of multidrug-resistant infections reveals poor coverage provided by recommended antibiotic regimens
- PMID: 40204461
- PMCID: PMC11987146
- DOI: 10.1136/bmjgh-2024-016272
Epidemiology of sepsis in hospitalised neonates in Indonesia: high burden of multidrug-resistant infections reveals poor coverage provided by recommended antibiotic regimens
Abstract
Background: Neonatal sepsis is a leading cause of child mortality, and this burden is rising secondary to increasing antimicrobial resistance worldwide. There are marked global disparities in the burden of antimicrobial resistance, with Southeast Asia identified as a region of particular concern. Indonesia is the world's fourth most populous country, with 4.2 million babies born each year. Despite this, there remains limited published data on the burden of neonatal sepsis and antimicrobial resistance in the country.
Methods: We conducted a 2-year analysis of the epidemiology of neonatal sepsis across three high-burden clinical settings in Indonesia, alongside an antibiotic point prevalence prescribing survey.
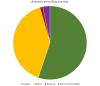
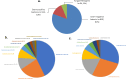
Results: Of 5439 blood cultures analysed, gram-negative bacteria predominated as causative pathogens for neonatal sepsis in Indonesia, with Klebsiella spp and Acinetobacter spp most common (prevalence 35% and 19%, respectively). Overall, the pathogens causing neonatal sepsis exhibit very low susceptibility to WHO-recommended antibiotic regimens for the treatment of neonatal sepsis, with only 25% coverage provided by aminopenicillins plus gentamicin (95% credible interval (CI) 22% to 29%) and 20% by third-generation cephalosporins (95% CI 17% to 23%). Almost half of all antibiotics prescribed to treat neonatal sepsis across the clinical settings included in our study were Watch and Reserve antibiotics.
Conclusion: Our multicentre study across three sites in Indonesia revealed neonatal sepsis is predominantly caused by Gram-negative pathogens, with very poor coverage provided by currently recommended empiric regimens. A high burden of multidrug-resistant pathogens drives empirical use of broad-spectrum antibiotics. There is an urgent need for new antibiotic regimens and infection prevention and control strategies to treat neonatal sepsis in regions with a high prevalence of multidrug-resistant infections.
Keywords: Blood disorders; Child health; Global Health; Infections, diseases, disorders, injuries; Public Health.
© Author(s) (or their employer(s)) 2025. Re-use permitted under CC BY. Published by BMJ Group.
Conflict of interest statement
Competing interests: None declared.
Figures

References
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous
