Patterns of Co-infection of HPV52 With Other HPV Genotypes and Their Risks of Cervical Precancer and Carcinoma
- PMID: 40243019
- PMCID: PMC12004346
- DOI: 10.1002/jmv.70312
Patterns of Co-infection of HPV52 With Other HPV Genotypes and Their Risks of Cervical Precancer and Carcinoma
Abstract
Human papillomavirus 52 (HPV52) is the second most frequent HPV type in high-grade squamous intraepithelial lesion (HSIL) cases in China. However, few researchers have explored the co-infection of HPV52 with other HPV genotypes and their correlation with cervical lesions. In this study, 13,809 HPV52-positive patients visiting the Obstetrics and Gynecology Hospital of Fudan University from 2018 to 2023 were included in the first stage to investigate the risk of cervical lesions among different multiple infection patterns. Another 443 HPV52-positive patients were further included for sequence alignment and phylogenetic analysis. In the current study, the most common HPV52 dual-infection patterns were as follows: HPV16 + HPV52, HPV52 + HPV58, HPV52 + HPV53, and HPV52 + HPV81. Compared with HPV52 single infection, the risk of HSIL+ was increased in HPV16 + HPV52 (OR = 3.47, 95% CI: 2.56, 4.69) and HPV52 + HPV58 (OR = 1.99, 95% CI: 1.35, 2.92) groups. The most common triple-infection patterns were HPV16 + HPV52 + HPV53 and HPV52 + HPV53 + HPV81, followed by HPV52 + HPV53 + HPV58. HPV53 was the most common co-infection type with HPV52 in cases of triple or more multiple infections. However, compared with dual infection, the addition of HPV53 did not affect the risk of HSIL+. Two synonymous mutations, G207A (p = 0.029) and C1203T (p = 0.021), showed statistically significant differences in distribution between single and multiple infection groups. Our results demonstrated that HPV52 showed preferences for co-infection with HPV16, 585,381. HPV52 co-infection with HPV16 and HPV58 increased the risk of HSIL+, while co-infection with HPV53 did not increase the risk of HSIL+. Virus variants with certain mutations may be more susceptible to multiple infections.
Keywords: HPV52; L1 variants; cervical squamous intraepithelial lesions; multiple infections.
© 2025 The Author(s). Journal of Medical Virology published by Wiley Periodicals LLC.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
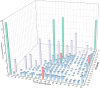
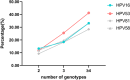


Similar articles
-
A 10-year Retrospective Analysis on HPV Genotype Switching in a Tertiary Center in China: Infection Characterization and Clinical Outcome.J Med Virol. 2025 Feb;97(2):e70193. doi: 10.1002/jmv.70193. J Med Virol. 2025. PMID: 39891593 Free PMC article.
-
Predicting the risk of high-grade precancerous cervical lesions based on high-risk HPV typing in Changsha China.BMC Womens Health. 2025 Jan 20;25(1):28. doi: 10.1186/s12905-025-03562-0. BMC Womens Health. 2025. PMID: 39833893 Free PMC article.
-
[Analysis of human papillomavirus subtype distribution and cervical lesion characteristics in a cancer hospital in Shenzhen City].Zhonghua Yu Fang Yi Xue Za Zhi. 2025 Apr 6;59(4):490-494. doi: 10.3760/cma.j.cn112150-20241004-00788. Zhonghua Yu Fang Yi Xue Za Zhi. 2025. PMID: 40176672 Chinese.
-
Prevalence and distribution of human papillomavirus genotypes in cervical intraepithelial neoplasia in China: a meta-analysis.Arch Gynecol Obstet. 2020 Dec;302(6):1329-1337. doi: 10.1007/s00404-020-05787-w. Epub 2020 Sep 10. Arch Gynecol Obstet. 2020. PMID: 32914222 Free PMC article. Review.
-
Human papillomavirus genotype distribution in low-grade cervical lesions: comparison by geographic region and with cervical cancer.Cancer Epidemiol Biomarkers Prev. 2005 May;14(5):1157-64. doi: 10.1158/1055-9965.EPI-04-0812. Cancer Epidemiol Biomarkers Prev. 2005. PMID: 15894666 Review.
References
-
- Sagasta A., Castillo P., Saco A., et al., “p16 Staining Has Limited Value in Predicting the Outcome of Histological Low‐Grade Squamous Intraepithelial Lesions of the Cervix,” Modern Pathology 29 (2016): 51–59. - PubMed
-
- Arbyn M., Tommasino M., Depuydt C., and Dillner J., “Are 20 Human Papillomavirus Types Causing Cervical Cancer?,” Journal of Pathology 234 (2014): 431–435. - PubMed
-
- Li M., Du X., Lu M., et al., “Prevalence Characteristics of Single and Multiple HPV Infections in Women With Cervical Cancer and Precancerous Lesions in Beijing, China,” Journal of Medical Virology 91 (2019): 473–481. - PubMed
-
- Sohrabi A., Hajia M., Jamali F., and Kharazi F., “Is Incidence of Multiple HPV Genotypes Rising in Genital Infections?,” Journal of Infection and Public Health 10 (2017): 730–733. - PubMed
MeSH terms
Substances
Supplementary concepts
LinkOut - more resources
Full Text Sources
Medical

