Prospective Study of Patients Treated with Palliative Radiation Therapy While on Immunotherapy
- PMID: 40213311
- PMCID: PMC11982977
- DOI: 10.1016/j.adro.2025.101741
Prospective Study of Patients Treated with Palliative Radiation Therapy While on Immunotherapy
Abstract
Purpose: To prospectively document the outcomes of patients treated with palliative radiation therapy (RT) who are receiving immunotherapy.
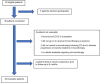
Methods and materials: Patients with advanced cancer receiving or planning to commence immunotherapy within 28 days who were referred for palliative RT at our center between January 2017 and September 2019 were screened for participation in this prospective observational study. Demographic and treatment data, along with patient-reported outcomes (PROs) using the Edmonton Symptom Assessment Scale for cancer, were collected at baseline, after 1 month, and then every 3 months for up to 1 year or until death. RT dose and fractionation were at the discretion of the treating radiation oncologist. Immunotherapy was given as per the standard of care protocol. The primary outcome was 3-month toxicity. Secondary outcomes included response evaluation criteria in solid tumors version 1.1 (RECIST v1.1) response on computed tomography scan performed 1, 3, and 6 months post-RT. The feasibility of enhancing PRO compliance using caregiver-aided PROs and virtual PRO collection was explored.
Results: Thirty-nine patients who received 50 courses of palliative RT (most often for pain) and who also received immunotherapy within 28 days of RT were evaluated for toxicity at 3 months post-RT. The most common primary cancer was non-small cell lung cancer (38%), followed by melanoma (36%). The most common RT dose was 20 Gy in 5 fractions (42%). 87% of patients (34/39) received a programmed cell death protein 1 inhibitor alone. An interval of <14 days between RT and immunotherapy. No grade 3 or higher toxicity was attributable to combined treatment. The median survival for the cohort was 11 months. At 3 months, 26 patients had imaging available for RECIST v1.1; 14 of 26 (54%) had an in-field response, and 3 of 26 (12%) had stable disease (with mixed out-of-field response). Compliance with PROs was 79% (31/39) at 1 month and 69% (27/39) at 3 months. Ten of the 31 patients (32%) and 11 of 31 patients (41%) used caregiver-aided PRO collection.
Conclusions: Palliative RT appears safe in patients receiving immunotherapy with no apparent increase in toxicity because of the combination. Responses out of irradiated volumes were no better than expected than with immunotherapy alone. Caregiver-aided PROs improved compliance with PRO data collection and were feasible.
© 2025 The Authors.
Conflict of interest statement
Andrew Bang reports institutional financial support from the BC Cancer Foundation for investigator-initiated study and honorarium (presentation fees) from AstraZeneca. Andrea Bezjak reports receiving an honorarium from AstraZeneca for serving as an advisory board member for lung cancer and as a board member for the International Association for Studying Lung Cancer from 2019 to 2023. Laura A. Dawson has received institutional support from Merck for the ITT clinical trial, a licensing agreement for software from Raysearch, and an honorarium from AstraZeneca. Laura A. Dawson also voluntarily served as President and Chair of ASTRO. Other authors have nothing to disclose.
Figures
Similar articles
-
Fostering efficacy of anti-PD-1-treatment: Nivolumab plus radiotherapy in advanced non-small cell lung cancer - study protocol of the FORCE trial.BMC Cancer. 2019 Nov 8;19(1):1074. doi: 10.1186/s12885-019-6205-0. BMC Cancer. 2019. PMID: 31703637 Free PMC article. Clinical Trial.
-
Palliative radiotherapy for children: Symptom response and treatment-associated toxicity according to radiation therapy dose and fractionation.Pediatr Blood Cancer. 2023 Apr;70(4):e30195. doi: 10.1002/pbc.30195. Epub 2023 Jan 15. Pediatr Blood Cancer. 2023. PMID: 36642970 Free PMC article.
-
High-dose irradiation in combination with non-ablative low-dose radiation to treat metastatic disease after progression on immunotherapy: Results of a phase II trial.Radiother Oncol. 2021 Sep;162:60-67. doi: 10.1016/j.radonc.2021.06.037. Epub 2021 Jul 5. Radiother Oncol. 2021. PMID: 34237343 Free PMC article. Clinical Trial.
-
Pembrolizumab with or without radiotherapy for metastatic non-small-cell lung cancer: a pooled analysis of two randomised trials.Lancet Respir Med. 2021 May;9(5):467-475. doi: 10.1016/S2213-2600(20)30391-X. Epub 2020 Oct 20. Lancet Respir Med. 2021. PMID: 33096027 Clinical Trial.
-
Palliative extracranial radiotherapy in patients receiving immunotherapy for non-small cell lung cancer: a narrative review.Transl Cancer Res. 2023 Jan 30;12(1):163-176. doi: 10.21037/tcr-22-1969. Epub 2022 Dec 21. Transl Cancer Res. 2023. PMID: 36760380 Free PMC article. Review.
References
-
- Weber J.S., D'Angelo S.P., Minor D., et al. Nivolumab versus chemotherapy in patients with advanced melanoma who progressed after anti-CTLA-4 treatment (CheckMate 037): A randomized, controlled, open-label, phase 3 trial. Lancet Oncol. 2015;16:375–384. - PubMed
-
- Butts C., Socinski M.A., Mitchell P.L., et al. Tecemotide (L-BLP25) versus placebo after chemoradiotherapy for stage III non-small-cell lung cancer (START): A randomised, double-blind, phase 3 trial. Lancet Oncol. 2014;15:59–68. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous