Fetal heart quantification ultrasound technology for the quantitative analysis of fetal cardiac morphology and function in hypertensive disorders of pregnancy
- PMID: 40235737
- PMCID: PMC11994513
- DOI: 10.21037/qims-24-1553
Fetal heart quantification ultrasound technology for the quantitative analysis of fetal cardiac morphology and function in hypertensive disorders of pregnancy
Abstract
Background: Hypertensive disorders of pregnancy (HDP) are associated with adverse outcomes for both the mother and fetus, including impaired fetal cardiac development and function. Accurate assessment of fetal heart morphology and function is essential for the early detection and management of potential complications. This study investigated the clinical application value of fetal heart quantification (Fetal HQ) technology in evaluating the cardiac morphology and function in fetuses from pregnancies affected by HDP.
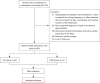
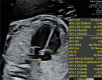
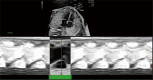
Methods: This prospective study examined 43 fetuses from singleton pregnancies complicated by HDP [mean gestational age (GA) 29.5±2.8 weeks] and 50 fetuses from normal pregnancies (mean GA 29.2±2.4 weeks). All participants underwent fetal ultrasonography from August 2023 to July 2024. Fetal HQ technology, incorporating two-dimensional speckle-tracking echocardiography (2D-STE) with quantitative analysis of cardiac segments, was used to assess heart size, shape, ventricular structure, contractility, and function.
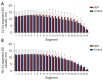
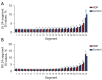
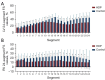
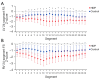
Results: The HDP group exhibited significantly altered maternal clinical characteristics, including higher maternal weight, BMI, and blood pressure. Fetal cardiac morphometry indicated that compared to the control group, the HDP group had larger left ventricular (LV) dimensions yet lower volumes but had smaller right ventricular (RV) dimensions. Notably, compared with the control group, the HDP group had a larger LV end-diastolic (ED) area (2.52±0.88 vs. 1.92±0.62 cm2; P<0.001) and ED length (2.35±0.37 vs. 1.89±0.33 cm; P<0.001) but a smaller LV ED volume (2.17±0.83 vs. 3.09±0.69 mL; P<0.001). Additionally, the HDP group exhibited significantly higher LV global strain (-30.53%±9.88% vs. -25.22%±8.33%; P=0.006), indicating altered cardiac function. The 24-segment analysis revealed notable alterations in ventricular geometry and function within the HDP group, with lower sphericity index (SI) and fractional shortening (FS) values across various segments of both ventricles. These findings closely align with the results of the Z score analysis, further highlighting the extent of cardiac dysfunction.
Conclusions: Fetal HQ technology effectively identified significant alterations in fetal heart structure and function in pregnancies complicated by HDP. These findings suggest that Fetal HQ is a useful tool for the early detection of fetal heart abnormalities and can facilitate timely intervention and accurate prognosis in affected pregnancies.
Keywords: Hypertensive disorders of pregnancy (HDP); fetal cardiac function; fetal cardiac morphology; fetal heart quantification technology (Fetal HQ technology); ultrasound imaging.
Copyright © 2025 AME Publishing Company. All rights reserved.
Conflict of interest statement
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://qims.amegroups.com/article/view/10.21037/qims-24-1553/coif). The authors have no conflicts of interest to declare.
Figures

Similar articles
-
Evaluation of fetal heart size, morphology and function with fetal growth restriction using fetal HQ.BMC Pregnancy Childbirth. 2024 Nov 14;24(1):751. doi: 10.1186/s12884-024-06966-2. BMC Pregnancy Childbirth. 2024. PMID: 39543509 Free PMC article.
-
Assessing Coarctation of the Aorta With Fetal Heart Quantification Technology.Matern Fetal Med. 2024 Jul 3;6(3):147-155. doi: 10.1097/FM9.0000000000000231. eCollection 2024 Jul. Matern Fetal Med. 2024. PMID: 40406281 Free PMC article.
-
Urgent neonatal balloon atrial septostomy in simple transposition of the great arteries: predictive value of fetal cardiac parameters.Ultrasound Obstet Gynecol. 2021 May;57(5):756-768. doi: 10.1002/uog.22164. Ultrasound Obstet Gynecol. 2021. PMID: 32730671
-
Pregnancy Complications Lead to Subclinical Maternal Heart Dysfunction-The Importance and Benefits of Follow-Up Using Speckle Tracking Echocardiography.Medicina (Kaunas). 2022 Feb 15;58(2):296. doi: 10.3390/medicina58020296. Medicina (Kaunas). 2022. PMID: 35208619 Free PMC article. Review.
-
Two-dimensional Speckle tracking echocardiography in Fetal Growth Restriction: a systematic review.Eur J Obstet Gynecol Reprod Biol. 2020 Nov;254:87-94. doi: 10.1016/j.ejogrb.2020.08.052. Epub 2020 Sep 2. Eur J Obstet Gynecol Reprod Biol. 2020. PMID: 32950891
Cited by
-
Assessment of fetal cardiac morphology and function in fetal growth restriction: insights from fetal heart quantification technology.Quant Imaging Med Surg. 2025 Aug 1;15(8):6713-6724. doi: 10.21037/qims-24-1957. Epub 2025 Jul 30. Quant Imaging Med Surg. 2025. PMID: 40785931 Free PMC article.
References
-
- Keskinkılıç B, Engin-Üstün Y, Sanisoğlu S, Şahin Uygur D, Keskin HL, Karaahmetoğlu S, Özcan A, Esen M, Alkan A, Kabasakal A, Şencan İ. Maternal mortality due to hypertensive disorders in pregnancy, childbirth, and the puerperium between 2012 and 2015 in Turkey: A nation-based study. J Turk Ger Gynecol Assoc 2017;18:20-5. 10.4274/jtgga.2016.0244 - DOI - PMC - PubMed
-
- Brown MA, Magee LA, Kenny LC, Karumanchi SA, McCarthy FP, Saito S, Hall DR, Warren CE, Adoyi G, Ishaku S, International Society for the Study of Hypertension in Pregnancy (ISSHP) . Hypertensive Disorders of Pregnancy: ISSHP Classification, Diagnosis, and Management Recommendations for International Practice. Hypertension 2018;72:24-43. 10.1161/HYPERTENSIONAHA.117.10803 - DOI - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
