Perioperative Outcomes and Trends of Surgical Correction of Male Urethral Strictures: Results from the GRAND Study
- PMID: 40217622
- PMCID: PMC11989686
- DOI: 10.3390/jcm14072171
Perioperative Outcomes and Trends of Surgical Correction of Male Urethral Strictures: Results from the GRAND Study
Abstract
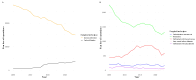
Background: While various techniques for the surgical correction of urethral strictures exist, data on their trends and perioperative outcomes are limited. Methods: Data from the German Nationwide Inpatient Data (GRAND) registry (2005-2023) were used to estimate the trends, baseline characteristics, and perioperative outcomes of the surgical techniques for urethral stricture correction. Results: A total of 500,937 patients underwent surgery. Internal urethrotomy was the most frequently performed procedure (n = 413,095, 82%), followed by urethral dilatation (n = 39,619, 8%), meatoplasty (n = 30,774, 6%), urethroplasty with buccal mucosa (n = 12,351, 2%), urethral excision with primary anastomosis (n = 3428, 0.7%), urethroplasty with preputial skin (n = 1585, 0.3%), and drug-coated balloon dilatation (n = 85, <0.1%). In recent years, internal urethrotomy declined; urethroplasty was relatively stable, and drug-coated balloon dilatation emerged as a promising treatment modality. Internal urethrotomy and urethral dilatation were predominantly performed in older patients (median age of 71 years), while urethroplasty was performed in younger (56 years). Preputial skin urethroplasty had a shorter hospital stay compared to buccal mucosa (-0.4 days, p = 0.02), with no significant differences in transfusion or sepsis rates. Conclusions: Internal urethrotomy remains the most frequently used technique despite declining utilization. Preputial skin urethroplasty presents similar perioperative outcomes compared to buccal mucosa urethroplasty.
Keywords: internal urethrotomy; perioperative outcomes; surgical trends; urethral strictures; urethroplasty.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
References
-
- Latini J.M., McAninch J.W., Brandes S.B., Chung J.Y., Rosenstein D. SIU/ICUD Consultation On Urethral Strictures: Epidemiology, etiology, anatomy, and nomenclature of urethral stenoses, strictures, and pelvic fracture urethral disruption injuries. Urology. 2014;83((Suppl. 3)):S1–S7. doi: 10.1016/j.urology.2013.09.009. - DOI - PubMed
-
- Patel H.V., Li K.D., Rourke K.F., Smith T.G., Voelzke B.B., Myers J.B., Broghammer J.A., Alsikafi N.F., Buckley J.C., Zhao L.C., et al. The Impact of Social Deprivation on Anterior Urethral Stricture Recurrence After Urethroplasty: A Trauma and Urologic Reconstructive Network of Surgeons Analysis. J. Urol. 2024;212:882–890. doi: 10.1097/JU.0000000000004188. - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources