Fecal microbiota transplantation for patients with ulcerative colitis: a systematic review and meta-analysis of randomized control trials
- PMID: 40246750
- PMCID: PMC12006273
- DOI: 10.1007/s10151-025-03113-7
Fecal microbiota transplantation for patients with ulcerative colitis: a systematic review and meta-analysis of randomized control trials
Abstract
Background: Fecal microbiota transplantation (FMT) has been shown to restore gut microbiome composition with an acceptable safety profile. FMT in inflammatory bowel disease, specifically ulcerative colitis (UC), has been investigated. We aimed to assess the efficacy of FMT in inducing UC remission.
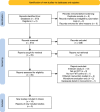
Methods: PubMed, Scopus, Google Scholar, and clinicaltrials.gov were searched for randomized control trials that assessed FMT in inducing UC remission. The primary outcome was combined clinical and endoscopic remission. Secondary outcomes were clinical remission, endoscopic remission, post-treatment overall adverse events, and colitis. Sensitivity analyses, meta-regression, bias assessment, and grading of certainty of evidence were performed.
Results: A total of 14 studies including 600 patients (55.8% male; median age 40.7 years) were assessed. FMT was used in 299 patients and associated with significantly higher odds of combined clinical and endoscopic remission (OR 2.25, 95% CI 1.54, 3.3; p < 0.0001), clinical remission (OR 2.02, 95% CI 1.4, 2.93; p = 0.0002), and endoscopic remission (OR 1.95, 95% CI 1.17, 3.28; p = 0.011). The odds of post-treatment overall adverse events (OR 1.24, 95% CI 0.79, 1.95; p = 0.34) and colitis (OR 0.85, 95% CI 0.52, 1.93; p = 0.512) were similar between groups. Compared with baseline, FMT was more effective when biologics (OR 2.71), steroids (OR 2.27), or methotrexate (OR 3.07) were used as pre-FMT treatment. Oral delivery of FMT (OR 3.15) and pooled donors (OR 3.32) led to higher odds of remission. On meta-regression, pooled donors and methotrexate pre-treatment were associated with an increased likelihood of remission.
Conclusions: FMT is promising in inducing UC remission. Administration of medical treatments before FMT may help achieve higher remission rates. Current evidence shows that oral delivery of FMT and multidonor FMT may confer better results.
Keywords: Fecal microbiota transplantation; Meta-analysis; Randomized control trials; Ulcerative colitis.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Conflict of interest: Dr. Wexner is a consultant for ActivSurgical, Arthrex, Baxter, Becton, Dickinson and Co, Glaxo Smith Kline, Intuitive Surgical, OstomyCure, Takeda, and Virtual Ports; has consulting agreements with stock options for consulting with GI View, OstomyCure, and Virtual Ports; is a member of the Data Safety Monitoring Board of JSR/WCG/ACI (chair), Polypoid (chair) and receives royalties from Intuitive Surgical, Karl Storz Endoscopy America Inc., and Unique Surgical Solutions, LLC. Dr. Emile is a consultant for Becton, Dickinson and Co. Ethical approval and informed consent: Ethics approval and informed consent were not required for this type of study (literature review).
Figures
References
-
- Nishida A, Inoue R, Inatomi O et al. (2018) Gut microbiota in the pathogenesis of inflammatory bowel disease. Clin J Gastroenterol 11:1–10. 10.1007/s12328-017-0813-5 - PubMed
-
- Ooijevaar RE, Terveer EM, Verspaget HW, Kuijper EJ, Keller JJ (2019) Clinical application and potential of fecal microbiota transplantation. Annu Rev Med 70:335–351. 10.1146/annurev-med-111717-122956. (Epub 2018 Nov 7 PMID: 30403550) - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical