Use of psychotropic medications among glioma patients in Denmark, Norway, Sweden, and Wales
- PMID: 40208515
- PMCID: PMC12106481
- DOI: 10.1007/s11060-025-04996-0
Use of psychotropic medications among glioma patients in Denmark, Norway, Sweden, and Wales
Abstract
Purpose: Glioma patients often suffer from psychiatric and neurological conditions. However, little is known about the patterns of use of psychotropic drugs pre- and post-glioma diagnosis. Therefore, we assessed temporal patterns of psychotropic prescriptions among glioma patients, compared to an age and sex matched comparison cohort in four European countries.
Methods: Incident gliomas were identified in Wales from the Secured Anonymized Information Linkage Databank (2005-2016) and population-based registries in Denmark (2001-2016), Norway (2006-2019), and Sweden (2008-2018). From each data source, a cancer-free comparison cohort was matched to the glioma cases by age and sex. We calculated rates of new psychotropic prescriptions and any psychotropic prescriptions during the 2 years prior to and post glioma diagnosis. Analyses were stratified by histological subtypes and subclasses of psychotropic medications.
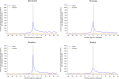
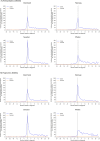
Results: We identified 16,007 glioma patients. The rate of new psychotropic drug use increased from 7 months before diagnosis, peaking around the month of glioma diagnosis (with peak rates ranging from 227 to 753 new psychotropic drugs per 1000 person-months). New use remained substantially higher among glioma patients than comparators throughout the 2-year follow-up period after glioma diagnosis, though rates of new use continued to decline throughout. New use was largely driven by antiepileptics, anxiolytics, hypnotics, and sedatives. Patterns were similar when analyses were stratified by histological subtype.
Conclusion: Psychotropic drug use among glioma patients was high, and elevations observed around the time of cancer diagnosis, largely driven by antiepileptics, anxiolytics, hypnotics, and sedatives, are likely associated with the consequences of the disease.
Keywords: Anticonvulsants; Brain tumor; Glioma; Hypnotics; Psychotropics.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Conflicts of interest: AP reports participation in research projects funded by Alcon, Almirall, Astellas, Astrazeneca, Boehringer-Ingelheim, Novo Nordisk, Servier, and LEO Pharma, all regulator-mandated phase IV-studies, all with funds paid to the institution where he was employed (no personal fees) and with no relation to the work reported in this paper. ML, JE and JR report participation in research projects funded by Janssen, Swedish Orphan BioVitrum (SOBI), Bayer, Novartis, AbbVie, Novo Nordisk, Pfizer, all with funds paid to the institution where they were employed (no personal fees) and with no relation to the work reported in this paper. JI reports participation in regulator-mandated post-authorisation safety studies (PASS) funded by Sanofi, Pfizer and Novartis, all with funds paid to the institution where she was employed (no personal fees). AL reports participation in PASS funded by Amgen, Sanofi, Pfizer and Novartis, all with funds paid to the institution where she was employed (no personal fees)]. Ethical approval: Approval was obtained for each of the individual datasets from: the Information Governance Review Panel (Wales), the Danish Data Protection Agency, the Regional Committee for Medical and Health Research Ethics (2018/2125/REK vest) (Norway), and the Swedish Ethical Authority, Statistics Sweden and the Swedish National Board of Health and Welfare].
Figures



Similar articles
-
Risk for use of antidepressants, anxiolytics, and hypnotics in partners of glioma patients-A nationwide study covering 19 years of prescriptions.Psychooncology. 2018 Aug;27(8):1930-1936. doi: 10.1002/pon.4744. Epub 2018 May 21. Psychooncology. 2018. PMID: 29683227
-
Time trends in brain tumor incidence rates in Denmark, Finland, Norway, and Sweden, 1974-2003.J Natl Cancer Inst. 2009 Dec 16;101(24):1721-4. doi: 10.1093/jnci/djp415. J Natl Cancer Inst. 2009. PMID: 19959779
-
Psychotropic and anti-epileptic drug use, before and after surgery, among patients with low-grade glioma: a nationwide matched cohort study.BMC Cancer. 2021 Mar 8;21(1):248. doi: 10.1186/s12885-021-07939-w. BMC Cancer. 2021. PMID: 33685410 Free PMC article.
-
Self-reported workplace bullying and subsequent risk of diagnosed mental disorders and psychotropic drug prescriptions: A register-based prospective cohort study of 75,252 participants.J Affect Disord. 2025 Jan 15;369:1-7. doi: 10.1016/j.jad.2024.09.134. Epub 2024 Sep 22. J Affect Disord. 2025. PMID: 39317298
-
Psychotropic drug use among children and adolescents in the Nordic countries: a systematic review.Eur Child Adolesc Psychiatry. 2025 Mar;34(3):903-919. doi: 10.1007/s00787-024-02545-0. Epub 2024 Aug 8. Eur Child Adolesc Psychiatry. 2025. PMID: 39115685
References
-
- Ho VKY, Reijneveld JC, Enting RH, Bienfait HP, Robe P, Baumert BG, Visser O (2014) Changing incidence and improved survival of gliomas. Eur J Cancer 50:2309–2318. 10.1016/j.ejca.2014.05.019 - PubMed
-
- Posti JP, Bori M, Kauko T, Sankinen M, Nordberg J, Rahi M, Frantzén J, Vuorinen V, Sipilä JO (2015) Presenting symptoms of glioma in adults. Acta Neurol Scand 131:88–93. 10.1111/ane.12285 - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

