Adaptive radiotherapy for oropharyngeal cancer with daily adapt-to-shape workflow on 1.5 T MRI-linac: Preliminary outcomes and comparison with helical tomotherapy
- PMID: 40231325
- PMCID: PMC11995038
- DOI: 10.1016/j.ctro.2025.100950
Adaptive radiotherapy for oropharyngeal cancer with daily adapt-to-shape workflow on 1.5 T MRI-linac: Preliminary outcomes and comparison with helical tomotherapy
Abstract
Introduction: MR-linac could offer several advantages for radical radiochemotherapy (RCHT) in oropharyngeal squamous cell carcinoma (OPSCC) patients. Currently, only a few case series have been published and no comparison with other techniques have been performed.
Methods: Data of 34 consecutive patients treated from September 2022 to May 2024 at a single Institution with RCHT on Unity® MR-linac for OPSCC with daily adaptive radiotherapy (RT) according to the adapt-to-shape (ATS) workflow were prospectively analyzed. A comparative cohort of 34 patients with similar characteristics treated with helical treatment on Radixact® was retrieved.
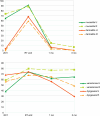
Results: Characteristics were well balanced across the two groups. Maximal toxicity grade ≥2 rate was borderline higher at RT end in MRI-linac group (p 0.049), but lower one month after RT (76.5 % vs 91.2 %; p = 0.257).Non-significantly lower rates of grade ≥2 xerostomia and dysgeusia were reported in Unity® group one and three months after RT. Higher rates of hospitalizations were reported in Radixact group at 20 fractions and at RT end (64.1 % vs 35.3 %; p = 0.015). Mean Karnofsky performance status (KPS) was higher in Unity group three months after RT (87.67 vs 83.87; p = 0.038).After a median follow up of 361.5 days, local complete response was reported for 93.6 % of patients treated with Unity® and 96.8 % of patients treated with Radixact®.
Conclusions: Results of this analysis support the feasibility of an ATS MR-linac workflow for RCHT in OPSCC. Compared with tomotherapy, treatment with Unity® resulted in significantly lower rates of hospitalization and higher KPS three months after RT. Grade 2 xerostomia and dysgeusia rates were non-significantly lower in Unity group. Optimal results in terms of local control were reported for both techniques.
Keywords: Adaptive radiotherapy; Head and neck; MR-guided radiotherapy; MR-linac; MRI-linac; Oropharyngeal; Oropharynx; Radiotherapy; Tomotherapy.
© 2025 The Author(s).
Conflict of interest statement
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Figures
Similar articles
-
First Experience and Prospective Evaluation on Feasibility and Acute Toxicity of Online Adaptive Radiotherapy of the Prostate Bed as Salvage Treatment in Patients with Biochemically Recurrent Prostate Cancer on a 1.5T MR-Linac.J Clin Med. 2022 Aug 9;11(16):4651. doi: 10.3390/jcm11164651. J Clin Med. 2022. PMID: 36012885 Free PMC article.
-
4D-MRI driven MR-guided online adaptive radiotherapy for abdominal stereotactic body radiation therapy on a high field MR-Linac: Implementation and initial clinical experience.Clin Transl Radiat Oncol. 2020 May 15;23:72-79. doi: 10.1016/j.ctro.2020.05.002. eCollection 2020 Jul. Clin Transl Radiat Oncol. 2020. PMID: 32490218 Free PMC article.
-
Treatment of Non-Hodgkin Lymphoma Involving Head and Neck Sites with a 1.5 T MR-Linac: Preliminary Results from a Prospective Observational Study.Hematol Rep. 2025 Mar 27;17(2):16. doi: 10.3390/hematolrep17020016. Hematol Rep. 2025. PMID: 40277840 Free PMC article.
-
Online Adaptive MR-Guided Ultrahypofractionated Radiotherapy of Prostate Cancer on a 1.5 T MR-Linac: Clinical Experience and Prospective Evaluation.Curr Oncol. 2024 May 9;31(5):2679-2688. doi: 10.3390/curroncol31050203. Curr Oncol. 2024. PMID: 38785484 Free PMC article.
-
MR-Guided Adaptive Radiotherapy for OAR Sparing in Head and Neck Cancers.Cancers (Basel). 2022 Apr 10;14(8):1909. doi: 10.3390/cancers14081909. Cancers (Basel). 2022. PMID: 35454816 Free PMC article. Review.
References
-
- Treatment decision is influenced by the stage and biologic characteristics of the disease, and firstline therapeutic options for non-metastatic disease consist of either definitive radio(chemo)therapy (RCT) or surgery possibly followed by adjuvant RCT.
-
- Machiels J.P., René Leemans C., Golusinski W., Grau C., Licitra L., Gregoire V. EHNS Executive Board. Squamous cell carcinoma of the oral cavity, larynx, oropharynx and hypopharynx: EHNS-ESMO-ESTRO Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann Oncol. 2020;31(11):1462–1475. doi: 10.1016/j.annonc.2020.07.011. - DOI - PubMed
LinkOut - more resources
Full Text Sources