Novel deep learning algorithm based MRI radiomics for predicting lymph node metastases in rectal cancer
- PMID: 40204902
- PMCID: PMC11982536
- DOI: 10.1038/s41598-025-96618-y
Novel deep learning algorithm based MRI radiomics for predicting lymph node metastases in rectal cancer
Abstract
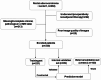
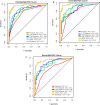
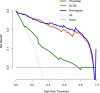
To explore the value of applying the MRI-based radiomic nomogram for predicting lymph node metastasis (LNM) in rectal cancer (RC). This retrospective analysis used data from 430 patients with RC from two medical centers. The patients were categorized into the LNM negative (LNM-) and LNM positive (LNM+) according to their surgical pathology results. We developed a physician model by selecting clinical independent predictors through physician assessments. Additionally, we developed deep learning radscore (DLRS) models by extracting deep features from multiparametric MRI (mpMRI) images. A nomogram model was constructed by combining the physician model and DLRS models. Among the patients, 192 (44.65%, 192/430) experienced LNM+. Six prediction models were developed, namely the physician model, three sequence models, the DLRS, and the nomogram. The physician model achieved AUC of the receiver operating characteristic (ROC) values of 0.78, 0.79, and 0.7, whereas the sequence models, DLRS model, and nomogram model achieved AUC values ranging from 0.83 to 0.99. The predictive performance of the DLRS and nomogram models was superior to that of the physician model. DLRS and nomogram models based on mpMRI provided higher accuracy in predicting LNM status in patients with RC than the other models.
Keywords: Deep learning; Lymph node metastasis; Magnetic resonance imaging; Rectal cancer.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Competing interests: The authors declare no competing interests.
Figures



Similar articles
-
Deep Learning Algorithm‑Based MRI Radiomics and Pathomics for Predicting Microsatellite Instability Status in Rectal Cancer: A Multicenter Study.Acad Radiol. 2025 Apr;32(4):1934-1945. doi: 10.1016/j.acra.2024.09.008. Epub 2024 Sep 16. Acad Radiol. 2025. PMID: 39289097
-
Novel deep learning radiomics nomogram-based multiparametric MRI for predicting the lymph node metastasis in rectal cancer: A dual-center study.J Cancer Res Clin Oncol. 2024 Oct 9;150(10):450. doi: 10.1007/s00432-024-05986-x. J Cancer Res Clin Oncol. 2024. PMID: 39379733 Free PMC article.
-
Multiparametric MRI-based radiomics nomogram for the preoperative prediction of lymph node metastasis in rectal cancer: A two-center study.Eur J Radiol. 2024 Sep;178:111591. doi: 10.1016/j.ejrad.2024.111591. Epub 2024 Jun 25. Eur J Radiol. 2024. PMID: 39013271
-
Prediction of peripheral lymph node metastasis (LNM) in thyroid cancer using delta radiomics derived from enhanced CT combined with multiple machine learning algorithms.Eur J Med Res. 2025 Mar 13;30(1):164. doi: 10.1186/s40001-025-02438-1. Eur J Med Res. 2025. PMID: 40075509 Free PMC article.
-
Multiparametric MRI-Based Radiomics Nomogram for Predicting Lymph Node Metastasis in Early-Stage Cervical Cancer.J Magn Reson Imaging. 2020 Sep;52(3):885-896. doi: 10.1002/jmri.27101. Epub 2020 Feb 25. J Magn Reson Imaging. 2020. PMID: 32096586
Cited by
-
A novel MRI-based habitat analysis and deep learning for predicting perineural invasion in prostate cancer: a two-center study.BMC Cancer. 2025 Aug 23;25(1):1367. doi: 10.1186/s12885-025-14759-9. BMC Cancer. 2025. PMID: 40849663 Free PMC article.
-
Explanation and Elaboration with Examples for METRICS (METRICS-E3): an initiative from the EuSoMII Radiomics Auditing Group.Insights Imaging. 2025 Aug 13;16(1):175. doi: 10.1186/s13244-025-02061-y. Insights Imaging. 2025. PMID: 40802002 Free PMC article.
References
-
- Bray, F. et al. Global cancer statistics 2022: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J. Clin.74, 229–263 (2024). - PubMed
-
- Ao, W. et al. Value of apparent diffusion coefficient for assessing preoperative T staging of low rectal cancer and whether this is correlated with Ki-67 expression. Can. Assoc. Radiol. J.71, 5–11 (2020). - PubMed
-
- Ciardiello, F. et al. Clinical management of metastatic colorectal cancer in the era of precision medicine. CA Cancer J. Clin.72, 372–401 (2022). - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

