80N as the Optimal Assistive Threshold for Wearable Exoskeleton-Mediated Gait Rehabilitation in Parkinson's Disease: A Prospective Biomarker Validation Study
- PMID: 40218096
- PMCID: PMC11989103
- DOI: 10.3390/healthcare13070799
80N as the Optimal Assistive Threshold for Wearable Exoskeleton-Mediated Gait Rehabilitation in Parkinson's Disease: A Prospective Biomarker Validation Study
Abstract
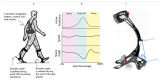
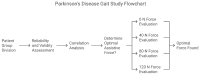
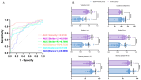
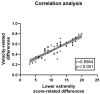
Background and Objectives: Robotic exoskeletons show potential in PD gait rehabilitation. But the optimal assistive force and its equivalence to clinical gold standard assessments are unclear. This study aims to explore the clinical equivalence of the lower limb exoskeleton in evaluating PD patients' gait disorders and find the best assistive force for clinical use. Methods: In this prospective controlled trial, 60 PD patients (Hoehn and Yahr stages 2-4) and 60 age-matched controls underwent quantitative gait analysis using a portable exoskeleton (Relink-ANK-1BM) at four assistive force levels (0 N, 40 N, 80 N, 120 N). Data from 57 patients and 57 controls were analyzed with GraphPad Prism 10. Different statistical tests were used based on data distribution. Results: ROC analysis showed that exoskeleton-measured velocity had the strongest power to distinguish PD patients from controls (AUC = 0.9198, p < 0.001). Other parameters also had high reliability and validity. There was a strong positive correlation between UPDRS-III lower extremity sub-score changes and gait velocity changes in PD patients (r = 0.8564, p < 0.001). The 80 N assistive force led to the best gait rehabilitation, with a 58% increase in gait velocity compared to unassisted walking (p < 0.001). Conclusions: 80 N is the optimal assistive threshold for PD gait rehabilitation. The wearable lower limb exoskeleton can be an objective alternative biomarker to UPDRS-III, enabling personalized home-based rehabilitation.
Keywords: Parkinson’s disease; gait disturbance; gait monitoring; lower limb exoskeletons; wearable device.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures

Similar articles
-
The Effectiveness and Safety of Exoskeletons as Assistive and Rehabilitation Devices in the Treatment of Neurologic Gait Disorders in Patients with Spinal Cord Injury: A Systematic Review.Global Spine J. 2016 Dec;6(8):822-841. doi: 10.1055/s-0036-1593805. Epub 2016 Nov 3. Global Spine J. 2016. PMID: 27853668 Free PMC article.
-
Assistive Mobility Control of a Robotic Hip-Knee Exoskeleton for Gait Training.Sensors (Basel). 2022 Jul 4;22(13):5045. doi: 10.3390/s22135045. Sensors (Basel). 2022. PMID: 35808539 Free PMC article.
-
Wearable rehabilitation exoskeletons of the lower limb: analysis of versatility and adaptability.Disabil Rehabil Assist Technol. 2023 May;18(4):392-406. doi: 10.1080/17483107.2020.1858976. Epub 2020 Dec 17. Disabil Rehabil Assist Technol. 2023. PMID: 33332159 Review.
-
Shape synthesis of an assistive knee exoskeleton device to support knee joint and rehabilitate gait.Disabil Rehabil Assist Technol. 2019 Jul;14(5):462-470. doi: 10.1080/17483107.2018.1493754. Epub 2018 Jul 25. Disabil Rehabil Assist Technol. 2019. PMID: 30044676
-
Systematic review on wearable lower-limb exoskeletons for gait training in neuromuscular impairments.J Neuroeng Rehabil. 2021 Feb 1;18(1):22. doi: 10.1186/s12984-021-00815-5. J Neuroeng Rehabil. 2021. PMID: 33526065 Free PMC article.
References
Grants and funding
LinkOut - more resources
Full Text Sources

