Progressive Myoclonus Epilepsy: Distinctive MRI Changes in Cerebellar and Motor Networks
- PMID: 40211586
- PMCID: PMC12172105
- DOI: 10.1002/acn3.70010
Progressive Myoclonus Epilepsy: Distinctive MRI Changes in Cerebellar and Motor Networks
Abstract
Objective: Progressive myoclonus epilepsy (PME) is a rare generalized epilepsy syndrome with a well-characterized genetic basis. The brain networks that are affected to give rise to the distinctive symptoms of PME are less well understood.
Methods: Eleven individuals with PME with a confirmed genetic diagnosis and 22 controls were studied. MRI included diffusion acquisition using 64 directions, b = 3000 s/mm2. Fixel-based analysis was used to identify white matter pathways with significant abnormality in structural connectivity, with subsequent tract segmentation and analysis. Region-of-interest and whole-brain volumetric analysis of T1-weighted images was performed. The relationship between structural connectivity measures and disease duration, and Unified Myoclonus Rating Scale was assessed.
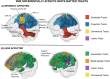
Results: Analysis of structural connectivity revealed significantly reduced fiber density and fiber bundle cross-section in white matter tracts in individuals with PME, with the most severe involvement of tracts within the cerebello-thalamo-cortical network, particularly the cerebello-thalamic, thalamo-cortical, cortico-thalamic, and corticospinal tracts, as well as the splenium of the corpus callosum. By comparison with these abnormalities, cortico-cortical association pathways were relatively preserved. There was reduced volume in the cerebellum, thalamus, brainstem, and mid-anterior corpus callosum.
Interpretation: Individuals with PME have atrophy and changes in fiber tracts that predominantly affect the cerebello-thalamic and motor systems, likely reflecting neuronal and axonal loss as part of a degenerative process. This imaging pattern is distinctive and accords well with the characteristic clinical, neuropathological, and neurophysiological features of the PMEs. The mechanism by which the PME genes affect these tracts is not yet known.
Keywords: MRI; motor networks; progressive myoclonus epilepsy.
© 2025 The Author(s). Annals of Clinical and Translational Neurology published by Wiley Periodicals LLC on behalf of American Neurological Association.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures


Similar articles
-
Hyperconnectivity and Connectome Gradient Dysfunction of Cerebello-Thalamo-Cortical Circuitry in Alzheimer's Disease Spectrum Disorders.Cerebellum. 2025 Feb 6;24(2):43. doi: 10.1007/s12311-025-01792-4. Cerebellum. 2025. PMID: 39913059
-
Characteristics of the cortico-striato-thalamo-cerebellar structural covariance network in Meige syndrome.Neuroscience. 2025 Aug 6;580:351-358. doi: 10.1016/j.neuroscience.2025.06.067. Epub 2025 Jul 1. Neuroscience. 2025. PMID: 40609622
-
The natural history of progressive myoclonus ataxia.Neurobiol Dis. 2024 Sep;199:106555. doi: 10.1016/j.nbd.2024.106555. Epub 2024 Jun 4. Neurobiol Dis. 2024. PMID: 38844245
-
White matter microstructure in children and adolescents with ADHD.Neuroimage Clin. 2022;33:102957. doi: 10.1016/j.nicl.2022.102957. Epub 2022 Feb 7. Neuroimage Clin. 2022. PMID: 35149304 Free PMC article.
-
Novel NUS1 variant in a Chinese patient with progressive myoclonus epilepsy: a case report and systematic review.Neurol Sci. 2023 Oct;44(10):3495-3498. doi: 10.1007/s10072-023-06851-4. Epub 2023 May 30. Neurol Sci. 2023. PMID: 37249665
References
-
- Berkovic S. F., Andermann F., Carpenter S., and Wolfe L. S., “Progressive Myoclonus Epilepsies: Specific Causes and Diagnosis,” New England Journal of Medicine 315, no. 5 (1986): 296–305. - PubMed
-
- Haltia M., Kristensson K., and Sourander P., “Neuropathological Studies in Three Scandinavian Cases of Progressive Myoclonus Epilepsy,” Acta Neurologica Scandinavica 45, no. 1 (1969): 63–77. - PubMed
-
- Cohen N. R., Hammans S. R., Macpherson J., and Nicoll J. A., “New Neuropathological Findings in Unverricht‐Lundborg Disease: Neuronal Intranuclear and Cytoplasmic Inclusions,” Acta Neuropathologica 121, no. 3 (2011): 421–427. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials
