Clinical diagnosis and treatment of abdominal inflammatory myofibroblastic tumors
- PMID: 40244559
- PMCID: PMC12006656
- DOI: 10.1007/s12672-025-02343-3
Clinical diagnosis and treatment of abdominal inflammatory myofibroblastic tumors
Abstract
Objective: This study aims to summarize the clinicopathological characteristics, treatment methods, and prognosis of these patients. The goal is to enhance our understanding of the disease and provide insights for the standardized diagnosis and treatment of abdominal inflammatory myofibroblastic tumors(IMT).
Methods: This retrospective cohort study included clinical data of 26 patients with abdominal IMT admitted to the First Hospital of Jilin University between January 2015 and December 2023. The clinical manifestations, pathological features, treatment methods, and prognoses were analyzed.
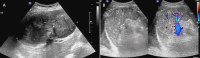
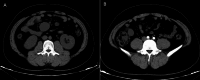
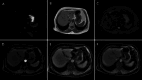
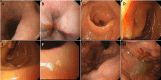
Results: Among 26 patients, 6 had hepatic IMT, 2 splenic IMT, and 1 abdominal wall IMT, all detected incidentally as painless masses during routine exams. Six patients with mesenteric IMT reported abdominal distension, pain, nausea, vomiting, and low-grade fever. Of five patients with gastric IMT, three had gastrointestinal bleeding, one had distension and fever, and one had dysphagia. Four small intestine cases included one asymptomatic and three with obstruction symptoms. The colon and rectal cases presented with intermittent hematochezia. Surgery was performed in 24 patients, and 2 with metastases received palliative therapy. During follow-up, five patients relapsed; three received palliative therapy, and two had surgery. At last follow-up, 20 patients were disease-free, 3 were living with tumors, and 3 had died.
Conclusions: Abdominal IMTs are rare, low-grade tumors with favorable prognoses. Pathological examination is essential for diagnosis, and surgery is the primary treatment. Adjuvant therapy depends on tumor location and risk factors. Close follow-up is necessary due to the potential for recurrence and metastasis.
Keywords: Abdominal tumors; Adjuvant therapy; Diagnosis; Inflammatory myofibroblastic tumor; Pathology; Surgery; Tumor location.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: This study has received approval from the Ethics Committee of the First Hospital of Jilin University (Approval number: 2024-1067) and informed consent has been duly obtained from both the patients and their families. Consent for publication: Not applicable. Competing interests: The authors declare no competing interests.
Figures

Similar articles
-
Therapeutic strategy and prognostic analysis of inflammatory myofibroblastic tumor in the head and neck: a retrospective study.PeerJ. 2025 Apr 18;13:e19315. doi: 10.7717/peerj.19315. eCollection 2025. PeerJ. 2025. PMID: 40260197 Free PMC article.
-
Inflammatory myofibroblastic tumor in children: diagnosis and treatment.J Pediatr Surg. 2001 Jun;36(6):908-12. doi: 10.1053/jpsu.2001.23970. J Pediatr Surg. 2001. PMID: 11381424 Review.
-
Abdominal inflammatory myofibroblastic tumor a clinicopathologic study with reappraisal of biologic behavior.J Pediatr Surg. 2011 Nov;46(11):2076-82. doi: 10.1016/j.jpedsurg.2011.07.009. J Pediatr Surg. 2011. PMID: 22075336
-
Abdominal inflammatory myofibroblastic tumour: Clinicopathological and molecular analysis of 20 cases, highlighting potential therapeutic targets.Histopathology. 2024 Apr;84(5):794-809. doi: 10.1111/his.15122. Epub 2023 Dec 28. Histopathology. 2024. PMID: 38155480
-
Computed tomographic features of inflammatory myofibroblastic tumour of the stomach in adult patients: An analysis of five multicentre cases with literature review.J Med Imaging Radiat Oncol. 2018 Dec;62(6):769-776. doi: 10.1111/1754-9485.12780. Epub 2018 Aug 3. J Med Imaging Radiat Oncol. 2018. PMID: 30076671 Review.
References
-
- Bansal A, Goyal S, Goyal A, Jana M. WHO classification of soft tissue tumours 2020: an update and simplified approach for radiologists. Eur J Radiol. 2021;143: 109937. - PubMed
-
- Mahajan P, Casanova M, Ferrari A, Fordham A, Trahair T, Venkatramani R. Inflammatory myofibroblastic tumor: molecular landscape, targeted therapeutics, and remaining challenges. Curr Probl Cancer. 2021;45: 100768. - PubMed
LinkOut - more resources
Full Text Sources
