Simvastatin mitigates ventilator-induced lung injury in mice with acute respiratory distress syndrome via a mechanism partly dependent on neutrophil extracellular traps
- PMID: 40247369
- PMCID: PMC12007243
- DOI: 10.1186/s40001-025-02544-0
Simvastatin mitigates ventilator-induced lung injury in mice with acute respiratory distress syndrome via a mechanism partly dependent on neutrophil extracellular traps
Abstract
Background: Mechanical ventilation (MV) is an essential life support for patients with acute respiratory distress syndrome (ARDS). However, mechanical ventilation in patients with ARDS can cause ventilator-induced lung injury (VILI). Simvastatin can alleviate acute lung injury by anti-inflammatory and enhancing endothelial barrier. The present study aimed to evaluate whether simvastatin could attenuate VILI in mice with ARDS.
Methods: Mice were randomized into six groups: the sham (S), LPS (L), MV (V), LPS/MV (LV), LPS/MV/simvastatin (MS) and LPS/MV/GSK484 (MG) groups. The mice in the L group received LPS but not ventilation, the mice in the V group received only MV, and the mice in the LV, MS and MG groups received LPS and MV. Additionally, MS group were treated with simvastatin, MG group were treated with GSK484, and the other mice were injected with saline, starting three days prior to mechanical ventilation. The PaO2/FiO2 ratio and wet‒dry weight ratio were calculated. Histopathological changes were observed, and injury scores were calculated. Inflammatory factor levels in the bronchoalveolar lavage fluid (BALF) were detected. Peptidylarginine deiminase 4 (PAD4), neutrophil elastase (NE) and citrullinated histone 3 (Cit-H3) in the lung tissue were detected, apoptosis were also evaluated.
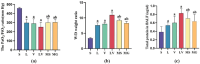
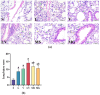
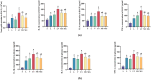
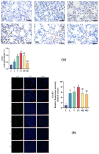
Results: All indices were improved in group S compared with the other groups. The lung injury score and wet‒dry weight ratio were lower, the PaO2/FiO2 ratio was greater, inflammatory factor levels in the BALF were lower, PAD4, NE, and Cit-H3 expression was lower, and apoptosis was decreased in the MS and MG groups compared with the LV group.
Conclusions: Simvastatin attenuated VILI in mice with ARDS, potentially via reductions in neutrophil extracellular traps (NETs) generation and apoptosis.
Keywords: Acute respiratory distress syndrome; Mechanical ventilation; Neutrophil extracellular traps; Simvastatin.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: This study was approved by the Laboratory Animal Committee of Qingdao Municipal Hospital (2021-118). Consent for publication: Not applicable. Competing interests: The authors declare no competing interests.
Figures


Similar articles
-
Alpha 1-antitrypsin for treating ventilator-associated lung injury in acute respiratory distress syndrome rats.Exp Lung Res. 2019 Sep;45(7):209-219. doi: 10.1080/01902148.2019.1642968. Epub 2019 Jul 26. Exp Lung Res. 2019. PMID: 31347410
-
Simvastatin Reduces NETosis to Attenuate Severe Asthma by Inhibiting PAD4 Expression.Oxid Med Cell Longev. 2023 Feb 2;2023:1493684. doi: 10.1155/2023/1493684. eCollection 2023. Oxid Med Cell Longev. 2023. PMID: 36778209 Free PMC article.
-
Endothelial Colony-forming Cells Attenuate Ventilator-induced Lung Injury in Rats with Acute Respiratory Distress Syndrome.Arch Med Res. 2018 Apr;49(3):172-181. doi: 10.1016/j.arcmed.2018.08.006. Epub 2018 Aug 14. Arch Med Res. 2018. PMID: 30119979
-
A long-lasting porcine model of ARDS caused by pneumonia and ventilator-induced lung injury.Crit Care. 2023 Jun 16;27(1):239. doi: 10.1186/s13054-023-04512-8. Crit Care. 2023. PMID: 37328874 Free PMC article. Review.
-
Renin-angiotensin-system, a potential pharmacological candidate, in acute respiratory distress syndrome during mechanical ventilation.Pulm Pharmacol Ther. 2019 Oct;58:101833. doi: 10.1016/j.pupt.2019.101833. Epub 2019 Aug 1. Pulm Pharmacol Ther. 2019. PMID: 31376462 Free PMC article. Review.
References
-
- Bellani G, Laffey JG, Pham T, Fan E, Brochard L, Esteban A, et al. Epidemiology, patterns of care, and mortality for patients with acute respiratory distress syndrome in intensive care units in 50 countries. JAMA. 2016;315(8):788–800. - PubMed
-
- Esteban A, Anzueto A, Alia I, Gordo F, Apezteguia C, Palizas F, et al. How is mechanical ventilation employed in the intensive care unit? An international utilization review. Am J Respir Crit Care Med. 2000;161(5):1450–8. - PubMed
-
- Tsushima K, Tatsumi K. Noninvasive mechanical ventilation and neutrophil elastase inhibitor: a new potential approaching to acute hypoxemic failure. J Crit Care. 2014;29(6):1124–5. - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

