Remnant Cholesterol Levels at Diagnosis May Predict Acute Coronary Syndrome Occurrence During Follow-Up in Patients with Antineutrophil Cytoplasmic Antibody-Associated Vasculitis
- PMID: 40217710
- PMCID: PMC11989813
- DOI: 10.3390/jcm14072260
Remnant Cholesterol Levels at Diagnosis May Predict Acute Coronary Syndrome Occurrence During Follow-Up in Patients with Antineutrophil Cytoplasmic Antibody-Associated Vasculitis
Abstract
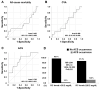
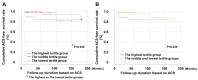
Background/Objectives: Previous studies have revealed the predictive potential of remnant cholesterol (RC) for acute coronary syndrome (ACS) occurrence in the general population. However, whether this association applies to patients with antineutrophil cytoplasmic antibody-associated vasculitis (AAV), in which a lipid paradox exists, remains unclear. We investigated whether RC levels at diagnosis could predict ACS occurrence during follow-up in patients with AAV. Methods: This study included 139 patients with AAV. ACS was defined as ST-elevation myocardial infarction (STEMI), non-STEMI, or unstable angina occurring after AAV diagnosis. RC levels were calculated as (total cholesterol)-(low-density lipoprotein cholesterol)-(high-density lipoprotein cholesterol). Patients were categorised into three groups by RC tertiles: highest (≥26.2 mg/dL), middle (19.1-26.1 mg/dL), and lowest (≤19.0 mg/dL) tertile groups. Results: The median age of the 139 patients (male, 31.7%) was 58.0 years. During follow-up, six, two, and one patients were diagnosed with ACS in the highest, middle, and lowest tertile groups, respectively. Patients in the highest tertile group exhibited a significantly lower ACS-free survival rate than those in the lowest tertile (p = 0.030). In the multivariable Cox hazards model, male sex (hazard ratio [HR] 9.054, 95% confidence interval [CI] 1.786-45.910), Birmingham vasculitis activity score (HR 1.147, 95% CI 1.033-1.274), and the highest tertile of RC levels (HR 10.818, 95% CI 1.867-62.689) were significantly and independently associated with ACS occurrence during follow-up in patients with AAV. Conclusions: Our findings indicate that RC levels at diagnosis may predict ACS occurrence during follow-up in patients with AAV, regardless of the traditional cardiovascular risk factors.
Keywords: acute coronary syndrome; antineutrophil cytoplasmic antibody; predict; remnant cholesterol; vasculitis.
Conflict of interest statement
The authors declare no conflicts of interest. The funders had no role in the design of the study; in the collection, analyses, or interpretation of data; in the writing of the manuscript; or in the decision to publish the results.
Figures

Similar articles
-
Triglyceride and Glucose Index Predicts Acute Coronary Syndrome in Patients with Antineutrophil Cytoplasmic Antibody-Associated Vasculitis.Diagnostics (Basel). 2022 Jun 17;12(6):1486. doi: 10.3390/diagnostics12061486. Diagnostics (Basel). 2022. PMID: 35741296 Free PMC article.
-
The monocyte-to-high-density lipoprotein-cholesterol ratio at diagnosis is associated with cerebrovascular accident during follow-up in patients with antineutrophil cytoplasmic antibody-associated vasculitis.J Rheum Dis. 2024 Jul 1;31(3):151-159. doi: 10.4078/jrd.2024.0001. Epub 2024 Mar 12. J Rheum Dis. 2024. PMID: 38957360 Free PMC article.
-
Acute coronary syndrome in antineutrophil cytoplasmic antibody-associated vasculitis: a Korean single-centre cohort study.J Rheum Dis. 2023 Apr 1;30(2):106-115. doi: 10.4078/jrd.2023.0002. Epub 2023 Mar 17. J Rheum Dis. 2023. PMID: 37483476 Free PMC article.
-
Atherogenic index of plasma predicts cerebrovascular accident occurrence in antineutrophil cytoplasmic antibody-associated vasculitis.Lipids Health Dis. 2020 Aug 14;19(1):184. doi: 10.1186/s12944-020-01360-1. Lipids Health Dis. 2020. PMID: 32799861 Free PMC article.
-
The residual risk of inflammation and remnant cholesterol in acute coronary syndrome patients on statin treatment undergoing percutaneous coronary intervention.Lipids Health Dis. 2024 Jun 7;23(1):172. doi: 10.1186/s12944-024-02156-3. Lipids Health Dis. 2024. PMID: 38849939 Free PMC article.
References
-
- Jennette J.C., Falk R.J., Bacon P.A., Basu N., Cid M.C., Ferrario F., Flores-Suarez L.F., Gross W.L., Guillevin L., Hagen E.C., et al. 2012 revised international chapel hill consensus conference nomenclature of vasculitides. Arthritis Rheum. 2013;65:1–11. - PubMed
-
- Watts R., Lane S., Hanslik T., Hauser T., Hellmich B., Koldingsnes W., Mahr A., Segelmark M., Cohen-Tervaert J.W., Scott D. Development and validation of a consensus methodology for the classification of the anca-associated vasculitides and polyarteritis nodosa for epidemiological studies. Ann. Rheum. Dis. 2007;66:222–227. - PMC - PubMed
-
- Suppiah R., Robson J.C., Grayson P.C., Ponte C., Craven A., Khalid S., Judge A., Hutchings A., Merkel P.A., Luqmani R.A., et al. 2022 american college of rheumatology/european alliance of associations for rheumatology classification criteria for microscopic polyangiitis. Ann. Rheum. Dis. 2022;81:321–326. - PubMed
-
- Robson J.C., Grayson P.C., Ponte C., Suppiah R., Craven A., Judge A., Khalid S., Hutchings A., Watts R.A., Merkel P.A., et al. 2022 american college of rheumatology/european alliance of associations for rheumatology classification criteria for granulomatosis with polyangiitis. Ann. Rheum. Dis. 2022;81:315–320. - PubMed
-
- Grayson P.C., Ponte C., Suppiah R., Robson J.C., Craven A., Judge A., Khalid S., Hutchings A., Luqmani R.A., Watts R.A., et al. 2022 american college of rheumatology/european alliance of associations for rheumatology classification criteria for eosinophilic granulomatosis with polyangiitis. Ann. Rheum. Dis. 2022;81:309–314. doi: 10.1136/annrheumdis-2021-221794. - DOI - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources

