Mechanistic insights into the sleep-glymphopathy-cerebral small vessel disease loop: implications for epilepsy pathophysiology and therapy
- PMID: 40212714
- PMCID: PMC11983519
- DOI: 10.3389/fnins.2025.1546482
Mechanistic insights into the sleep-glymphopathy-cerebral small vessel disease loop: implications for epilepsy pathophysiology and therapy
Abstract
Epilepsy is the second most common neurological disorder and affects approximately 50 million people worldwide. Despite advances in antiepileptic therapy, about 30% of patients develop refractory epilepsy. Recent studies have shown sleep, glymphatic function, cerebral small vessel disease (CSVD), and epilepsy are interrelated by sharing a multidirectional relationship in influencing their severity and progression. Sleep plays a vital role in brain homeostasis and promotes glymphatic clearance responsible for the removal of metabolic wastes and neurotoxic substances from the brain. Disrupted sleep is a common feature in epilepsy and can lead to impairment in glymphatic efficiency or glymphopathy, promoting neuroinflammation and accrual of epileptogenic factors. CSVD, occurring in up to 60% of the aging population, further exacerbates neurovascular compromise and neurodegeneration by increasing seizure susceptibility and worsening epilepsy outcomes. This narrative review aims to discuss the molecular and pathophysiological inter-relationships between these factors, providing a new framework that places glymphopathy and CSVD as contributors to epileptogenesis in conditions of sleep disruption. We propose an integrative model wherein the glymphopathy and vascular insufficiency interact in a positive feedback loop of sleep disruption and increased seizure vulnerability mediated by epileptic activity. Acknowledging these interactions has significant impacts on both research and clinical practice. Targeting sleep modulation, glymphatic function, and cerebrovascular health presents a promising avenue for therapeutic intervention. Future research should focus on developing precision medicine approaches that integrate neuro-glial-vascular mechanisms to optimize epilepsy management. Clinically, addressing sleep disturbances and CSVD in epilepsy patients may improve treatment effectiveness, reduce seizure burden, and improve overall neurological outcomes. This framework highlights the need for interdisciplinary approaches to break the vicious cycle of epilepsy, sleep disturbance, and cerebrovascular pathology, paving the way for innovative treatment paradigms.
Keywords: cerebral small vessel disease; epilepsy; glymphatic system; sleep; therapy.
Copyright © 2025 Hein, Al-Zaghal, Muhammad Ghazali, Jaffer, Abdul Hamid, Mehat, Che Ramli and Che Mohd Nassir.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
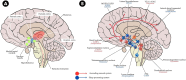
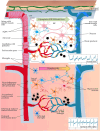
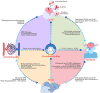
References
Publication types
LinkOut - more resources
Full Text Sources

