Combined Treatment With Lipoprotein Apheresis and Hemodialysis in Patients With Severe Cardiovascular Disease, High Lipoprotein(a) and End Stage Renal Disease
- PMID: 40217551
- PMCID: PMC11992239
- DOI: 10.1002/jca.70020
Combined Treatment With Lipoprotein Apheresis and Hemodialysis in Patients With Severe Cardiovascular Disease, High Lipoprotein(a) and End Stage Renal Disease
Abstract
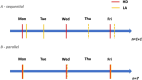
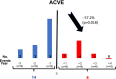
Elevated Lipoprotein(a) (Lp(a)) is a known independent cardiovascular risk factor. Lp(a) Lipoprotein Apheresis (LA) substantially reduces the number of cardiovascular events. The effect of LA treatment in hemodialysis (HD) patients remains unknown. Retrospective analysis of nine patients undergoing LA and HD. Cardiovascular risk factors and the efficacy of treatment were assessed. Adverse cardiac or vascular events (ACVE) were recorded. Median (range) years on HD were 4.2 (1.5 to 23.6) years and median years on LA were 4.0 (1.6 to 12.4) years. Before initiation of LA, median (range) Lp(a) level was 242.67 (164.0 to 400.10) nmol/L and mean LDL-C level (±SD) 2.49 (±1.14) mmol/L. Under treatment, mean acute reduction rates, comparing concentrations before and after LA sessions, were 64.15 (±5.45)% for Lp(a) and 57.26 (±7.93)% for LDL-C. Before initiation of LA, 14 ACVE occurred; after initiation, only 6 (57.2% reduction rate). In this small cohort, LA appears to be effective in reducing ACVE in patients on HD with elevated Lp(a) levels. Further studies are needed to evaluate the effect of LA on cardiovascular outcomes in dialysis patients.
Keywords: ACVE; dialysis; lipid disorder; lipoprotein apheresis; lipoprotein(a).
© 2025 The Author(s). Journal of Clinical Apheresis published by Wiley Periodicals LLC.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures

Similar articles
-
Cardiovascular events in patients with familial hypercholesterolemia and hyperlipoproteinaemia (a): Indications for lipoprotein apheresis in Poland.J Clin Apher. 2021 Jun;36(3):370-378. doi: 10.1002/jca.21872. Epub 2021 Jan 2. J Clin Apher. 2021. PMID: 33386762
-
Long-term lipoprotein apheresis reduces cardiovascular events in high-risk patients with isolated lipoprotein(a) elevation.J Clin Lipidol. 2024 Sep-Oct;18(5):e738-e745. doi: 10.1016/j.jacl.2024.04.134. Epub 2024 Apr 27. J Clin Lipidol. 2024. PMID: 38908966
-
Lipoprotein apheresis for lipoprotein(a) and cardiovascular disease.J Clin Lipidol. 2019 Nov-Dec;13(6):894-900. doi: 10.1016/j.jacl.2019.09.010. Epub 2019 Sep 21. J Clin Lipidol. 2019. PMID: 31753721
-
Current insights into the German lipoprotein apheresis standard: PCSK9-inhibitors, lipoprotein apheresis or both?Atheroscler Suppl. 2017 Nov;30:44-49. doi: 10.1016/j.atherosclerosissup.2017.05.005. Epub 2017 Jun 1. Atheroscler Suppl. 2017. PMID: 29096860 Review.
-
Lipoprotein(a)-apheresis in the light of new drug developments.Atheroscler Suppl. 2017 Nov;30:38-43. doi: 10.1016/j.atherosclerosissup.2017.05.025. Epub 2017 May 31. Atheroscler Suppl. 2017. PMID: 29096859 Review.
References
-
- Sarnak M. J., Levey A. S., Schoolwerth A. C., et al., “Kidney Disease as a Risk Factor for Development of Cardiovascular Disease: A Statement From the American Heart Association Councils on Kidney in Cardiovascular Disease, High Blood Pressure Research, Clinical Cardiology, and Epidemiology and Prevention,” Circulation 108, no. 17 (2003): 2154–2169. - PubMed
-
- Foley R. N., Parfrey P. S., and Sarnak M. J., “Clinical Epidemiology of Cardiovascular Disease in Chronic Renal Disease,” American Journal of Kidney Diseases 32, no. 5 Suppl 3 (1998): S112–S119. - PubMed
-
- Webster A. C., Nagler E. V., Morton R. L., and Masson P., “Chronic Kidney Disease,” Lancet 389, no. 10075 (2017): 1238–1252. - PubMed
-
- Herzog C. A., Ma J. Z., and Collins A. J., “Poor Long‐Term Survival After Acute Myocardial Infarction Among Patients on Long‐Term Dialysis,” New England Journal of Medicine 339, no. 12 (1998): 799–805. - PubMed
-
- Kwan B. C., Kronenberg F., Beddhu S., and Cheung A. K., “Lipoprotein Metabolism and Lipid Management in Chronic Kidney Disease,” Journal of the American Society of Nephrology 18, no. 4 (2007): 1246–1261. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

