Integrating inflammation, nutrition, and immunity: the CALLY index as a prognostic tool in digestive system cancers - a systematic review and meta-analysis
- PMID: 40217204
- PMCID: PMC11992890
- DOI: 10.1186/s12885-025-14074-3
Integrating inflammation, nutrition, and immunity: the CALLY index as a prognostic tool in digestive system cancers - a systematic review and meta-analysis
Abstract
Background: Digestive system cancers remain a leading cause of cancer-related mortality globally, underscoring the need for reliable prognostic tools. The C-reactive protein-Albumin-Lymphocyte (CALLY) index, which reflects inflammation, nutrition, and immunity, has shown potential in predicting survival. However, comprehensive evaluations of its role in digestive system cancers are still limited.
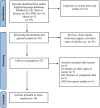
Methods: A meta-analysis of English-language studies from online databases was performed to assess the prognostic value of the CALLY index. Pooled hazard ratios (HRs) were calculated for overall survival (OS), disease-free survival (DFS), recurrence-free survival (RFS), and cancer-specific survival (CSS).
Results: A total of eighteen articles (19 studies, encompassing 7,951 patients) were included. A lower CALLY index was significantly associated with poorer outcomes across all survival endpoints. The pooled HR for OS was 1.973 (95% CI: 1.734-2.244), with HRs for DFS, RFS, and CSS being 2.093 (95% CI: 1.682-2.604), 1.462 (95% CI: 1.292-1.654), and 2.456 (95% CI: 1.887-3.221), respectively (all P < 0.001). Subgroup analyses for OS demonstrated consistent prognostic significance across various treatment strategies, cancer types, cutoff values, sample sizes, and regions. Notably, the CALLY index was a strong predictor of OS in surgical patients (HR = 2.014, 95% CI: 1.794-2.260, P < 0.001). Sensitivity analyses validated the robustness of these findings, with minimal publication bias (Egger's test P = 0.053).
Conclusions: The CALLY index serves as a cost-effective and reliable biomarker for predicting prognosis in digestive system cancers. Its utility as a pre-treatment risk stratification tool, which integrates key factors of inflammation, nutrition, and immunity, renders it valuable for guiding clinical decision-making.
Keywords: CALLY index; Digestive system cancers; Meta-analysis; Prognostic biomarker.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: As the data utilized in this study were derived exclusively from publicly available databases, ethical approval and informed consent were not required. Consent for publication: Not applicable. Competing interests: The authors declare no competing interests.
Figures




Similar articles
-
Prognostic and clinicopathological significance of C-reactive protein-albumin-lymphocyte(CALLY) in patients with digestive system neoplasms: a systematic review and meta-analysis.World J Surg Oncol. 2025 Apr 2;23(1):114. doi: 10.1186/s12957-025-03779-1. World J Surg Oncol. 2025. PMID: 40176025 Free PMC article.
-
Pan-immune-inflammation value as a novel prognostic biomarker for digestive system cancers: a meta-analysis.World J Surg Oncol. 2024 Nov 20;22(1):306. doi: 10.1186/s12957-024-03595-z. World J Surg Oncol. 2024. PMID: 39563378 Free PMC article.
-
Clinical usefulness of C-reactive protein-albumin-lymphocyte (CALLY) index as a prognostic biomarker in patients undergoing surgical resection of pancreatic cancer.Langenbecks Arch Surg. 2024 Oct 21;409(1):317. doi: 10.1007/s00423-024-03512-8. Langenbecks Arch Surg. 2024. PMID: 39432010
-
The prognostic value of systemic inflammation response index in digestive system carcinomas: a systematic review and meta-analysis.BMC Gastroenterol. 2025 Jan 24;25(1):34. doi: 10.1186/s12876-025-03635-2. BMC Gastroenterol. 2025. PMID: 39856542 Free PMC article.
-
Association between C-reactive protein-albumin-lymphocyte (CALLY) index and overall survival in patients with colorectal cancer: From the investigation on nutrition status and clinical outcome of common cancers study.Front Immunol. 2023 Mar 30;14:1131496. doi: 10.3389/fimmu.2023.1131496. eCollection 2023. Front Immunol. 2023. PMID: 37063910 Free PMC article.
References
-
- Li Q, Xia C, Li H, Yan X, Yang F, Cao M, et al. Disparities in 36 cancers across 185 countries: secondary analysis of global cancer statistics. Front Med. 2024;18(5):911–20. 10.1007/s11684-024-1058-6. - PubMed
-
- Shen L, Chen Z, Zhang Z, Wu Y, Ren Y, Li Y, et al. Clinical efficacy of taxol plus platinum (TP) chemotherapy combined with delayed administration of PD-1 inhibitors in patients with locally advanced, recurrent or metastatic esophageal squamous cell carcinoma: A retrospective study. Drug Des Devel Ther. 2024;18:2761–73. 10.2147/DDDT.S455248. - PMC - PubMed
-
- Skapinker E, Aucoin EB, Kombargi HL, Yaish AM, Li Y, Baghaie L, et al. Contemporaneous inflammatory, angiogenic, fibrogenic, and angiostatic cytokine profiles of the Time-to-Tumor development by cancer cells to orchestrate tumor neovascularization, progression, and metastasis. Cells. 2024;13(20):1739. 10.3390/cells13201739. - PMC - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials

