Distinct features of three clinical subtypes in 533 patients with primary hypertrophic osteoarthropathy
- PMID: 40251683
- PMCID: PMC12007382
- DOI: 10.1186/s13023-025-03722-3
Distinct features of three clinical subtypes in 533 patients with primary hypertrophic osteoarthropathy
Abstract
Background: Primary hypertrophic osteoarthropathy (PHO) is a rare genetic disorder classified into clinical subtypes and genetic subtypes. Previous clinical studies have primarily focused on case reports and family analyses, largely characterizing the genetic subtypes. However, there remains a long-standing gap in understanding the characteristics of the different clinical subtypes of PHO. This study aimed to determine the distribution of the three clinical subtypes of PHO and compare their clinical characteristics using a large global sample.
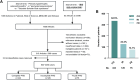
Methods: A systematic literature search was conducted in multiple databases to categorize cases into complete form (CO), incomplete form (IN), and fruste form (FR). Statistical analyses were performed to assess clinical differences in a retrospective study design.
Results: Males predominated across all subtypes, whereas females were most prevalent in IN patients (51.1%). IN patients had the highest family history rate (62.1%). Age at onset peaked in adolescence for CO and FR patients, while IN patients exhibited bimodal peaks in early childhood and adolescence. Congenital diseases were more frequent in IN patients (7.8%, P = 0.021), while CO patients had a higher prevalence of digestive system diseases (12.2%, P = 0.007). Urinary prostaglandin E2 (PGE2) and PGE Metabolite (PGEM) were consistently elevated in CO and FR patients. In IN patients, urinary PGE2 levels were also increased, but the urinary PGEM levels showed equal proportions of elevation and reduction. Genetic analysis revealed that solute carrier organic anion transporter family member 2A1 (SLCO2A1) mutations were predominant in CO (95 cases, 73.1%) and FR (22 cases, 57.9%) patients, whereas hydroxyprostaglandin dehydrogenase (HPGD) mutations were most frequently associated with IN (25 cases, 73.5%).
Conclusions: The three clinical subtypes of PHO exhibited distinct characteristics with no clear correlation between clinical and genetic subtypes. These findings highlighted the clinical significance of PHO typing and provided valuable insights for diagnosis, differential diagnosis and subtype-specific management strategies.
Keywords: Clinical subtypes; Genetic subtypes; Pachydermoperiostosis; Primary hypertrophic osteoarthropathy; Touraine-Solente-Gole syndrome.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: Not applicable. Consent for publication: Not applicable. Competing interests: The authors declare no competing interests.
Figures



Similar articles
-
Identification of mutations in the prostaglandin transporter gene SLCO2A1 and phenotypic comparison between two subtypes of primary hypertrophic osteoarthropathy (PHO): A single-center study.Bone. 2018 Jan;106:96-102. doi: 10.1016/j.bone.2017.09.015. Epub 2017 Sep 28. Bone. 2018. PMID: 28963081
-
Touraine-Solente-Gole syndrome: pathogenic variant in SLCO2A1 presented with polyarthralgia and digital clubbing.Pediatr Rheumatol Online J. 2023 May 24;21(1):48. doi: 10.1186/s12969-023-00831-w. Pediatr Rheumatol Online J. 2023. PMID: 37226222 Free PMC article.
-
Two novel mutations in the SLCO2A1 gene in a Chinese patient with primary hypertrophic osteoarthropathy.Gene. 2014 Jan 25;534(2):421-3. doi: 10.1016/j.gene.2013.10.051. Epub 2013 Nov 1. Gene. 2014. PMID: 24185079
-
Primary hypertrophic osteoarthropathy related gastrointestinal complication has distinctive clinical and pathological characteristics: two cases report and review of the literature.Orphanet J Rare Dis. 2019 Dec 26;14(1):297. doi: 10.1186/s13023-019-1264-5. Orphanet J Rare Dis. 2019. PMID: 31878983 Free PMC article.
-
Primary hypertrophic osteoarthropathy: genetics, clinical features and management.Front Endocrinol (Lausanne). 2023 Aug 29;14:1235040. doi: 10.3389/fendo.2023.1235040. eCollection 2023. Front Endocrinol (Lausanne). 2023. PMID: 37705574 Free PMC article. Review.
References
-
- Castori M, Sinibaldi L, Mingarelli R, et al. Pachydermoperiostosis: an update. Clin Genet. 2005;68(6):477–86. - PubMed
-
- Touraine A, Solente G, Gole L. Un syndrome osteodermopathique: La pachydermie plicaturee avec pachyperiostose des extremites. Presse Med. 1935;43:1820–4.
-
- Martinez-Lavin M. Hypertrophic osteoarthropathy. Best Pract Res Clin Rheumatol. 2020;34(3):101507. - PubMed
-
- Lucas Rocha M, Silvestre-Teixeira V. Secondary hypertrophic osteoarthropathy. N Engl J Med. 2024;390(13):1218. - PubMed
-
- Uppal S, Diggle CP, Carr IM, et al. Mutations in 15-hydroxyprostaglandin dehydrogenase cause primary hypertrophic osteoarthropathy. Nat Genet. 2008;40(6):789–93. - PubMed
MeSH terms
Substances
Grants and funding
- 2023zhyx-B10/Research Fund of Anhui Institute of translational medicine
- Outstanding Project of Jianghuai Talent Training Program in Anhui Province/Outstanding Project of Jianghuai Talent Training Program in Anhui Province
- 2023AH053163/the Key Scientific Research Foundation of the Education Department of Anhui Province
- 2023GQFY01/National Natural Science Foundation Incubation Program of The Second Affiliated Hospital of Anhui Medical University
- Clinical Medicine project of Anhui Medical University/Clinical Medicine project of Anhui Medical University
LinkOut - more resources
Full Text Sources
Miscellaneous

